Abstract
Purpose
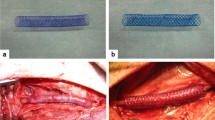
This study was designed to evaluate performance and tissue response to a self-expandable bioabsorbable vein stent-base cut from a tube with enhanced stiffness and strength in vitro and in vivo.
Methods
A diamond-shaped stent-base was cut from a sequential biaxially strained poly(l-lactide) (PLLA) tube for optimized performance. The performance of the stent-base was evaluated in a finite element analysis model, and validation was attempted in vitro through a cyclic flat-plate compression and radial force measurement. The performance of the stent-base was tested in vivo using 3 sheep with 2 implants each for 2 and 3½ weeks, respectively.
Results
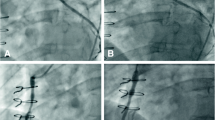
In vitro the stent-base showed an elliptical deformation but no fractures. In vivo the stent-base showed adequate radial force and no migration. All implanted stent-bases showed multiple fractures not only at the predicted stress zones but at all connecting points. Fragments of the caudal stent-base stayed in the vein wall indicating sufficient tissue coverage to avoid embolization of the fractured stent pieces, whereas fragments from the cranial device remaining were few. Neointima formation was confirmed histologically at 2 and 3½ weeks.
Conclusion
A bioabsorbable self-expandable stent-base made from PLLA for large veins seems feasible, but over time, the PLLA used in this study appears too stiff and lacks the sufficient flexibility to move with the vena cava, causing multiple fractures.







Similar content being viewed by others
References
Nagata T, Makutani S, Uchida H, Kichikawa K, Maeda M, Yoshioka T, Anai H, Sakaguchi H, Yoshimura H. Follow-up results of 71 patients undergoing metallic stent placement for the treatment of a malignant obstruction of the superior vena cava. Cardiovasc Intervent Radiol. 2007;30:959–67.
Imberti D, Ageno W, Dentali F, Donadini M, Mandredini R, Gallerani M. Retrievable vena cava filters: a clinical review. J Thromb Thrombolysis. 2012;33:258–66.
Rizvi AZ, Kalra M, Bjarnason H, Bower TC, Schleck C, Gloviczi P. Benign superior vena cava syndrome: stenting is now the first line of treatment. J Vasc Surg. 2008;47:372–80.
Nuutinen J, Clerc C, Törmälä P. Mechanical properties and in vitro degradation of bioabsorbable self-expanding braided stents. J Biomater Sci Polymer Edn. 2003;14:667–87.
Hayman D, Bergsson C, Miller S, Moreno M, Moore JE. The effect of static and dynamic loading on degradation of PLLA stent fibers. J Biomech Eng. 2014;136:1–9.
Welch TR, Eberhart RC, Reisch J, Chuong C. Influence of thermal annealing on the mechanical properties of PLLA coiled stents. Cardiovasc Eng Technol. 2014;5:270–80.
Vaazjanen A, Nuutinen J, Isotalo T, Törmälä P, Tammela TLJ, Talja M. Expansion and fixation properties of a new braided bioabsorbable urethral stent: an experimental study in the rabbit. J Urol. 2003;169:1171–4.
Wu Y, Shen L, Wang Q, Ge L, Xie J, Hu X, Sun A, Qian J. Comparison of acute recoil between bioabsorbable poly-l-lactic acid XINSORB stent and metallic stent in porcine model. J Biomed Biotechnol. 2012;13:1–8.
Ormiston JA, Serruys PW. Bioabsorbable coronary stents. Circ Cardiovasc Intervent. 2009;2:255–60.
Ginsberg G, Shah J, Carty A, Kaufmann C, Nuutinen J, Törmäla P. In vivo evaluation of a new bioabsorbable self-expanding biliary stent. Gastrointest Endosc. 2003;58:777–84.
Mario CD, Borgia F. Assimilating the current clinical data of fully bioabsorbable stents. EuroIntervention Suppl. 2009;5:103–8.
Thomas SD, Ofri A, Tang T, Englund R. Endovascular reconstruction of an interrupted inferior vena cava. Int J Surg Case Rep. 2014;5:59–62.
Lasprilla AJR, Martinez GAR, Lunelli BH, Jardini AL, Filho RM. Poly-lactic acid synthesis for application in biomedical devices—a review. Biotechnol Adv. 2012;30:321–8.
