Abstract
Purpose
The present study was designed to evaluate the 16 weeks diabetes prevention program (DPP) combined with instructed run sprint interval training (INT) or moderate-intensity continuous training (MICT) on glycemic control, body composition, fitness, exercise adherence, and perceived exercise enjoyment in sedentary, adults with prediabetes.
Methods
Participants completed three weekly supervised sessions of INT (4–10 bouts of 30 s maximal sprints followed by a 4 min active recovery) or MICT (30–60 min at 45–55% HRR) exercise coupled with the DPP for 16 weeks. At baseline, 8 and 16 weeks, participants completed fitness and clinical assessments as well as questionnaires to assess group and time differences.
Results
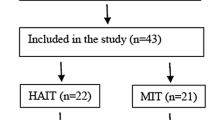
Twenty-nine study participants (INT n = 17, MICT n = 12) were randomized, however, significantly (p = 0.024) more participants withdrew from the INT (n = 11) than MICT (n = 4) treatment. There was no significant difference between groups in perceived exercise enjoyment, but, the MICT group significantly improved their perceived exercise enjoyment (10.8 ± 14.2; p = 0.021) from baseline to 16 weeks. Both INT and MICT groups decreased their body weight (2.0 ± 0.8 vs. − 5.5 ± 1.4 kg; p < 0.001), BMI (− 0.6 ± 0.3 vs. − 2.1 ± 0.5 kg/m2; p < 0.001), body fat mass (1.4 ± 0.6 vs. − 4.2 ± 1.0 kg; p < 0.001), fasting glucose (− 0.09 ± 0.01 vs. − 0.18 ± 0.02 mmol/L; p = 0.020), and HbA1c (− 0.21 ± 0.09 vs. − 0.12 ± 0.12%; p = 0.001), respectively, however, the MICT had greater reductions (GxT: p ≤ 0.05) in body weight, BMI, and body fat than the INT group.
Conclusion
Sixteen weeks of MICT is adhered to better and elicits greater improvements in body composition than INT. Nevertheless, both interventions similarly reduced fasting glucose and HbA1c in adults with prediabetes, suggesting either treatment could be effective for T2D prevention.




Similar content being viewed by others
Abbreviations
- ACSM:
-
American College of Sports Medicine
- ANOVA:
-
Analysis of variance
- BMI:
-
Body mass index
- BP:
-
Blood pressure
- DPP:
-
Diabetes prevention program
- GxT:
-
Group by time interaction
- HbA1c:
-
Hemoglobin A1c
- HR:
-
Heart rate
- INT:
-
Interval training
- ITT:
-
Intention to treat
- MICT:
-
Moderate-intensity continuous exercise
- OGTT:
-
Oral glucose tolerance test
- PACES:
-
Physical activity enjoyment scale
- RPE:
-
Rate of perceived exertion
- SE:
-
Standard error
- T2D:
-
Type 2 diabetes
- WHR:
-
Waist-to-hip ratio
References
American Diabetes Association (2016) Diagnosing diabetes and learning about prediabetes. http://www.diabetes.org/diabetes-basics/statistics/. Accessed 23 Oct 2017
Bouaziz W, Schmitt E, Kaltenback G, Geny B, Vogel T (2015) Health benefits of cycle ergometer training for older adults over 70: a review. Eur Rev Aging Phys Act 12:8
Boyd JC, Simpson CA, Jung ME, Gurd BJ (2013) Reducing the intensity and volume of interval training diminishes cardiovascular adaptation but not mitochondrial biogenesis in overweight/obese men. PLoS ONE 8(7):e68091
Burgomaster K, Cermak N, Phillips S, Benton C, Bonen A, Gibala M (2007) Divergent response of metabolite transport proteins in human skeletal muscle after sprint interval training and detraining. Am J Physiol Regul Integr Comp Physiol 292:1970–1976
Centers for Disease Control and Prevention (2016) What is prediabetes? https://www.cdc.gov/diabetes/basics/prediabetes.html. Accessed 23 Oct 2017
Craig C, Marshall A, Sjostrom M, Bauman A, Booth M, Ainsworth B, Pratt M et al (2003) International physical activity questionnaire: 12-country reliability and validity. Med Sci Sports Exerc 35(8):1381–1395
Elobeid MA, Padilla MA, McVie T, Thomas O, Brock DW, Musser B, Lu K et al (2009) Missing data in randomized clinical trials for weight loss: scope of the problem, state of the field, and performance of statistical methods. PLoS ONE 4(8):e6624
