Abstract
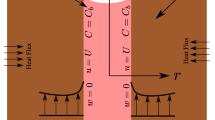
A numerical simulation of interstitial fluid flow and blood flow and diffusion of magnetic nanoparticles (MNPs) are developed, based on the governing equations for the fluid flow, i.e., the continuity and momentum and mass diffusion equations, to a tissue containing two-dimensional cylindrical tumor. The tumor is assumed to be rigid porous media with a necrotic core, interstitial fluid and two capillaries with arterial pressure input and venous pressure output. Blood flow through the capillaries and interstitial fluid flow in tumor tissues are carried by extended Poiseuille’s law and Darcy’s law, respectively. Transvascular flows are also described using Starling’s law. MNPs diffuse by interstitial fluid flow in tumor. The finite difference method has been used to simulate interstitial fluid pressure and velocity, blood pressure and velocity and diffusion of MNPs injected inside a biological tissue during magnetic fluid hyperthermia (MFH). Results show that the interstitial pressure has a maximum value at the center of the tumor and decreases toward the first capillary. The reduction continues between two capillaries, and interstitial pressure finally decreases in direction of the tumor perimeter. This study also shows that decreasing in intercapillary distance may cause a decrease in interstitial pressure. Furthermore, multi-site injection of nanoparticles has better effect on MFH.

































Similar content being viewed by others
References
Attaluri, A., Ma, R., Qiu, Y., Li, W., Zhu, L.: Nanoparticle distribution and temperature elevations in prostatic tumours in mice during magnetic nanoparticle hyperthermia. Int. J. Hyperth. 27, 491–502 (2011)
Attar, M.M., Haghpanahi, M., Amanpour, S., Mohaqeq, M.: Analysis of bioheat transfer equation for hyperthermia cancer treatment. J. Mech. Sci. Technol. 28, 763–771 (2014)
Baish, J.W., Netti, P.A., Jain, R.K.: Transmural coupling of fluid flow in microcirculatory network and interstitium in tumors. Microvasc. Res. 53, 128–141 (1997)
Baxter, L.T., Jain, R.K.: Transport of fluid and macromolecules in tumors (II): role of heterogeneous perfusion and lymphatics. Microvasc. Res. 40, 246–263 (1990)
Baxter, L.T., Jain, R.K.: Transport of fluid and macromolecules in tumors (III): role of binding and metabolism. Microvasc. Res. 4, 15–23 (1991a)
Baxter, L.T., Jain, R.K.: Transport of fluid and macromolecules in tumors IV: a microscopic model of the perivascular distribution. Microvasc. Res. 41, 252–272 (1991b)
Bear, J.: Dynamics of Fluids in Porous Media. Dover Publications, New York (1988)
Charjouei Moghadam, M., Deyranlou, A., Sharifi, A., Niazmand, H.: Numerical simulation of the tumor interstitial fluid transport: consideration of drug delivery mechanism. Microvasc. Res. 101, 62–71 (2015)
Di Michele, F., Pizzichelli, G., Mazzolai, B., Sinibaldi, E.: On the preliminary design of hyperthermia treatments based on infusion and heating of magnetic nanofluids. Math. Biosci. 262, 105–116 (2015)
Goldacre, R.J., Sylven, B.: On the access of blood-borne dyes to various tumor regions. Br. J. Cancer 16, 306–322 (1962)
Golneshan, A.A., Lahonian, M.: Diffusion of magnetic nanoparticles in a multi-site injection process within a biological tissue during magnetic fluid hyperthermia using lattice Boltzmann method. Mech. Res. Commun. 38, 425–430 (2011)
Hassanpour, S., Saboonchi, A.: Interstitial hyperthermia treatment of countercurrent vascular tissue: a comparison of Pennes, WJ and porous media bioheat models. J. Therm. Biol. 46, 47–55 (2014)
Jain, R.K.: Determinants of tumor blood flow: a review. Cancer Res. 48, 2641–2658 (1988a)
Jain, R.K., Baxter, L.T.: Mechanisms of heterogeneous distribution of monoclonal antibodies and other macromolecules in tumors: significance of elevated interstitial pressure. Cancer Res. 48, 7022–7032 (1988)
Jain, R.K., Hartley, K.W.: Tumor blood flow-characterization, modifications, and role in hyperthermia. IEEE Trans. Sonics Ultrason. 31, 504–525 (1984)
Lin, ChT, Liu, KCh.: Estimation for the heating effect of magnetic nanoparticles in perfused tissues. Int. Commun. Heat Mass Transf. 36, 241–244 (2009)
