Abstract
Purpose
To assess the impact of obesity on cancer-related fatigue (CRF) in patients with breast cancer, through a secondary analysis of a large, longitudinal, nationwide study of breast cancer patients beginning chemotherapy.
Methods
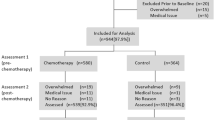
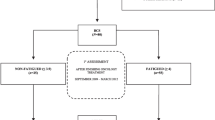
All patients (N = 565; aged 53 ± 10.6) with breast cancer completed the multidimensional fatigue symptom inventory and the symptom inventory to measure CRF symptoms at baseline, post-chemotherapy, and 6 months post-chemotherapy. Height and weight at baseline were used to categorize subjects based on body mass index (BMI): obese (≥ 30.0 kg/m2; n = 294), overweight (25.0–29.9 kg/m2; n = 146), and normal weight (18.5–24.9 kg/m2; n = 125). Multivariate regression models evaluated the relationship of obesity level to CRF over time, controlling for age, menopausal status, race, Karnofsky Performance Status, cancer stage, radiation, and exercise status.
Results
At baseline, the obese had significantly higher CRF symptoms than the normal weight subjects for both the Multidimensional fatigue symptom inventory (MFSI) total (obese = 11.2 vs normal weight = 6.3; p = 0.03) and Symptom Inventory (SI) (obese = 3.5 vs normal weight = 2.9; p = 0.03). Significantly higher SI fatigue scores persisted at post-chemotherapy for the obese (obese = 5.0 vs normal weight = 4.4; p = 0.02). At 6 months post-chemotherapy, the obese patients still had significantly higher SI fatigue scores (obese = 3.5 vs normal weight = 3.0; p = 0.05).
Conclusion
Obese patients suffered greater CRF from pre-chemotherapy through 6 months post-chemotherapy. Recommendations for weight loss or weight maintenance may impact CRF levels in obese breast cancer patients before and after chemotherapy.


Similar content being viewed by others
Abbreviations
- CRF:
-
Cancer-related fatigue
- BMI:
-
Body mass index
- QOL:
-
Quality of life
- SI:
-
Symptom inventory
- MFSI-SF:
-
Multidimensional fatigue symptom inventory-short form
- KPS:
-
Karnofsky Performance Status
References
Goodwin PJ, Ennis M, Pritchard KI, McCready D, Koo J, Sidlofsky S, Trudeau M, Hood N, Redwood S (1999) Adjuvant treatment and onset of menopause predict weight gain after breast cancer diagnosis. J Clin Oncol Off J Am Soc Clin Oncol 17(1):120–129. https://doi.org/10.1200/jco.1999.17.1.120
Cantarero-Villanueva I, Galiano-Castillo N, Fernandez-Lao C, Diaz-Rodriguez L, Fernandez-Perez AM, Sanchez MJ, Arroyo-Morales M (2015) The influence of body mass index on survival in breast cancer patients. Clin Breast Cancer 15(2):e117–e123. https://doi.org/10.1016/j.clbc.2014.11.006
Neuhouser ML, Aragaki AK, Prentice RL, Manson JE, Chlebowski R, Carty CL, Ochs-Balcom HM, Thomson CA, Caan BJ, Tinker LF, Urrutia RP, Knudtson J, Anderson GL (2015) Overweight, obesity, and postmenopausal invasive breast cancer risk: a secondary analysis of the women’s health initiative randomized clinical trials. JAMA Oncol 1(5):611–621. https://doi.org/10.1001/jamaoncol.2015.1546
Yerushalmi R, Dong B, Chapman JW, Goss PE, Pollak MN, Burnell MJ, Levine MN, Bramwell VHC, Pritchard KI, Whelan TJ, Ingle JN, Shepherd LE, Parulekar WR, Han L, Ding K, Gelmon KA (2017) Impact of baseline BMI and weight change in CCTG adjuvant breast cancer trials. Ann Oncol 28(7):1560–1568. https://doi.org/10.1093/annonc/mdx152
Ford ME, Magwood G, Brown ET, Cannady K, Gregoski M, Knight KD, Peterson LL, Kramer R, Evans-Knowell A, Turner DP (2017) Disparities in obesity, physical activity rates, and breast cancer survival. Adv Cancer Res 133:23–50. https://doi.org/10.1016/bs.acr.2016.08.002
Picon-Ruiz M, Morata-Tarifa C, Valle-Goffin JJ, Friedman ER, Slingerland JM (2017) Obesity and adverse breast cancer risk and outcome: mechanistic insights and strategies for intervention. CA Cancer J Clin 67(5):378–397. https://doi.org/10.3322/caac.21405
