Abstract
Stages of change measure an individual’s readiness to alter a health behavior. This study examined the latent longitudinal patterns of stages of change (SoC) for regular exercise over time among individuals participating in a lifestyle intervention project. It also investigated the association between the longitudinal patterns of SoC and intervention outcomes using a new statistical method to assess the relationship between latent class membership and distal outcomes. We analyzed data from the Special Diabetes Program for Indians Diabetes Prevention Program, a lifestyle intervention program to prevent diabetes among American Indians and Alaska Natives. Latent class analysis (LCA) was conducted to identify the longitudinal patterns of SoC for regular exercise reported at three time points. LCA with distal outcomes was performed to investigate the associations between latent class membership and behavioral changes after the intervention. The parameters and standard errors of the LCA with distal outcomes models were estimated using an improved three-step approach. Three latent classes were identified: Pre-action, Transition, and Maintenance classes. The Transition class, where stage progression occurred, had the greatest improvements in physical activity and weight outcomes at both time points post-baseline among female participants. It also had the largest improvements in weight outcomes among male participants. Furthermore, the Pre-action class had more attenuation in the improvements they had achieved initially than the other two classes. These findings suggest the potential importance of motivating participants to modify their readiness for behavioral change in future lifestyle interventions.


Similar content being viewed by others
References
Absetz, P., Valve, R., Oldenburg, B., Heinonen, H., Nissinen, A., Fogelholm, M., & Uutela, A. (2007). Type 2 diabetes prevention in the “real world”: One-year results of the GOAL implementation trial. Diabetes Care, 30, 2465–2470. doi:10.2337/dc07-0171.
Adams, J., & White, M. (2003). Are activity promotion interventions based on the transtheoretical model effective? A critical review. British Journal of Sports Medicine, 37, 106–114. doi:10.1136/bjsm.37.2.106.
Adams, J., & White, M. (2005). Why don’t stage-based activity promotion interventions work? Health Education Research, 20, 237–243. doi:10.1093/her/cyg105.
Adams, S. A., Matthews, C. E., Ebbeling, C. B., Moore, C. G., Cunningham, J. E., Fulton, J., & Hebert, J. R. (2005). The effect of social desirability and social approval on self-reports of physical activity. American Journal of Epidemiology, 161, 389–398. doi:10.1093/aje/kwi054.
Ali, M. K., Echouffo-Tcheugui, J., & Williamson, D. F. (2012). How effective were lifestyle interventions in real-world settings that were modeled on the Diabetes Prevention Program? Health Affairs, 31, 67–75. doi:10.1377/hlthaff.2011.1009.
Asparouhov, T., & Muthén, B. (2014). Auxiliary variables in mixture modeling: Three-step approaches using Mplus. Structural Equation Modeling, 21, 329–341. doi:10.1080/10705511.2014.915181.
Bolck, A., Croon, M. A., & Hagenaars, J. A. (2004). Estimating latent structure models with categorical variables: One-step versus three-step estimators. Political Analysis, 12, 3–27. doi:10.1093/pan/mph001.
Casazza, K., Fontaine, K. R., Astrup, A., Birch, L. L., Brown, A. W., Bohan Brown, M. M., & Allison, D. B. (2013). Myths, presumptions, and facts about obesity. New England Journal of Medicine, 368, 446–454. doi:10.1056/NEJMsa1208051.
Collins, L. M., & Lanza, S. T. (2010). Latent class and latent transition analysis: With applications in the social, behavioral, and health sciences. Hoboken: Wiley.
Evers, K. E., Prochaska, J. O., Johnson, J. L., Mauriello, L. A., Padula, J. A., & Prochaska, J. M. (2006). A randomized clinical trial of a population- and transtheoretical model-based stress-management intervention. Health Psychology, 25, 521–529. doi:10.1037/0278-6133.25.4.521.
Feingold, A., Tiberio, S. S., & Capaldi, D. M. (2014). New approaches for examining associations with latent categorical variables: Applications to substance abuse and aggression. Psychology of Addictive Behaviors, 28, 257–267. doi:10.1037/a0031487.
Greaney, M. L., Riebe, D., Ewing Garber, C., Rossi, J. S., Lees, F. D., Burbank, P. A., & Clark, P. G. (2008). Long-term effects of a stage-based intervention for changing exercise intentions and behavior in older adults. Gerontologist, 48, 358–367.