Nair LS, Laurencin CT. Biodegradable polymers as biomaterials. Prog Polym Sci. 2007;32:762–98.
Van Ditzhuijzen NS, Karanosos A, Van der Sijde JN, Van Soest G, Regar E. Bioabsorbable stent. In: Jang I, editor. Cardiovascular OCT imaging. Dordrecht: Springer; 2015. p. 179–93.
Zhang F, Hailei L, Liang G, Zhang H. Development and evaluation of a new biodegradable vena cava filter in a canine model. Asian J Surg. 2015;xx:1–5.
Eggers MD, McArthurt MJ, Figueira TA, Abdelsalam ME, Dixon KP, Pageon LR, Wallace MJ, Huang SY. Pilot in vivo study of an absorbable polydioxanone vena cava filter. J Vasc Surg. 2015;3:409–20.
Ou X, Cakmak M. Comparative study on development of structural hierarchy in constrained annealed simultaneous and sequential biaxially stretched polylactic acid films. Polymer. 2010;51:783–92.
Tsai C, Wu R, Cheng H, Li S, Siao Y, Kong D, Jang G. Crystallinity and dimensional stability of biaxial oriented poly(lactic acid) films. Polym Degrad Stab. 2010;95:1292–8.
Wu J, Yen M, Wu C, Li C, Kuo MC. Effect of biaxial stretching on thermal properties, shrinkage and mechanical properties of poly (lactic acid) films. J Polym Environ. 2013;21:303–11.
Løvdal A, Andreasen JW, Mikkelsen LP, Agersted K, Almdal K. Characterization of biaxial strain of poly(l-lactide) tubes. Polym Int. 2016;65:133–41.
Lingaiah K. Machine design data handbook. New York: McGraw-Hill; 1994.
Wallace DJ, Allision M, Stone MB. Inferior vena cava percentage collapse during respiration is affected by the sampling location: an ultrasound study in healthy volunteers. Acad Emergy Med. 2010;17:96–9.
Maddox S. Measuring vital in signs. In: Baillie L, editor. Developing practical adult nursing skills. Fargo: CRC Press Taylor & Francis; 2009. p. 116–518.
Ke MT, Fujimoto S, Imai T. SeeDB: a simple and morphology-preserving optical clearing agent for neuronal circuit reconstruction. Nat Neurosci. 2013;16:1154–61.
Calve S, Ready A, Huppenbauer C, Main R, Neu CP. Optical clearing in dense connective tissues to visualize cellular connectivity in situ. PLoS ONE. 2015;10:1–14.
Vieira AC, Guedes RM, Tita V. Considerations for the design of polymeric biodegradable products. J Polym Eng. 2013;33:292–302.
Irving JD, Dondelinger RF, Reidy JF, Schild H, Dick R, Adam A, Maynar M, Zollikofer CL. Gianturco serf-expanding stents: clinical experience in the vena cava and large veins. Cardiovasc Intervent Radiol. 1992;15:328–33.
Johnston CR, Lee K, Flewitt J, Moore R, Dobson GM, Thornton GM. The mechanical properties of endovascular stents: an in vitro assessment. Cardiovasc Eng. 2010;10:128–35.
Miyazaki K, Nishibe T, Manase H, Ohkashiwa H, Takahashi T, Watanabe S, Katoh H, Morita Y. Gianturco stents for the venous system: a detailed pathological study. Jpn J Surg. 1998;28:396–400.
Acknowledgement
The authors thank the Non-clinical Testing Team at Cook Research Incorporated for conducting the animal study.
Funding
This study was funded by Innovation Fund Denmark.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Studied sponsored by William Cook Europe as a part of the Industrial PhD Program.
Ethical approval
All applicable international, national, and/or institutional guidelines for the care and use of animals were followed.
Rights and permissions
About this article
Cite this article
Løvdal, A.L.V., Calve, S., Yang, S. et al. Evaluation of a Bioabsorbable Self-Expandable Vein Stent-Base Made of Poly(l-lactide) In Vitro and In Vivo. Cardiovasc Intervent Radiol 40, 112–119 (2017). https://doi.org/10.1007/s00270-016-1491-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00270-016-1491-2