Hall DL, Mishel MH, Germino BB (2014) Living with cancer-related uncertainty: associations with fatigue, insomnia, and affect in younger breast cancer survivors. Support Care Cancer 22(9):2489–2495. https://doi.org/10.1007/s00520-014-2243-y
Peoples AR, Roscoe JA, Block RC, Heckler CE, Ryan JL, Mustian KM, Janelsins MC, Peppone LJ, Moore DF Jr, Coles C, Hoelzer KL, Morrow GR, Dozier AM (2017) Nausea and disturbed sleep as predictors of cancer-related fatigue in breast cancer patients: a multicenter NCORP study. Support Care Cancer 25(4):1271–1278. https://doi.org/10.1007/s00520-016-3520-8
Bower JE (2014) Cancer-related fatigue--mechanisms, risk factors, and treatments. Nat Rev Clin Oncol 11(10):597–609. https://doi.org/10.1038/nrclinonc.2014.127
Crosswell AD, Lockwood KG, Ganz PA, Bower JE (2014) Low heart rate variability and cancer-related fatigue in breast cancer survivors. Psychoneuroendocrinology 45:58–66. https://doi.org/10.1016/j.psyneuen.2014.03.011
Barsevick AM, Irwin MR, Hinds P, Miller A, Berger A, Jacobsen P, Ancoli-Israel S, Reeve BB, Mustian K, O'Mara A, Lai JS, Fisch M, Cella D (2013) Recommendations for high-priority research on cancer-related fatigue in children and adults. J Natl Cancer Inst 105(19):1432–1440. https://doi.org/10.1093/jnci/djt242
Bower JE, Lamkin DM (2013) Inflammation and cancer-related fatigue: mechanisms, contributing factors, and treatment implications. Brain Behav Immun 30(Suppl):S48–S57. https://doi.org/10.1016/j.bbi.2012.06.011
Kuhl T, Behrens S, Jung AY, Obi N, Thone K, Schmidt ME, Becher H, Chang-Claude J (2018) Validation of inflammatory genetic variants associated with long-term cancer related fatigue in a large breast cancer cohort. Brain Behav Immun. https://doi.org/10.1016/j.bbi.2018.05.009
Izaola O, de Luis D, Sajoux I, Domingo JC, Vidal M (2015) [Inflammation and obesity (lipoinflammation)]. Nutr Hosp 31(6):2352–2358. https://doi.org/10.3305/nh.2015.31.6.8829
Chadt A, Scherneck S, Joost HG, Al-Hasani H (2000) Molecular links between obesity and diabetes: “diabesity”. In: De Groot LJ, Chrousos G, Dungan K et al (eds) . Endotext. MDText.com, Inc., South Dartmouth (MA)
Schmitz KH, Neuhouser ML, Agurs-Collins T, Zanetti KA, Cadmus-Bertram L, Dean LT, Drake BF (2013) Impact of obesity on cancer survivorship and the potential relevance of race and ethnicity. J Natl Cancer Inst 105(18):1344–1354. https://doi.org/10.1093/jnci/djt223
Meeske K, Smith AW, Alfano CM, McGregor BA, McTiernan A, Baumgartner KB, Malone KE, Reeve BB, Ballard-Barbash R, Bernstein L (2007) Fatigue in breast cancer survivors two to five years post diagnosis: a HEAL study report. Qual Life Res Int J Qual Life Asp Treat Care Rehab 16(6):947–960. https://doi.org/10.1007/s11136-007-9215-3
Demark-Wahnefried W, Kenyon AJ, Eberle P, Skye A, Kraus WE (2002) Preventing sarcopenic obesity among breast cancer patients who receive adjuvant chemotherapy: results of a feasibility study. Clin Exerc Physiol 4(1):44–49
Deluche E, Leobon S, Desport JC, Venat-Bouvet L, Usseglio J, Tubiana-Mathieu N (2018) Impact of body composition on outcome in patients with early breast cancer. Support Care Cancer 26(3):861–868. https://doi.org/10.1007/s00520-017-3902-6
Martin L, Birdsell L, Macdonald N, Reiman T, Clandinin MT, McCargar LJ, Murphy R, Ghosh S, Sawyer MB, Baracos VE (2013) Cancer cachexia in the age of obesity: skeletal muscle depletion is a powerful prognostic factor, independent of body mass index. J Clin Oncol Off J Am Soc Clin Oncol 31(12):1539–1547. https://doi.org/10.1200/jco.2012.45.2722
Kilgour RD, Vigano A, Trutschnigg B, Hornby L, Lucar E, Bacon SL, Morais JA (2010) Cancer-related fatigue: the impact of skeletal muscle mass and strength in patients with advanced cancer. J Cachexia Sarcopenia Muscle 1(2):177–185. https://doi.org/10.1007/s13539-010-0016-0
Platt A, Gross J, Davis MP (2015) Force perception, effort, strength, and dynamic muscle function in cancer-related fatigue: a pilot study. Am J Hosp Palliat Care 32(6):577–580. https://doi.org/10.1177/1049909114528746
