Abstract
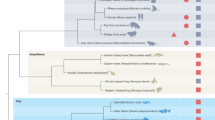
The neonatal capacity for cardiac regeneration in mice is well studied and has been used to develop many potential strategies for adult cardiac regenerative repair following injury. However, translating these findings from rodents to designing regenerative therapeutics for adult human heart disease remains elusive. Large mammals including pigs, dogs, and sheep are widely used as animal models of humans in preclinical trials of new cardiac drugs and devices. However, very little is known about the fundamental cardiac cell biology and the timing of postnatal cardiac events that influence cardiomyocyte proliferation in these animals. There is emerging evidence that external physiological and environmental cues could be the key to understanding cardiomyocyte proliferative behavior. In this review, we survey available literature on postnatal development in various large mammal models to offer a perspective on the physiological and cellular characteristics that could be regulating cardiomyocyte proliferation. Similarities and differences between developmental milestones, cardiomyocyte maturational events, as well as environmental cues regulating cardiac development, are discussed for various large mammals, with a focus on postnatal cardiac regenerative potential and translatability to the human heart.


Similar content being viewed by others
References
Bui AL, Horwich TB, Fonarow GC (2011) Epidemiology and risk profile of heart failure. Nat Rev Cardiol 8:30–41
Oster ME, Lee KA, Honein MA, Riehle-Colarusso T, Shin M, Correa A (2013) Temporal trends in survival among infants with critical congenital heart defects. Pediatrics 131:e1502–1508
Porrello ER, Mahmoud AI, Simpson E, Hill JA, Richardson JA, Olson EN, Sadek HA (2011) Transient regenerative potential of the neonatal mouse heart. Science 331:1078–1080
Haubner BJ, Adamowicz-Brice M, Khadayate S, Tiefenthaler V, Metzler B, Aitman T, Penninger JM (2012) Complete cardiac regeneration in a mouse model of myocardial infarction. Aging 4:966–977
Tzahor E, Poss KD (2017) Cardiac regeneration strategies: staying young at heart. Science 356:1035–1039
Wang J, Liu S, Heallen T, Martin JF (2018) The Hippo pathway in the heart: pivotal roles in development, disease, and regeneration. Nat Rev Cardiol 15:672–684
Rumyantsev P (1991) Growth and hyperplasia of cardiac muscle cells. Taylor & Francis, Milton Park
Vivien CJ, Hudson JE, Porrello ER (2016) Evolution, comparative biology and ontogeny of vertebrate heart regeneration. NPJ Regen Med 1:16012
Foglia MJ, Poss KD (2016) Building and re-building the heart by cardiomyocyte proliferation. Development 143:729–740
Mollova M, Bersell K, Walsh S, Savla J, Das LT, Park SY, Silberstein LE, Dos Remedios CG, Graham D, Colan S, Kuhn B (2013) Cardiomyocyte proliferation contributes to heart growth in young humans. Proc Natl Acad Sci USA 110:1446–1451
Bergmann O, Bhardwaj RD, Bernard S, Zdunek S, Barnabe-Heider F, Walsh S, Zupicich J, Alkass K, Buchholz BA, Druid H, Jovinge S, Frisen J (2009) Evidence for cardiomyocyte renewal in humans. Science 324:98–102
Bergmann O, Zdunek S, Felker A, Salehpour M, Alkass K, Bernard S, Sjostrom SL, Szewczykowska M, Jackowska T, Dos Remedios C, Malm T, Andra M, Jashari R, Nyengaard JR, Possnert G, Jovinge S, Druid H, Frisen J (2015) Dynamics of cell generation and turnover in the human heart. Cell 161:1566–1575
