Abstract
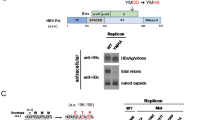
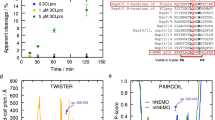
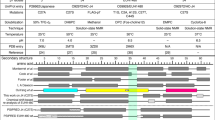
The HIV-1 accessory protein Nef plays an active role in the pathogenesis of AIDS by its numerous cellular interactions that facilitate the release of virus particles. This 27 kDa protein is required for maintenance of the viral replication in HIV, and is also known to contribute to immune evasion, blocking of apoptosis in virus-infected cells and enhancement of virus infectivity. Nef has been shown to be secreted and is present on the surface of virus-infected cells. Recent studies from our laboratory have shown that the Nef protein is secreted from nef-transfected and HIV-1-infected cells in small exosome-like vesicles (40–100 nm diam.) that do not contain virions. We have identified three amino-terminal domains of Nef as necessary for secretion: (i) the four arginine residues (17,19,21, 22) comprising the basic region; (ii) the phosphofurin acidic cluster sequence (PACS) composed of four glutamic acid residues (61–64); (iii) a previously unknown motif spanning amino acid residues 65–69 (VGFPV) which we named the secretion modification region (SMR). In this study, we have used population-based phylogeny data and sequence analysis to characterize the conservation of the Nef SMR domain that regulates vesicle secretion. We have performed in silico computational chemistry analysis involving molecular dynamic structure modeling of mutations in the SMR motif. Sequence analysis of Nef from HIV-1-infected patients, including slow progressors (SP), long term progressors (LTP) and long term non-progressors (LTNP) demonstrated 99 % conservation of the Nef SMR motif. Computational analysis including modeling of wild-type HIV-1 Nef and V66A Nef SMR mutant using structural homology and molecular dynamics of ligand-associated interactions indicated significant structural changes in the Nef mutant, thus supporting the importance of the SMR domain for mediating Nef vesicle secretion.

Novel secretion modification region (SMR) of HIV-1 Nef







Similar content being viewed by others
References
Smith SM (2006) The pathogenesis of HIV infection: stupid may not be so dumb after all. Retrovirol 3:60–65
McIntyre LB, Geczy AF, Dyer WB, Learmont JC, Sullivan JS (1999) The Sydney Blood Bank Cohort: a case–control study using a transfused HIV-1 seronegative group. Ann Epidemiol 9:436–440
Hanna Z, Priceputu E, Hu C, Vincent P, Jolicoeur P (2006) HIV-1 Nef mutations abrogating downregulation of CD4 affect other Nef functions and show reduced pathogenicity in transgenic mice. Virol 346:40–52. doi:10.1016/j.virol.2005.10.010
Priceputu E, Rodrigue I, Chrobak P, Poudrier J, Mak TW, Hanna Z, Hu C, Kay DG, Jolicoeur P (2005) The Nef-mediated AIDS-like disease of CD4C/human immunodeficiency virus transgenic mice is associated with increased Fas/FasL expression on T cells and T-cell death but is not prevented in Fas-, FasL-, tumor necrosis factor receptor 1-, or interleukin-1beta-converting enzyme-deficient or Bcl2-expressing transgenic mice. J Virol 79:6377–6391
Simard MC, Chrobak P, Kay DG, Hanna Z, Jothy S, Jolicoeur P (2002) Expression of simian immunodeficiency virus nef in immune cells of transgenic mice leads to a severe AIDS-like disease. J Virol 76:3981–3995
Hanna Z, Kay DG, Rebai N, Guimond A, Jothy S, Jolicoeur P (1998) Nef harbors a major determinant of pathogenicity for an AIDS-like disease induced by HIV-1 in transgenic mice. Cell 95:163–175