Jeronimo AF, Freitas AG, Weller M (2017) Risk factors of breast cancer and knowledge about the disease: an integrative revision of Latin American studies. Cienc Saude Colet 22(1):135–149. https://doi.org/10.1590/1413-81232017221.09272015
Nagrani R, Mhatre S, Rajaraman P, Soerjomataram I, Boffetta P, Gupta S, Parmar V, Badwe R, Dikshit R (2016) Central obesity increases risk of breast cancer irrespective of menopausal and hormonal receptor status in women of South Asian ethnicity. Eur J Cancer 66:153–161. https://doi.org/10.1016/j.ejca.2016.07.022
Janelsins MC, Heckler CE, Peppone LJ, Kamen C, Mustian KM, Mohile SG, Magnuson A, Kleckner IR, Guido JJ, Young KL, Conlin AK, Weiselberg LR, Mitchell JW, Ambrosone CA, Ahles TA, Morrow GR (2017) Cognitive complaints in survivors of breast cancer after chemotherapy compared with age-matched controls: an analysis from a nationwide, multicenter, prospective longitudinal study. J Clin Oncol Off J Am Soc Clin Oncol 35(5):506–514. https://doi.org/10.1200/jco.2016.68.5826
Aldebeyan S, Nooh A, Aoude A, Weber MH, Harvey EJ (2017) Hypoalbuminaemia-a marker of malnutrition and predictor of postoperative complications and mortality after hip fractures. Injury 48(2):436–440. https://doi.org/10.1016/j.injury.2016.12.016
Lim WS, Roh JL, Kim SB, Choi SH, Nam SY, Kim SY (2017) Pretreatment albumin level predicts survival in head and neck squamous cell carcinoma. Laryngoscope 127(12):E437–e442. https://doi.org/10.1002/lary.26691
Tada T, Kumada T, Toyoda H, Yasuda S, Koyabu T, Nakashima M (2019) Impact of branched-chain amino acid granule therapy in patients with hepatocellular carcinoma who have normal albumin levels and low branched-chain amino acid to tyrosine ratios. Nutr Cancer:1–10. https://doi.org/10.1080/01635581.2019.1597905
Stein KD, Jacobsen PB, Blanchard CM, Thors C (2004) Further validation of the multidimensional fatigue symptom inventory-short form. J Pain Symptom Manag 27(1):14–23
Jones D, Zhao F, Fisch MJ, Wagner LI, Patrick-Miller LJ, Cleeland CS, Mendoza TR (2014) The validity and utility of the MD Anderson symptom inventory in patients with prostate cancer: evidence from the Symptom Outcomes and Practice Patterns (SOAPP) data from the Eastern Cooperative Oncology Group. Clin Genitourin Cancer 12(1):41–49. https://doi.org/10.1016/j.clgc.2013.07.003
Donovan KA, Stein KD, Lee M, Leach CR, Ilozumba O, Jacobsen PB (2015) Systematic review of the multidimensional fatigue symptom inventory-short form. Support Care Cancer 23(1):191–212. https://doi.org/10.1007/s00520-014-2389-7
Can B, Kara O, Kizilarslanoglu MC, Arik G, Aycicek GS, Sumer F, Civelek R, Demirtas C, Ulger Z (2017) Serum markers of inflammation and oxidative stress in sarcopenia. Aging Clin Exp Res 29(4):745–752. https://doi.org/10.1007/s40520-016-0626-2
Karam BS, Chavez-Moreno A, Koh W, Akar JG, Akar FG (2017) Oxidative stress and inflammation as central mediators of atrial fibrillation in obesity and diabetes. Cardiovasc Diabetol 16(1):120. https://doi.org/10.1186/s12933-017-0604-9
Saad MJ, Santos A, Prada PO (2016) Linking gut microbiota and inflammation to obesity and insulin resistance. Physiology (Bethesda, Md) 31(4):283–293. https://doi.org/10.1152/physiol.00041.2015
Weber D, O'Brien K (2017) Cancer and cancer-related fatigue and the interrelationships with depression, stress, and inflammation. J Evid Based Complementary Altern Med 22(3):502–512. https://doi.org/10.1177/2156587216676122
Andrykowski MA, Donovan KA, Laronga C, Jacobsen PB (2010) Prevalence, predictors, and characteristics of off-treatment fatigue in breast cancer survivors. Cancer 116(24):5740–5748. https://doi.org/10.1002/cncr.25294
Gerber LH, Stout N, McGarvey C, Soballe P, Shieh CY, Diao G, Springer BA, Pfalzer LA (2011) Factors predicting clinically significant fatigue in women following treatment for primary breast cancer. Support Care Cancer 19(10):1581–1591. https://doi.org/10.1007/s00520-010-0986-7