Haubner BJ, Schneider J, Schweigmann U, Schuetz T, Dichtl W, Velik-Salchner C, Stein JI, Penninger JM (2016) Functional recovery of a human neonatal heart after severe myocardial infarction. Circ Res 118:216–221
Oberpriller JO, Oberpriller JC (1974) Response of the adult newt ventricle to injury. J Exp Zool 187:249–253
Poss KD, Wilson LG, Keating MT (2002) Heart regeneration in zebrafish. Science 298:2188–2190
Kikuchi K, Holdway JE, Werdich AA, Anderson RM, Fang Y, Egnaczyk GF, Evans T, Macrae CA, Stainier DY, Poss KD (2010) Primary contribution to zebrafish heart regeneration by gata4(+) cardiomyocytes. Nature 464:601–605
de Pater E, Clijsters L, Marques SR, Lin YF, Garavito-Aguilar ZV, Yelon D, Bakkers J (2009) Distinct phases of cardiomyocyte differentiation regulate growth of the zebrafish heart. Development 136:1633–1641
Cao J, Poss KD (2018) The epicardium as a hub for heart regeneration. Nat Rev Cardiol 15:631–647
Gonzalez-Rosa JM, Sharpe M, Field D, Soonpaa MH, Field LJ, Burns CE, Burns CG (2018) Myocardial polyploidization creates a barrier to heart regeneration in zebrafish. Dev Cell 44(433–446):e437
Gunthel M, Barnett P, Christoffels VM (2018) Development, proliferation, and growth of the mammalian heart. Mol Ther 26:1599–1609
Lavine KJ, Epelman S, Uchida K, Weber KJ, Nichols CG, Schilling JD, Ornitz DM, Randolph GJ, Mann DL (2014) Distinct macrophage lineages contribute to disparate patterns of cardiac recovery and remodeling in the neonatal and adult heart. Proc Natl Acad Sci USA 111:16029–16034
Patterson M, Barske L, Van Handel B, Rau CD, Gan P, Sharma A, Parikh S, Denholtz M, Huang Y, Yamaguchi Y, Shen H, Allayee H, Crump JG, Force TI, Lien CL, Makita T, Lusis AJ, Kumar SR, Sucov HM (2017) Frequency of mononuclear diploid cardiomyocytes underlies natural variation in heart regeneration. Nat Genet 49:1346–1353
Qian L, Huang Y, Spencer CI, Foley A, Vedantham V, Liu L, Conway SJ, Fu JD, Srivastava D (2012) In vivo reprogramming of murine cardiac fibroblasts into induced cardiomyocytes. Nature 485:593–598
Yahalom-Ronen Y, Rajchman D, Sarig R, Geiger B, Tzahor E (2015) Reduced matrix rigidity promotes neonatal cardiomyocyte dedifferentiation, proliferation and clonal expansion. Elife 4:e07455
Li Y, Asfour H, Bursac N (2017) Age-dependent functional crosstalk between cardiac fibroblasts and cardiomyocytes in a 3D engineered cardiac tissue. Acta Biomater 55:120–130
Aurora AB, Porrello ER, Tan W, Mahmoud AI, Hill JA, Bassel-Duby R, Sadek HA, Olson EN (2014) Macrophages are required for neonatal heart regeneration. J Clin Invest 124:1382–1392
Puente BN, Kimura W, Muralidhar SA, Moon J, Amatruda JF, Phelps KL, Grinsfelder D, Rothermel BA, Chen R, Garcia JA, Santos CX, Thet S, Mori E, Kinter MT, Rindler PM, Zacchigna S, Mukherjee S, Chen DJ, Mahmoud AI, Giacca M, Rabinovitch PS, Aroumougame A, Shah AM, Szweda LI, Sadek HA (2014) The oxygen-rich postnatal environment induces cardiomyocyte cell-cycle arrest through DNA damage response. Cell 157:565–579
Nakada Y, Canseco DC, Thet S, Abdisalaam S, Asaithamby A, Santos CX, Shah AM, Zhang H, Faber JE, Kinter MT, Szweda LI, Xing C, Hu Z, Deberardinis RJ, Schiattarella G, Hill JA, Oz O, Lu Z, Zhang CC, Kimura W, Sadek HA (2017) Hypoxia induces heart regeneration in adult mice. Nature 541:222–227