Maenosono, S., Saita, S.: Theoretical assessment of FePt nanoparticles as heating elements for magnetic hyperthermia. IEEE Trans. Magn. 42, 1638–1642 (2006)
Matsuki, H., Yanada, T.: Temperature sensitive amorphous magnetic flakes for intra-tissue hyperthermia. Mater. Sci. Eng. A 181–182, 1366–1368 (1994)
McDougall, S.R., Anderson, A.R.A., Chaplain, M.A.J., Sherratt, J.A.: Mathematical modeling of flow through vascular network: implications for tumor-induced angiogenesis and chemotherapy strategies. Bull. Math. Biol. 64, 673–702 (2002)
Nabil, M., Decuzzi, P., Zuninol, P.: Modelling mass and heat transfer in nano-based cancer hyperthermia. R. Soc. Open Sci. 2, 150447 (2015)
Netti, P.A., Baxter, L.T., Boucher, Y., Skalak, R., Jain, R.K.: Time-dependent behavior of interstitial fluid pressure in solid tumors: implication for drug delivery. Cancer Res. 55, 5451–5458 (1995)
Nicholson, C.: Diffusion and related transport mechanism in brain tissue. Rep. Prog. Phys. 64, 815–884 (2001)
Pozrikidis, C.: Numerical simulation of blood and interstitial flow through a solid tumor. J. Math. Biol. 60, 75–94 (2010)
Pozrikidis, C., Farrow, D.A.: A model of fluid flow in solid tumors. Ann. Biomed. Eng. 31, 181–194 (2003)
Robinson, J.E., Wizenberg, M.J., Mccready, W.A.: Combined hyperthermia and radiation, an alternative to heavy particle therapy for reduced oxygen enhancement ratios. Nature 251, 521–522 (1974)
Salloum, M., Ma, R.H., Weeks, D., Zhu, L.: Controlling nanoparticle delivery in magnetic nanoparticle hyperthermia for cancer treatment: experimental study in agarose gel. Int. J. Hyperth. 24, 337–345 (2008a)
Salloum, M., Ma, R.H., Zhu, L.: An in-vivo experimental study of temperature elevations in animal tissue during magnetic nanoparticle hyperthermia. Int. J. Hyperth. 24, 589–601 (2008b)
Saltzman, W.M., Radomsky, M.L.: Drugs released from polymers: diffusion and elimination in brain tissue. Chem. Eng. Sci. 46, 2429–2444 (1991)
Sefidgar, M., Soltani, M., Raahemifar, K., Bazmara, H.: Effect of fluid friction on interstitial fluid flow coupled with blood flow through solid tumor microvascular network. Comput. Math. Methods Med. (2015). doi:10.1155/2015/673426
Sefidgar, M., Soltani, M., Raahemifar, K., Sadeghi, M., Bazmara, H., Bazargan, M., Mousavi Naeenian, M.: Numerical modeling of drug delivery in a dynamic solid tumor microvasculature. Microvasc. Res. 99, 43–56 (2015b)
Sefidgar, M., Soltani, M., Raahemifar, K., Bazmara, H., Nayinian, S.M.M., Bazargan, M.: Effect of tumor shape, size, and tissue transport properties on drug delivery to solid tumors. J. Biol. Eng. 8, 1 (2014)
Soltani, M., Chen, P.: Effect of tumor shape and size on drug delivery to solid tumors. J. Biol. Eng. 6, 1 (2012)
Soltani, M., Chen, P.: Numerical modeling of fluid flow in solid tumors. PLoS One 6, e20344 (2011)
Steeves, R.A.: Hyperthermia in cancer therapy: where are we today and where are we going? Bull. N.Y. Acad. Med. 68, 342–350 (1992)
Stohrer, M., Boucher, Y., Stangassinger, M., Jain, R.K.: Oncotic pressure in solid tumors is elevated. Cancer Res. 60, 4251–4255 (2000)
Vallooran, J.J., Negrini, R., Mezzenga, R.: Controlling anisotropic drug diffusion in lipid-Fe\(_{3}\)O\(_{4}\) nanoparticle hybrid mesophases by magnetic alignment. Langmuir 29, 999–1004 (2013)
Wang, C.H., Li, J.: Three dimensional simulation of IgG delivery to tumors. Chem. Eng. Sci. 53, 3579–3600 (1998)
Wang, C.H., Li, J., Teo, C.S., Lee, T.: The delivery of BCNU to brain tumors. J. Control. Release 61, 21–41 (1999)
Welter, M., Rieger, H.: Interstitial fluid flow and drug delivery in vascularized tumors: a computational model. PLoS One 8, e70395 (2013)
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Zakariapour, M., Hamedi, M.H. & Fatouraee, N. Numerical Investigation of Magnetic Nanoparticles Distribution Inside a Cylindrical Porous Tumor Considering the Influences of Interstitial Fluid Flow. Transp Porous Med 116, 251–274 (2017). https://doi.org/10.1007/s11242-016-0772-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11242-016-0772-1