Jiang, L., Beals, J., Zhang, L., Mitchell, C. M., Manson, S. M., Acton, K. J., & Roubideaux, Y. (2012). Latent class analysis of stages of change for multiple health behaviors: Results from the special diabetes program for Indians diabetes prevention program. Prevention Science, 13, 449–461. doi:10.1007/s11121-011-0272-z.
Jiang, L., Manson, S. M., Beals, J., Henderson, W. G., Huang, H., Acton, K. J., & Roubideaux, Y. (2013). Translating the diabetes prevention program into American Indian and Alaska native communities: results from the special diabetes program for Indians diabetes prevention demonstration project. Diabetes Care, 36, 2027–2034. doi:10.2337/dc12-1250.
Johnson, S. S., Paiva, A. L., Cummins, C. O., Johnson, J. L., Dyment, S. J., Wright, J. A., & Sherman, K. (2008). Transtheoretical model-based multiple behavior intervention for weight management: Effectiveness on a population basis. Preventive Medicine, 46, 238–246. doi:10.1016/j.ypmed.2007.09.010.
Knowler, W. C., Barrett-Connor, E., Fowler, S. E., Hamman, R. F., Lachin, J. M., Walker, E. A., & Diabetes Prevention Program Res, G. (2002). Reduction in the incidence of type 2 diabetes with lifestyle intervention or metformin. New England Journal of Medicine, 346, 393–403.
Lanza, S. T., & Collins, L. M. (2006). A mixture model of discontinuous development in heavy drinking from ages 18 to 30: The role of college enrollment. Journal of Studies on Alcohol, 67, 552–561.
Lanza, S. T., Tan, X. M., & Bray, B. C. (2013). Latent class analysis with distal outcomes: A flexible model-based approach. Structural Equation Modeling, 20, 1–26. doi:10.1080/10705511.2013.742377.
Makiko, N., Aiba, N., Suda, N., Morita, A., Miyachi, M., Sasaki, S., & Watanabe, S. (2012). Behavioral change during weight loss program and one-year follow-up: Saku Control Obesity Program (SCOP) in Japan. Asia Pacific Journal of Clinical Nutrition, 21, 22–34.
Marcus, B. H., Banspach, S. W., Lefebvre, R. C., Rossi, J. S., Carleton, R. A., & Abrams, D. B. (1992). Using the stages of change model to increase the adoption of physical activity among community participants. American Journal of Health Promotion, 6, 424–429.
Marcus, B. H., Bock, B. C., Pinto, B. M., Forsyth, L. H., Roberts, M. B., & Traficante, R. M. (1998). Efficacy of an individualized, motivationally-tailored physical activity intervention. Annals of Behavioral Medicine, 20, 174–180. doi:10.1007/bf02884958.
Muthén, L. K., & Muthén, B. O. (2012). Mplus user’s guide (7th ed.). Los Angeles: Muthén & Muthén.
Pinto, B. M., Frierson, G. M., Rabin, C., Trunzo, J. J., & Marcus, B. H. (2005). Home-based physical activity intervention for breast cancer patients. Journal of Clinical Oncology, 23, 3577–3587. doi:10.1200/JCO.2005.03.080.
Prochaska, J. O., & DiClemente, C. C. (1983). Stages and processes of self-change of smoking: Toward an integrative model of change. Journal of Consulting and Clinical Psychology, 51, 390–395.
Prochaska, J. O., DiClemente, C. C., Velicer, W. F., & Rossi, J. S. (1993). Standardized, individualized, interactive, and personalized self-help programs for smoking cessation. Health Psychology, 12, 399–405.
Riemsma, R. P., Pattenden, J., Bridle, C., Sowden, A. J., Mather, L., Watt, I. S., & Walker, A. (2003). Systematic review of the effectiveness of stage based interventions to promote smoking cessation. The British Medical Journal, 326, 1175–1177. doi:10.1136/bmj.326.7400.1175.
Salmela, S., Poskiparta, M., Kasila, K., Vahasarja, K., & Vanhala, M. (2009). Transtheoretical model-based dietary interventions in primary care: A review of the evidence in diabetes. Health Education Research, 24, 237–252. doi:10.1093/her/cyn015.
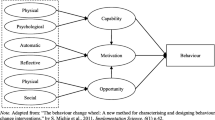
Silverwood, R. J., Nitsch, D., Pierce, M., Kuh, D., & Mishra, G. D. (2011). Characterizing longitudinal patterns of physical activity in mid-adulthood using latent class analysis: results from a prospective cohort study. American Journal of Epidemiology, 174, 1406–1415. doi:10.1093/aje/kwr266.
Sutton, S. (2001). Back to the drawing board? A review of applications of the transtheoretical model to substance use. Addiction, 96, 175–186. doi:10.1080/09652140020017049.