Gilbertson NM, Eichner NZM, Francois M, Gaitán JM, Heiston EM, Weltman A, Malin S (2018) Glucose tolerance is linked to postprandial fuel use independent of exercise dose. Med Sci Sports Exerc. https://doi.org/10.1249/MSS.0000000000001667
Gillies C, Abrams K, Lambert P, Cooper N, Sutton A, Hsu R, Sutton A (2007) Pharmacological and lifestyle interventions to prevent or delay type 2 diabetes in people with impaired glucose tolerance: systematic review and meta-analysis. BMJ 334:299
Hazell T, Olver T, Hamilton C, Lemon P (2012) Two minutes of sprint-interval exercise elicits 24-hr oxygen consumption similar to that of 30 min of continuous endurance exercise. Int J Sport Nutr Exerc Metab 22:276–283
Hazell T, Hamilton C, Olver T, Lemon P (2014) Run sprint interval training induces fat loss in women. Appl Physiol Nutr Metab 39(8):944–950
Hughes V, Fiatarone M, Fielding R, Kahn B, Ferrara C, Shepherd P, Fisher E et al (1993) Exercise increase muscle GLUT-4 levels and insulin action in subjects with impaired glucose tolerance. Am J Physiol 264:E855–E862
Jakicic JM, Marcus BH, Gallagher KI (2003) Effect of exercise duration and intensity on weight loss in overweight, sedentary women. JAMA 290(10):1323–1330
Jin J (2014) Running injuries. JAMA 312(2):202
Kendzierski D, DeCarlo KJ (1991) Physical activity enjoyment scale: two validation studies. J Sport Exerc Psychol 13(1):50–64
Khaw KT, Wareham N, Luben R, Bingham S, Oakes S, Welch A, Day N (2001) Glycated hemoglobin, diabetes, and mortality in men in Norfolk cohort of European Prospective Investigation of Cancer and Nutrition (EPIC-Norfolk). BMJ 322(7277):15
Korkiakangas E, Alahuhta M, Husman P, Keinanen-Kiukaanniemi S, Taanila A, Laitinen J (2011) Motivators and barriers to exercise among adults with a high risk of type 2 diabetes—a qualitative study. Scand J Caring Sci 25:62–69
Linke SE, Gallo LC, Norman GJ (2011) Attrition and adherence rates of sustained vs. intermittent exercise interventions. Ann Behav Med 42(2):197–209
Little JP, Gillen JB, Percival ME et al (2011) Low-volume high-intensity interval training reduces hyperglycemia and increases muscle mitochondrial capacity in patients with type 2 diabetes. J Appl Physiol 111(6):1554–1560
Lunt H, Draper N, Marshall HC, Logan FJ, Hamlin MJ, Shearman JP, Cotter JD et al (2014) High intensity interval training in a real world setting: a randomized controlled feasibility study in overweight inactive adults, measuring change in maximal oxygen uptake. PLoS ONE 9(1):e83256
Macpherson R, Hazell T, Olver T, Paterson D, Lemon P (2010) Run sprint interval training improves aerobic performance but not maximal cardiac output. Med Sci Sports Exerc 43(1):115–122
Matthews D, Hosker J, Rudenski A, Naylor B, Treacher D, Turner R (1985) Homeostasis model assessment: insulin resistance and beta-cell function from fasting plasma glucose and insulin concentrations in man. Diabetologia 28(7):412–419
Mayer-Davis E, D’Agostino R, Karter A, Haffner S, Rewers M, Saad M, Bergman R (1998) Intensity and amount of physical activity in relation to insulin sensitivity. JAMA 279:669–674
Metcalfe R, Babraj J, Fawkner S, Vollaard N (2012) Towards the minimal amount of exercise for improving metabolic health: beneficial effects of reduced-exertion high-intensity interval exercise. Eur J Appl Physiol 112:2767–2775
Mullen S, Phillips S, Szabo A, Wohcicki T, Mailey E, Gothe N, Fanning J et al (2011) Measuring enjoyment of physical activity in older adults: invariance of the physical activity enjoyment scale across groups and time. Int J Behav Nutr Phys Act 8:103
Mullen S, Wojcicki T, Mailey E, Szabo A, Gothe N, Olson E, Fanning J et al (2013) A profile for predicting attrition from exercise in older adults. Prev Sci 14(5):489–496
Nybo L, Sundstrup E, Jakobsen MD, Mohr M, Hornstrup T, Simonsen L, Bulow J et al (2010) High-intensity training versus traditional exercise interventions for promoting health. Med Sci Sports Exerc 42(10):1951–1958