Hirose K, Payumo AY, Cutie S, Hoang A, Zhang H, Guyot R, Lunn D, Bigley RB, Yu H, Wang J, Smith M, Gillett E, Muroy SE, Schmid T, Wilson E, Field KA, Reeder DM, Maden M, Yartsev MM, Wolfgang MJ, Grutzner F, Scanlan TS, Szweda LI, Buffenstein R, Hu G, Flamant F, Olgin JE, Huang GN (2019) Evidence for hormonal control of heart regenerative capacity during endothermy acquisition. Science 364:184–188
Camacho P, Fan H, Liu Z, He JQ (2016) Large mammalian animal models of heart disease. J Cardiovasc Dev Dis 3(4):30
Ye L, D'Agostino G, Loo SJ, Wang CX, Su LP, Tan SH, Tee GZ, Pua CJ, Pena EM, Cheng RB, Chen WC, Abdurrachim D, Lalic J, Tan RS, Lee TH, Zhang J, Cook SA (2018) Early regenerative capacity in the porcine heart. Circulation 138:2798–2808
Zhu W, Zhang E, Zhao M, Chong Z, Fan C, Tang Y, Hunter JD, Borovjagin AV, Walcott GP, Chen JY, Qin G, Zhang J (2018) Regenerative potential of neonatal porcine hearts. Circulation 138:2809–2816
Nagy A, Gertsenstein M, Vintersten K, Behringer R (2003) Manipulating the mouse embryo: a laboratory manual. Firefly Books, Richmond Hill
de Magalhaes JP, Costa J (2009) A database of vertebrate longevity records and their relation to other life-history traits. J Evol Biol 22:1770–1774
Cutler RG (1979) Evolution of human longevity: a critical overview. Mech Ageing Dev 9:337–354
Finn CA (1963) Reproductive capacity and litter size in mice: effect of age and environment. J Reprod Fertil 6:205–214
Chen P, Baas TJ, Mabry JW, Koehler KJ, Dekkers JC (2003) Genetic parameters and trends for litter traits in U.S. Yorkshire, Duroc, Hampshire, and Landrace pigs. J Anim Sci 81:46–53
Okkens AC, Hekerman TW, de Vogel JW, van Haaften B (1993) Influence of litter size and breed on variation in length of gestation in the dog. Vet Q 15:160–161
Janssens S, Vandepitte W, Bodin L (2004) Genetic parameters for litter size in sheep: natural versus hormone-induced oestrus. Genet Sel Evol 36:543–562
Silva del Rio N, Stewart S, Rapnicki P, Chang YM, Fricke PM (2007) An observational analysis of twin births, calf sex ratio, and calf mortality in Holstein dairy cattle. J Dairy Sci 90:1255–1264
Poore KR, Fowden AL (2004) The effects of birth weight and postnatal growth patterns on fat depth and plasma leptin concentrations in juvenile and adult pigs. J Physiol 558:295–304
Sibly RM, Brown JH (2009) Mammal reproductive strategies driven by offspring mortality-size relationships. Am Nat 173:E185–199
Li F, Wang X, Capasso JM, Gerdes AM (1996) Rapid transition of cardiac myocytes from hyperplasia to hypertrophy during postnatal development. J Mol Cell Cardiol 28:1737–1746
Beinlich CJ, Rissinger CJ, Morgan HE (1995) Mechanisms of rapid growth in the neonatal pig heart. J Mol Cell Cardiol 27:273–281
Peterson CJ, Whitman V, Watson PA, Schuler HG, Morgan HE (1989) Mechanisms of differential growth of heart ventricles in newborn pigs. Circ Res 64:360–369
Grabner W, Pfitzer P (1974) Number of nuclei in isolated myocardial cells of pigs. Virchows Arch B Cell Pathol 15:279–294
Kirk GR, Smith DM, Hutcheson DP, Kirby R (1975) Postnatal growth of the dog heart. J Anat 119:461–469
Bishop SP, Hine P (1975) Cardiac muscle cytoplasmic and nuclear development during canine neonatal growth. Recent Adv Stud Cardiac Struct Metab 8:77–98
Munnell JF, Getty R (1968) Rate of accumulation of cardiac lipofuscin in the aging canine. J Gerontol 23:154–158
Thornburg K, Jonker S, O'Tierney P, Chattergoon N, Louey S, Faber J, Giraud G (2011) Regulation of the cardiomyocyte population in the developing heart. Prog Biophys Mol Biol 106:289–299