Telford, R. D. (2007). Low physical activity and obesity: Causes of chronic disease or simply predictors? Medicine and Science in Sports and Exercise, 39, 1233–1240. doi:10.1249/mss.0b013e31806215b7.
The Diabetes Prevention Program (DPP). (2002). Description of lifestyle intervention. Diabetes Care, 25, 2165–2171.
Topolski, T. D., LoGerfo, J., Patrick, D. L., Williams, B., Walwick, J., & Patrick, M. B. (2006). The Rapid Assessment of Physical Activity (RAPA) among older adults. Preventing Chronic Disease, 3, A118.
Vermunt, J. K. (2010). Latent class modeling with covariates: Two improved three-step approaches. Political Analysis, 18, 450–469.
Acknowledgments
The authors would like to express our gratitude to the Indian Health Service (IHS) as well as all tribal and urban Indian health programs and participants involved in the Special Diabetes Program for Indians Diabetes Prevention Program.
Compliance with Ethical Standards
ᅟ
Funding
Funding for SDPI-DP project was provided by the Indian Health Service (HHSI242200400049C, S. Manson). Manuscript preparation was supported in part by American Diabetes Association (ADA #7-12-CT-36, L. Jiang) and the National Institute of Diabetes and Digestive and Kidney Diseases (1P30DK092923, S.M. Manson).
Conflicts of Interest
The authors claim no conflict of interest.
Ethical Approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. The SDPI-DP protocol was approved by the institutional review board (IRB) of the University of Colorado Denver and the IHS IRB. When required, grantees obtained approval from other entities charged with overseeing research in their programs (e.g., tribal review boards).
Informed Consent
All participants provided written informed consent and Health Insurance Portability and Accountability Act authorization.
Author information
Authors and Affiliations
Consortia
Corresponding author
Additional information
Grant programs participating in the Special Diabetes Program for Indians Diabetes Prevention Demonstration Project: Confederated Tribes of the Chehalis Reservation, Cherokee Nation, Cheyenne River Sioux Tribe, the Chickasaw Nation, Coeur d’Alene Tribe, Colorado River Indian Tribes, Colville Confederated Tribes, Cow Creek Band of Umpqua Tribe, Fond du Lac Reservation, Gila River Health Care, Haskell Health Center, Ho-Chunk Nation, Indian Health Board of Minneapolis, Urban Native Diabetes Prevention Consortium, Kenaitze Indian Tribe IRA, Lawton IHS Service Unit, Menominee Indian Tribe of Wisconsin, Mississippi Band of Choctaw Indians, Norton Sound Health Corporation, Pine Ridge IHS Service Unit, Pueblo of San Felipe, Quinault Indian Nation, Rapid City IHS Diabetes Program, Red Lake Comprehensive Health Services, Rocky Boy Health Board, Seneca Nation of Indians, Sonoma County Indian Health Project, South East Alaska Regional Health Consortium, Southcentral Foundation, Trenton Indian Service Area, Tuba City Regional Health Care Corporation, United American Indian Involvement, Inc., United Indian Health Services, Inc., Warm Springs Health & Wellness Center, Winnebago Tribe of Nebraska, Zuni Pueblo.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Appendix 1
Baseline characteristics and SoC distributions among SDPI-DP participants (DOCX 32 kb)
Appendix 2
Baseline characteristics among SDPI-DP participants by latent class membership (DOCX 29 kb)
Appendix 3
Associations between latent class membership and changes in intervention outcomes among SDPI-DP participants (Parameters estimated using classical three-step approach) (DOCX 31 kb)
Appendix 4
Associations between latent class membership and changes in intervention outcomes among SDPI-DP participants (Parameters estimated using model-based approach) (DOCX 33 kb)
Appendix 5
The expected value of the SoC variable at each time point for each latent class with changes in aerobic RAPA (Rapid Assessment of Physical Activity) from baseline to post-curriculum assessment as a distal outcome, using model-based approach. (Expected value is calculated as the sum of the product of stage of change variable and its corresponding item-specific probability for each latent class at each time point.) (DOCX 88 kb)
Rights and permissions
About this article
Cite this article
Jiang, L., Chen, S., Zhang, B. et al. Longitudinal Patterns of Stages of Change for Exercise and Lifestyle Intervention Outcomes: An Application of Latent Class Analysis with Distal Outcomes. Prev Sci 17, 398–409 (2016). https://doi.org/10.1007/s11121-015-0599-y
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11121-015-0599-y