Abstract
Purpose
Thyroid cancer is the most rapidly increasing cancer in the USA, affects a young, mostly female population, and has high survival. The aim of this study was to determine if there is an increased risk of reproductive system adverse events or pregnancy complications among women diagnosed with thyroid cancer under the age of 50.
Methods
Up to five female cancer-free individuals were matched to each female thyroid cancer survivor diagnosed before the age of 50 based on birth year, birth state, and follow-up time, within the Utah Population Database. Medical records were used to identify disease diagnoses stratified over three time periods: 0–1, > 1–5, and > 5–10 years after cancer diagnosis. Cox proportional hazards models were used to estimate hazard ratios (HR) with adjustment on matching factors, race, BMI, and Charlson Comorbidity Index.
Results
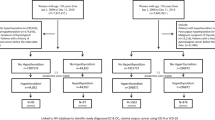
There were 1832 thyroid cancer survivors and 7921 matched individuals. Thyroid cancer survivors had higher rates of having multiple health conditions associated with the gynecological system (15.4% vs. 9.4%) and pregnancy (14.3% vs 9.5%) > 1–5 years after cancer diagnosis. Increased risks persisted > 5–10 years after cancer diagnosis for menopausal disorders (HR = 1.78, 99% CI = 1.37, 2.33) and complications related to pregnancy (HR = 2.13, 99% CI = 1.14, 3.98). Stratified analyses showed these risks remained increased across different treatment types.
Conclusions
There were significant risk increases in reproductive system and pregnancy complications among female thyroid cancer survivors within this study.
Implications for Cancer Survivors
Although radiation has been linked to reproductive risks in previous studies, we found risks were increased in patients regardless of treatment.

Similar content being viewed by others
References
Society AC. Cancer treatment & survivorship facts & figures 2016–2017. Atlanta: American Cancer Society; 2016.
Cancer of the Thyroid - Cancer Stat Facts. 2017. https://seer.cancer.gov/statfacts/html/thyro.html. Accessed February 2, 2017.
Key Statistics for Thyroid Cancer. American Cancer Society. 2017. https://www.cancer.org/cancer/thyroid-cancer/about/key-statistics.html. Accessed February 21, 2017.
Cancer of the Thyroid - SEER Stat Fact Sheets. 2016. http://seer.cancer.gov/statfacts/html/thyro.html. Accessed February 8, 2016.
McLeod DS, Sawka AM, Cooper DS. Controversies in primary treatment of low-risk papillary thyroid cancer. Lancet (London, England). 2013;381(9871):1046–57. https://doi.org/10.1016/s0140-6736(12)62205-3.
Fard-Esfahani A, Emami-Ardekani A, Fallahi B, Fard-Esfahani P, Beiki D, Hassanzadeh-Rad A, et al. Adverse effects of radioactive iodine-131 treatment for differentiated thyroid carcinoma. Nucl Med Commun. 2014;35(8):808–17. https://doi.org/10.1097/mnm.0000000000000132.
Wu JX, Young S, Ro K, Li N, Leung AM, Chiu HK, et al. Reproductive outcomes and nononcologic complications after radioactive iodine ablation for well-differentiated thyroid cancer. Thyroid. 2015;25(1):133–8. https://doi.org/10.1089/thy.2014.0343.
Banach R, Bartes B, Farnell K, Rimmele H, Shey J, Singer S, et al. Results of the thyroid cancer alliance international patient/survivor survey: psychosocial/informational support needs, treatment side effects and international differences in care. Hormones (Athens). 2013;12(3):428–38.
Overview - Utah Population Database - - Huntsman Cancer Institute - University of Utah Health Care - Salt Lake City, Utah. 2016. http://healthcare.utah.edu/huntsmancancerinstitute/research/updb/. Accessed May 10, 2016.
HCUP-US Tools & Software Page. 2016. https://www.hcup-us.ahrq.gov/toolssoftware/ccs/ccs.jsp. Accessed February 9, 2016.
Charlson ME, Pompei P, Ales KL, MacKenzie CR. A new method of classifying prognostic comorbidity in longitudinal studies: development and validation. J Chronic Dis. 1987;40(5):373–83.
Sawka AM, Lakra DC, Lea J, Alshehri B, Tsang RW, Brierley JD, et al. A systematic review examining the effects of therapeutic radioactive iodine on ovarian function and future pregnancy in female thyroid cancer survivors. Clin Endocrinol. 2008;69(3):479–90. https://doi.org/10.1111/j.1365-2265.2008.03222.x.