Reinertsen KV, Cvancarova M, Loge JH, Edvardsen H, Wist E, Fossa SD (2010) Predictors and course of chronic fatigue in long-term breast cancer survivors. J Cancer Surviv 4(4):405–414. https://doi.org/10.1007/s11764-010-0145-7
Taylor DL, Nichols JF, Pakiz B, Bardwell WA, Flatt SW, Rock CL (2010) Relationships between cardiorespiratory fitness, physical activity, and psychosocial variables in overweight and obese breast cancer survivors. Int J Behav Med 17(4):264–270. https://doi.org/10.1007/s12529-010-9076-y
Ancoli-Israel S, Liu L, Rissling M, Natarajan L, Neikrug AB, Palmer BW, Mills PJ, Parker BA, Sadler GR, Maglione J (2014) Sleep, fatigue, depression, and circadian activity rhythms in women with breast cancer before and after treatment: a 1-year longitudinal study. Support Care Cancer 22(9):2535–2545. https://doi.org/10.1007/s00520-014-2204-5
Reeves MM, Terranova CO, Eakin EG, Demark-Wahnefried W (2014) Weight loss intervention trials in women with breast cancer: a systematic review. Obes Rev 15(9):749–768. https://doi.org/10.1111/obr.12190
Demark-Wahnefried W, Campbell KL, Hayes SC (2012) Weight management and its role in breast cancer rehabilitation. Cancer 118(8 Suppl):2277–2287. https://doi.org/10.1002/cncr.27466
Gravena AA, Brischiliari SC, Lopes TC, Agnolo CM, Carvalho MD, Pelloso SM (2013) Excess weight and abdominal obesity in postmenopausal Brazilian women: a population-based study. BMC Womens Health 13:46. https://doi.org/10.1186/1472-6874-13-46
Mefferd K, Nichols JF, Pakiz B, Rock CL (2007) A cognitive behavioral therapy intervention to promote weight loss improves body composition and blood lipid profiles among overweight breast cancer survivors. Breast Cancer Res Treat 104(2):145–152. https://doi.org/10.1007/s10549-006-9410-x
Campbell KL, Van Patten CL, Neil SE, Kirkham AA, Gotay CC, Gelmon KA, McKenzie DC (2012) Feasibility of a lifestyle intervention on body weight and serum biomarkers in breast cancer survivors with overweight and obesity. J Acad Nutr Diet 112(4):559–567. https://doi.org/10.1016/j.jada.2011.10.022
Meneses-Echavez JF, Gonzalez-Jimenez E, Ramirez-Velez R (2015) Effects of supervised exercise on cancer-related fatigue in breast cancer survivors: a systematic review and meta-analysis. BMC Cancer 15:77. https://doi.org/10.1186/s12885-015-1069-4
Lipsett A, Barrett S, Haruna F, Mustian K, O'Donovan A (2017) The impact of exercise during adjuvant radiotherapy for breast cancer on fatigue and quality of life: a systematic review and meta-analysis. Breast 32:144–155. https://doi.org/10.1016/j.breast.2017.02.002
Lin PJ, Peppone LJ, Janelsins MC, Mohile SG, Kamen CS, Kleckner IR, Fung C, Asare M, Cole CL, Culakova E, Mustian KM (2018) Yoga for the management of cancer treatment-related toxicities. Curr Oncol Rep 20(1):5. https://doi.org/10.1007/s11912-018-0657-2
Acknowledgments
The authors would like to thank all study participants from NCORP sites involved in this research.
Funding
This study was funded by grants U10CA037420, UG1 CA189961, DP2 CA195765, R25 CA1026185, and K07CA221931 through the National Cancer Institute in the National Institute of Health.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Ethical approval
Furthermore, the authors declare that the protocol herein described complies with the University of Rochester Medical Center and that they obtained institutional review board approval and have been performed in accordance with the ethical standards as laid down in the 1964 Declaration of Helsinki and its later amendments or comparable ethical standards.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Inglis, J.E., Janelsins, M.C., Culakova, E. et al. Longitudinal assessment of the impact of higher body mass index on cancer-related fatigue in patients with breast cancer receiving chemotherapy. Support Care Cancer 28, 1411–1418 (2020). https://doi.org/10.1007/s00520-019-04953-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00520-019-04953-4