Klotman PE, Notkins AL (1996) Transgenic models of human immunodeficiency virus type-1. Curr Top Microbiol Immunol 206:197–222
Fujii Y, Otake K, Tashiro M, Adachi A (1996) Human immunodeficiency virus type 1 Nef protein on the cell surface is cytocidal for human CD4+ T cells. FEBS Lett 393:105–108
Fujii Y, Otake K, Tashiro M, Adachi A (1996) Soluble Nef antigen of HIV-1 is cytotoxic for human CD4+ T cells. FEBS Lett 393:93–96
Okada H, Takei R, Tashiro M (1997) Nef protein of HIV-1 induces apoptotic cytolysis of murine lymphoid cells independently of CD95 (Fas) and its suppression by serine/threonine protein kinase inhibitors. FEBS Lett 417:61–64
Okada H, Takei R, Tashiro M (1997) HIV-1 Nef protein-induced apoptotic cytolysis of a broad spectrum of uninfected human blood cells independently of CD95(Fas). FEBS Lett 414:603–606
Roeth JF, Collins KL (2006) Human immunodeficiency virus type 1 Nef: adapting to intracellular trafficking pathways. Microbiol Mol Biol Rev 70:548–563
Fujii Y, Otake K, Fujita Y, Yamamoto N, Nagai Y, Tashiro M, Adachi A (1996) Clustered localization of oligomeric Nef protein of human immunodeficiency virus type 1 on the cell surface. FEBS Lett 395:257–261
Zeigler ZR, Rosenfeld CS, Andrews DF III, Nemunaitis J, Raymond JM, Shadduck RK, Kramer RE, Gryn JF, Rintels PB, Besa EC, George JN (1996) Plasma von Willebrand Factor Antigen (vWF:AG) and thrombomodulin (TM) levels in Adult Thrombotic Thrombocytopenic Purpura/Hemolytic Uremic Syndromes (TTP/HUS) and bone marrow transplant-associated thrombotic microangiopathy (BMT-TM). Am J Hematol 53:213–220
Varin A, Manna SK, Quivy V, Decrion AZ, Van Lint C, Herbein G, Aggarwal BB (2003) Exogenous Nef protein activates NF-kappa B, AP-1, and c-Jun N-terminal kinase and stimulates HIV transcription in promonocytic cells. Role in AIDS pathogenesis. J Biol Chem 278:2219–2227
Huang MB, Jin LL, James CO, Khan M, Powell MD, Bond VC (2004) Characterization of Nef-CXCR4 interactions important for apoptosis induction. J Virol 78:11084–11096
James CO, Huang M-B, Khan M, Garcia-Barrio M, Powell MD, Bond VC (2004) Extracellular Nef protein targets CD4+ T cells for apoptosis by interacting with CXCR4 surface receptors. J Virol 78:3099–3109
Calenda V, Graber P, Delamarter JF, Chermann JC (1994) Involvement of HIV nef protein in abnormal hematopoiesis in AIDS: in vitro study on bone marrow progenitor cells. Eur J Haematol 52:103–107
Federico M, Percario Z, Olivetta E, Fiorucci G, Muratori C, Micheli A, Romeo G, Affabris E (2001) HIV-1 Nef activates STAT1 in human monocytes/macrophages through the release of soluble factors. Blood 98:2752–2761
Percario Z, Olivetta E, Fiorucci G, Mangino G, Peretti S, Romeo G, Affabris E, Federico M (2003) Human immunodeficiency virus type 1 (HIV-1) Nef activates STAT3 in primary human monocyte/macrophages through the release of soluble factors: involvement of Nef domains interacting with the cell endocytotic machinery. J Leukocyte Biol 74:821–832
Campbell TD, Khan M, Huang M-B, Bond VC, Powell MD (2008) HIV-1 Nef protein is secreted into vesicles that can fuse with target cells and virions. Ethn Dis 18:S2–S9
Ali SA, Huang M-B, Campbell PE, Roth WW, Campbell T, Khan M, Newman G, Villinger F, Powell MD, Bond VC (2010) Genetic characterization of HIV type 1 Nef-induced vesicle secretion. AIDS Res Hum Retroviruses 26:173–192
Leitner T, Foley B, Hahn B, Marx P, McCutchan F, Mellors J, Wolinsky S, Korber B, (2007) HIV Sequence Compendium 2006/2007. Los Alamos National Laboratory, NM 07–