Jonker SS, Louey S, Giraud GD, Thornburg KL, Faber JJ (2015) Timing of cardiomyocyte growth, maturation, and attrition in perinatal sheep. FASEB J 29:4346–4357
Burrell JH, Boyn AM, Kumarasamy V, Hsieh A, Head SI, Lumbers ER (2003) Growth and maturation of cardiac myocytes in fetal sheep in the second half of gestation. Anat Rec A Discov Mol Cell Evol Biol 274:952–961
Soonpaa MH, Kim KK, Pajak L, Franklin M, Field LJ (1996) Cardiomyocyte DNA synthesis and binucleation during murine development. Am J Physiol 271:H2183–2189
Soonpaa MH, Zebrowski DC, Platt C, Rosenzweig A, Engel FB, Field LJ (2015) Cardiomyocyte cell-cycle activity during preadolescence. Cell 163:781–782
Adler CP, Friedburg H, Herget GW, Neuburger M, Schwalb H (1996) Variability of cardiomyocyte DNA content, ploidy level and nuclear number in mammalian hearts. Virchows Arch 429:159–164
Chen X, Wilson RM, Kubo H, Berretta RM, Harris DM, Zhang X, Jaleel N, MacDonnell SM, Bearzi C, Tillmanns J, Trofimova I, Hosoda T, Mosna F, Cribbs L, Leri A, Kajstura J, Anversa P, Houser SR (2007) Adolescent feline heart contains a population of small, proliferative ventricular myocytes with immature physiological properties. Circ Res 100:536–544
Kim MY, Eiby YA, Lumbers ER, Wright LL, Gibson KJ, Barnett AC, Lingwood BE (2014) Effects of glucocorticoid exposure on growth and structural maturation of the heart of the preterm piglet. PLoS ONE 9:e93407
Pfitzer P (1971) Polyploid nuclei in myocardial cells of the pig. Virchows Arch B Cell Pathol 9:180–186
Bensley JG, De Matteo R, Harding R, Black MJ (2016) Three-dimensional direct measurement of cardiomyocyte volume, nuclearity, and ploidy in thick histological sections. Sci Rep 6:23756
Pfitzer P (1972) Polyploid nuclei in myocardial cells of monkeys. Virchows Arch B Cell Pathol 10:268–274
Olivetti G, Cigola E, Maestri R, Corradi D, Lagrasta C, Gambert SR, Anversa P (1996) Aging, cardiac hypertrophy and ischemic cardiomyopathy do not affect the proportion of mononucleated and multinucleated myocytes in the human heart. J Mol Cell Cardiol 28:1463–1477
Ascuitto RJ, Ross-Ascuitto NT (1996) Substrate metabolism in the developing heart. Semin Perinatol 20:542–563
Doenst T, Nguyen TD, Abel ED (2013) Cardiac metabolism in heart failure: implications beyond ATP production. Circ Res 113:709–724
Makinde AO, Kantor PF, Lopaschuk GD (1998) Maturation of fatty acid and carbohydrate metabolism in the newborn heart. Mol Cell Biochem 188:49–56
Werner JC, Whitman V, Fripp RR, Schuler HG, Morgan HE (1981) Carbohydrate metabolism in isolated, working newborn pig heart. Am J Physiol 241:E364–371
Werner JC, Whitman V, Vary TC, Fripp RR, Musselman J, Schuler HG (1983) Fatty acid and glucose utilization in isolated, working newborn pig hearts. Am J Physiol 244:E19–23
Werner JC, Sicard RE, Schuler HG (1989) Palmitate oxidation by isolated working fetal and newborn pig hearts. Am J Physiol 256:E315–321
Ascuitto RJ, Ross-Ascuitto NT, Chen V, Downing SE (1989) Ventricular function and fatty acid metabolism in neonatal piglet heart. Am J Physiol 256:H9–15
Breuer E, Barta E, Pappova E, Zlatos L (1967) Developmental changes of myocardial metabolism. I. Peculiarities of cardiac carbohydrate metabolism in early postnatal period in dogs. Biologia Neonatorum 11:367–370
Fisher DJ, Heymann MA, Rudolph AM (1980) Myocardial oxygen and carbohydrate consumption in fetal lambs in utero and in adult sheep. Am J Physiol 238:H399–405