Sioka C, Kouraklis G, Zafirakis A, Manetou A, Dimakopoulos N. Menstrual cycle disorders after therapy with iodine-131. Fertil Steril. 2006;86(3):625–8. https://doi.org/10.1016/j.fertnstert.2006.02.081.
Sioka C, Fotopoulos A. Effects of I-131 therapy on gonads and pregnancy outcome in patients with thyroid cancer. Fertil Steril. 2011;95(5):1552–9. https://doi.org/10.1016/j.fertnstert.2011.01.017.
Souza Rosario PW, Alvarenga Fagundes T, Villas-Boas Fagundes AS, Barroso AL, Lamego Rezende L, Lanza Padrao E, et al. Ovarian function after radioiodine therapy in patients with thyroid cancer. Exp Clin Endocrinol Diabetes. 2005;113(6):331–3. https://doi.org/10.1055/s-2005-837666.
Rosario PW, Fagundes TA, Fagundes AV, Barraso AL, Rezende LL, Padrao EL, et al. Radioiodine therapy and age at menopause in patients with thyroid cancer. Clin Endocrinol. 2006;64(2):225–6. https://doi.org/10.1111/j.1365-2265.2005.02413.x.
Garsi JP, Schlumberger M, Rubino C, Ricard M, Labbe M, Ceccarelli C, et al. Therapeutic administration of 131I for differentiated thyroid cancer: radiation dose to ovaries and outcome of pregnancies. J Nucl Med. 2008;49(5):845–52. https://doi.org/10.2967/jnumed.107.046599.
Fard-Esfahani A, Hadifar M, Fallahi B, Beiki D, Eftekhari M, Saghari M, et al. Radioiodine treatment complications to the mother and child in patients with differentiated thyroid carcinoma. Hell J Nucl Med. 2009;12(1):37–40.
Ying H, Tang YP, Bao YR, Su XJ, Cai X, Li YH, et al. Maternal TSH level and TPOAb status in early pregnancy and their relationship to the risk of gestational diabetes mellitus. Endocrine. 2016;54(3):742–50. https://doi.org/10.1007/s12020-016-1022-6.
Ma J, Huang M, Wang L, Ye W, Tong Y, Wang H. Obesity and risk of thyroid cancer: evidence from a meta-analysis of 21 observational studies. Med Sci Monit. 2015;21:283–91. https://doi.org/10.12659/msm.892035.
Hadley EE, Discacciati A, Costantine MM, Munn MB, Pacheco LD, Saade GR, et al. Maternal obesity is associated with chorioamnionitis and earlier indicated preterm delivery among expectantly managed women with preterm premature rupture of membranes. J Matern Fetal Neonatal Med. 2017:1–8. https://doi.org/10.1080/14767058.2017.1378329.
Madan J, Chen M, Goodman E, Davis J, Allan W, Dammann O. Maternal obesity, gestational hypertension, and preterm delivery. J Matern Fetal Neonatal Med. 2010;23(1):82–8. https://doi.org/10.3109/14767050903258738.
American Thyroid Association. Childhood head & neck irradiation. 2014. https://www.thyroid.org/wp-content/uploads/patients/brochures/Head_Neck_Irradiation_brochure.pdf. Accessed 8 Jan 2018.
Funding
This work was supported by grants from the NCI (R03 CA159357; R21 CA185811), the Huntsman Cancer Institute, Cancer Control and Population Sciences Program (HCI Cancer Center Support Grant P30CA042014), and the NCRR grant, “Sharing Statewide Health Data for Genetic Research” (R01 RR021746, G. Mineau, PI) with additional support from the Utah State Department of Health and the University of Utah. We thank the Pedigree and Population Resource of the Huntsman Cancer Institute, University of Utah (funded in part by the Huntsman Cancer Foundation) for its role in the ongoing collection, maintenance, and support of the Utah Population Database (UPDB). We thank the University of Utah Center for Clinical and Translational Science (CCTS) (funded by NIH Clinical and Translational Science Awards), the Pedigree and Population Resource, University of Utah Information Technology Services, and Biomedical Informatics Core for establishing the Master Subject Index between the Utah Population Database, the University of Utah Health Sciences Center, and Intermountain Health Care.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Electronic supplementary material
ESM 1
(DOCX 19 kb)
Rights and permissions
About this article
Cite this article
Blackburn, B.E., Ganz, P.A., Rowe, K. et al. Reproductive and gynecological complication risks among thyroid cancer survivors. J Cancer Surviv 12, 702–711 (2018). https://doi.org/10.1007/s11764-018-0707-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11764-018-0707-7