Perseghin G, Price T, Petersen K, Roden M, Cline G, Gerow K, Rothman D et al (1996) Increased glucose transport-phosphorylation and muscle glycogen synthesis after exercise training in insulin-resistant subjects. N Engl J Med 335:1357–1362
Pollock M, Gettman L, Milesis C, Bah M, Durstine L, Johnson R (1977) Effects of frequency and duration of training on attrition and incidence of injury. Med Sci Sports Exerc 9:31–36
Rowley T, Espinoza J, Akers J, Wenos D, Edwards E (2017) Effects of run sprint interval training on healthy, inactive, overweight/obese women: a pilot study. FACETS 2:53–67
Sandvei M, Jeppesen P, Stoen L, Litleskare S, Johansen T, Strensrud T, Enoksen E et al (2012) Sprint interval running increases insulin sensitivity in young healthy subjects. Arch Physiol Biochem 118:139–147
Schjerve IE, Tyldum GA, Tjonna AE, Stolen T, Loennechen JP, Hansen HEM, Haram PM et al (2008) Both aerobic endurance and strength training programmes improve cardiovascular health in obese adults. Clin Sci 115:283–293
Streiner D, Geddes J (2001) Intention to treat analysis in clinical trials where there are missing data. Evid Based Ment Health 4:70–71
Stutts W (2002) Physical activity determinants in adults perceived benefits, barriers, and self efficacy. AAOHN J 50:499–507
Taylor L, Spence J, Raine K, Plotnikoff R, Vallance J, Sharma A (2010) Physical activity and health-related quality of life in individuals with prediabetes. Diabetes Res Clin Pract 90:15–21
Terada T, Friesen A, Chahal B, Bell G, McCargar L, Boule N (2013) Feasibility and preliminary efficacy of high intensity interval training in type 2 diabetes. Diabetes Res Clin Pract 99:120–129
The Diabetes Prevention Program Research Group (1999) Design and methods for a clinical trial in the prevention of type 2 diabetes. Diabetes Care 22:623–634
The Diabetes Prevention Program Research Group (2002) Reduction in the incidence of type 2 diabetes with lifestyle intervention or metformin. N Engl J Med 346:393–403
Tibana RA, de Sousa NMF (2018) Are extreme condition programmes effective and safe? A narrative review of high-intensity functional training methods research paradigms and findings. BMJ Open Sport Exerc Med 4:ee000435
Tomlin DL, Wenger HA (2001) The relationship between aerobic fitness and recovery from high intensity intermittent exercise. Sports Med 31(1):1–11
Acknowledgements
Thank you to Sentara-Rockingham Memorial Regional Hospital Medical Center (Harrisonburg, VA) and the Human Performance Laboratory at James Madison University for the support and assistance throughout the project. We would like to express our gratitude to all the undergraduate research assistants, especially Kevin Decker, who helped with data collection and training sessions. This project would not have been possible without the excellent efforts of our study participants.
Funding
This study was funded by Sentara-Rockingham Memorial Regional Hospital (Harrisonburg, VA) and an Inter-Professional Education Grant through the College of Health and Behavioral Studies at James Madison University.
Author information
Authors and Affiliations
Contributions
NMG and ESE were primarily responsible for analyzing data and writing this manuscript. JDA, TAH, DLW and ESE were responsible for the study design and obtaining funding. NMG, JAM, and KH recruited participants, collected data, trained participants, and maintained data. JDA reviewed and analyzed food logs. All the authors edited this manuscript and approved submission.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Communicated by Philip D. Chilibeck.
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Gilbertson, N.M., Mandelson, J.A., Hilovsky, K. et al. Combining supervised run interval training or moderate-intensity continuous training with the diabetes prevention program on clinical outcomes. Eur J Appl Physiol 119, 1503–1512 (2019). https://doi.org/10.1007/s00421-019-04137-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00421-019-04137-2