van Marle G, Henry S, Todoruk T, Sullivan A, Silva C, Rourke SB, Holden J, McArthur JC, Gill MJ, Power C (2004) Human immunodeficiency virus type 1 Nef protein mediates neural cell death: a neurotoxic role for IP-10. Virol 329:302–318
Rhodes DI, Ashton L, Solomon A, Carr A, Cooper D, Kaldor J, Deacon N (2000) Characterization of three nef-defective human immunodeficiency virus type 1 strains associated with long-term nonprogression. Australian Long-Term Nonprogressor Study Group. J Virol 74:10581–10588
Catucci M, Venturi G, Romano L, Valensin PE, Zazzi M (2000) Analysis of the HIV-1 nef gene in five intravenous drug users with long-term nonprogressive HIV-1 infection in Italy. J Med Virol 60:294–299
Yamada T, Iwamoto A (2000) Comparison of proviral accessory genes between long-term nonprogressors and progressors of human immunodeficiency virus type 1 infection. Arch Virol 145:1021–1027
Combet C, Jambon M, Deleage G, Geourjon C (2002) Geno3D: automatic comparative molecular modelling of protein. Bioinforma 18:213–214
Case DA, Cheatham TE III, Darden T, Gohlke H, Luo R, Merz KM Jr, Onufriev A, Simmerling C, Wang B, Woods RJ (2005) The Amber biomolecular simulation programs. J Comput Chem 26:1668–1688
Hornak V, Abel R, Okur A, Strockbine B, Roitberg A, Simmerling C (2006) Comparison of multiple Amber force fields and development of improved protein backbone parameters. Proteins 65:712–725
Price DJ, Brooks CL III (2004) A modified TIP3P water potential for simulation with Ewald summation. J Chem Phys 121:10096–10103
Jorgensen WL, Tirado-Rives J (2005) Potential energy functions for atomic-level simulations of water and organic and biomolecular systems. Proc Natl Acad Sci USA 102:6665–6670
Pettersen EF, Goddard TD, Huang CC, Couch GS, Greenblatt DM, Meng EC, Ferrin TE (2004) UCSF Chimera–a visualization system for exploratory research and analysis. J Comput Chem 25:1605–1612
Petsko GA, Dagmar R (2003) Protein structure and function. Wiley-Blackwell, London
Lovell SC, Davis IW, Arendall WB III, de Bakker PI, Word JM, Prisant MG, Richardson JS, Richardson DC (2003) Structure validation by Calpha geometry: phi, psi and Cbeta deviation. Proteins 50:437–450
Raymond AD, Campbell-Sims TC, Khan M, Lang M, Huang MB, Bond VC, Powell MD (2011) HIV type 1 Nef is released from infected cells in CD45+ microvesicles and is present in the plasma of HIV-infected individuals. AIDS Res Hum Retroviruses 27:167–178. doi:10.1089/aid.2009.0170
Acknowledgments
This work and the researchers at Morehouse were supported by NIH/NIGMS/MBRS grant S06 GM08248, NIH/NCRR/RCMI grant G12-RR03034, Georgia Research Alliance funding grant GRA.VAC08.W. This investigation was conducted in a facility constructed with support from Research Facilities Improvement Grant #C06 RR18386 from NIH/NCRR. The work, researchers, and facilities at Jackson State University NSF CREST Interdisciplinary Nanotoxicity Center were supported by grant NSF-CREST - # HRD-0833178. No competing financial interests exist.
Author information
Authors and Affiliations
Corresponding author
Additional information
Patrick E. Campbell and Olexandr Isayev contributed equally to this work
Rights and permissions
About this article
Cite this article
Campbell, P.E., Isayev, O., Ali, S.A. et al. Validation of a novel secretion modification region (SMR) of HIV-1 Nef using cohort sequence analysis and molecular modeling. J Mol Model 18, 4603–4613 (2012). https://doi.org/10.1007/s00894-012-1452-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00894-012-1452-x