Abstract
Introduction
We investigated multi-domain baseline neurocognition of primary brain tumor patients prior to radiotherapy (RT), including clinical predictors of function and association between pre-RT and post-RT impairment on a prospective trial.
Methods
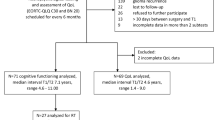
A multi-domain neuropsychological battery (memory, executive functioning, language, attention, processing) was performed on 37 patients, pre-RT and 3-(n = 21), 6-(n = 22) and 12-(n = 14) months post-RT. Impairment rate was the proportion of patients with standardized T-scores ≤ 1.5 standard deviations below normative means. Per-patient impairment across all domains was calculated using a global deficit score (GDS; higher value indicates more impairment). Associations between baseline GDS and clinical variables were tested. Global GDS impairment rate at each time point was the fraction of patients with GDS scores > 0.5.
Results
Statistically significant baseline neurocognitive impairments were identified on 4 memory (all p ≤ 0.03) and 2 out of 3 (p = 0.01, p = 0.027) executive functioning tests. Per-patient baseline GDS was significantly associated with tumor volume (p = 0.048), tumor type (p = 0.043), seizure history (p = 0.007), and use of anti-epileptics (p = 0.009). The percentage of patients with the same impairment status at 3-, 6-, and 12-months as at baseline were 88%, 85%, and 85% respectively.
Conclusions
Memory and executive functioning impairment were the most common cognitive deficits prior to RT. Patients with larger tumors, more aggressive histology, and use of anti-epileptics had higher baseline GDS values. GDS is a promising tool to encompass multi-domain neurocognitive function, and baseline GDS can identify those at risk of cognitive impairment.



Similar content being viewed by others
References
Makale MT, McDonald CR, Hattangadi-Gluth JA et al (2017) Mechanisms of radiotherapy-associated cognitive disability in patients with brain tumours. Nat Rev Neurol 13:52–64
Greene-Schloesser D, Robbins ME, Peiffer AM et al (2012) Radiation-induced brain injury: a review. Front Oncol 2:1–18
Greene-Schloesser DM, Moore E, Robbins ME (2013) Molecular pathways: radiation-induced cognitive impairment. Clin Cancer Res 19:2294–2300
Jacob J, Durand T, Feuvret L et al (2018) Cognitive impairment and morphological changes after radiation therapy in brain tumors: a review. Radiother Oncol 128:221–228
Tringale KR, Nguyen T, Bahrami N et al (2019) Identifying early diffusion imaging biomarkers of regional white matter injury as indicators of executive function decline following brain radiotherapy: a prospective clinical trial in primary brain tumor patients. Radiother Oncol 132:27–33
Gondi V, Tomé WA, Mehta MP (2010) Why avoid the hippocampus? A comprehensive review. Radiother Oncol 97:370–376
Karunamuni RA, Moore KL, Seibert TM et al (2016) Radiation sparing of cerebral cortex in brain tumor patients using quantitative neuroimaging. Radiother Oncol 118:29–34
Murzin VL, Woods K, Moiseenko V et al (2018) 4Π Plan optimization for cortical-sparing brain radiotherapy. Radiother Oncol 127:128–135
Wefel JS, Lenzi R, Theriault R et al (2004) “Chemobrain” in breast carcinoma? A prologue. Cancer 101:466–475
Wefel JS, Saleeba AK, Buzdar AU et al (2010) Acute and late onset cognitive dysfunction associated with chemotherapy in women with breast cancer. Cancer 116:3348–3356
Noll KR, Bradshaw ME, Weinberg JS et al (2018) Relationships between neurocognitive functioning, mood, and quality of life in patients with temporal lobe glioma. Psychooncology 26:617–624
Noll KR, Sullaway C, Ziu M et al (2014) Relationships between tumor grade and neurocognitive functioning in patients with glioma of the left temporal lobe prior to surgical resection. Neuro Oncol 17:580–587
Blackstone K, Moore DJ, Franklin DR et al (2012) Defining neurocognitive impairment in HIV: deficit scores versus clinical ratings. Clin Neuropsychol. https://doi.org/10.1038/jid.2014.371
Reichenberg A, Harvey PD, Bowie CR et al (2009) Neuropsychological function and dysfunction in schizophrenia and psychotic affective disorders. Schizophr Bull 35:1022–1029
Society RS (2018) Controlling the false discovery rate: a practical and powerful approach to multiple testing author (s): Yoav Benjamini and Yosef Hochberg Source. J Royal Stat Soc B 57(1):289–300
Makale MT, McDonald CR, Hattangadi-Gluth JA et al (2016) Mechanisms of radiotherapy-associated cognitive disability in patients with brain tumours. Nat Rev Neurol 13:52
Gondi V, Pugh SL, Tome WA et al (2014) Preservation of memory with conformal avoidance of the hippocampal neural stem-cell compartment during whole-brain radiotherapy for brain metastases (RTOG 0933): a Phase II Multi-Institutional Trial. J Clin Oncol 32:3810–3819
Meador KJ. Cognitive outcomes and predictive factors in epilepsy. Neurology 2002;58:S21 LP-S26
Butler JM, Rapp SR, Shaw EG (2006) Managing the cognitive effects of brain tumor radiation therapy. Curr Treat Options Oncol 7:517–523
Brown PD, Asher AL, Ballman K V, et al. NCCTG N0574 (Alliance): A phase III randomized trial of whole brain radiation therapy (WBRT) in addition to radiosurgery (SRS) in patients with 1 to 3 brain metastases. J Clin Oncol 2015;33:LBA4–LBA4
Proton Beam or Intensity-Modulated Radiation Therapy in Preserving Brain Function in Patients With IDH Mutant Grade II or III Glioma—Full Text View—ClinicalTrials.gov. CinicalTrials.gov. Accessed June 27 2018
Chapman CH, Zhu T, Nazem-zadeh M et al (2016) Diffusion tensor imaging predicts cognitive function change following partial brain radiotherapy for low-grade and benign tumors. Radiother Oncol 120:234–240
Ma TM, Grimm J, McIntyre R et al (2017) A prospective evaluation of hippocampal radiation dose volume effects and memory deficits following cranial irradiation. Radiother Oncol 125:234–240
Goldberg TE, Harvey PD, Wesnes KA et al (2015) Practice effects due to serial cognitive assessment: implications for preclinical Alzheimer’s disease randomized controlled trials. Alzheimer’s Dement Diagn Assess Dis Monit 1:103–111
Funding
This work was funded, in part, by: National Institute of Health (NIH) grants #1KL2TR001444 (JAH-G), #UL1TR000100 (JAH-G), R01CA238783-01 (JAH-G), TL1TR001443 (KRT, DM), R01NS065838 (C.R.M.); American Cancer Society Pilot Award ACS-IRG 70-002 (JAH-G); American Cancer Society Research Scholar Grant RSG-15-229-01-CCE (C.R.M.).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Drs. Seibert, Dr. Hattangadi-Gluth, and Dr. Karunamuni report grant funding from Varian Medical Systems, unrelated to the present study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Karunamuni, R., Tringale, K.R., Burkeen, J. et al. Multi-domain neurocognitive classification of primary brain tumor patients prior to radiotherapy on a prospective clinical trial. J Neurooncol 146, 131–138 (2020). https://doi.org/10.1007/s11060-019-03353-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11060-019-03353-2