Yin Z, Ren J, Guo W (2015) Sarcomeric protein isoform transitions in cardiac muscle: a journey to heart failure. Biochim Biophys Acta 1852:47–52
Saggin L, Gorza L, Ausoni S, Schiaffino S (1989) Troponin I switching in the developing heart. J Biol Chem 264:16299–16302
Posterino GS, Dunn SL, Botting KJ, Wang W, Gentili S (1985) Morrison JL (2011) Changes in cardiac troponins with gestational age explain changes in cardiac muscle contractility in the sheep fetus. J Appl Physiol 111:236–243
Locher MR, Razumova MV, Stelzer JE, Norman HS, Moss RL (2011) Effects of low-level α-myosin heavy chain expression on contractile kinetics in porcine myocardium. Am J Physiol Heart Circ Physiol 300:H869–878
Castro-Ferreira R, Fontes-Carvalho R, Falcao-Pires I, Leite-Moreira AF (2011) The role of titin in the modulation of cardiac function and its pathophysiological implications. Arq Bras Cardiol 96:332–339
Warren CM, Krzesinski PR, Campbell KS, Moss RL, Greaser ML (2004) Titin isoform changes in rat myocardium during development. Mech Dev 121:1301–1312
Opitz CA, Leake MC, Makarenko I, Benes V, Linke WA (2004) Developmentally regulated switching of titin size alters myofibrillar stiffness in the perinatal heart. Circ Res 94:967–975
Bassat E, Mutlak YE, Genzelinakh A, Shadrin IY, Baruch Umansky K, Yifa O, Kain D, Rajchman D, Leach J, Riabov Bassat D, Udi Y, Sarig R, Sagi I, Martin JF, Bursac N, Cohen S, Tzahor E (2017) The extracellular matrix protein agrin promotes heart regeneration in mice. Nature 547:179–184
Chen WC, Wang Z, Missinato MA, Park DW, Long DW, Liu HJ, Zeng X, Yates NA, Kim K, Wang Y (2016) Decellularized zebrafish cardiac extracellular matrix induces mammalian heart regeneration. Sci Adv 2:e1600844
Lewis AM, Mathieu-Costello O, McMillan PJ, Gilbert RD (1999) Effects of long-term, high-altitude hypoxia on the capillarity of the ovine fetal heart. Am J Physiol 277:H756–762
Li M, Iismaa SE, Naqvi N, Nicks A, Husain A, Graham RM (2014) Thyroid hormone action in postnatal heart development. Stem Cell Res 13:582–591
Fisher DA, Klein AH (1981) Thyroid development and disorders of thyroid function in the newborn. N Engl J Med 304:702–712
Chattergoon NN, Louey S, Stork P, Giraud GD, Thornburg KL (2012) Mid-gestation ovine cardiomyocytes are vulnerable to mitotic suppression by thyroid hormone. Reprod Sci 19:642–649
Karra R, Poss KD (2017) Redirecting cardiac growth mechanisms for therapeutic regeneration. J Clin Invest 127:427–436
Garbern JC, Mummery CL, Lee RT (2013) Model systems for cardiovascular regenerative biology. Cold Spring Harb Perspect Med 3:a014019
Best KE, Rankin J (2016) Long-term survival of individuals born with congenital heart disease: a systematic review and meta-analysis. J Am Heart Assoc 5:e002846
Triedman JK, Newburger JW (2016) Trends in congenital heart disease: the next decade. Circulation 133:2716–2733
Egbe AC, Mittnacht AJ, Nguyen K, Joashi U (2014) Risk factors for morbidity in infants undergoing tetralogy of fallot repair. Ann Pediatr Cardiol 7:13–18
Yutzey KE (2017) Cardiomyocyte proliferation: teaching an old dogma new tricks. Circ Res 120:627–629
Huttenbach Y, Ostrowski ML, Thaller D, Kim HS (2001) Cell proliferation in the growing human heart: MIB-1 immunostaining in preterm and term infants at autopsy. Cardiovasc Pathol 10:119–123
Amir G, Ma X, Reddy VM, Hanley FL, Reinhartz O, Ramamoorthy C, Riemer RK (2008) Dynamics of human myocardial progenitor cell populations in the neonatal period. Ann Thorac Surg 86:1311–1319
Silva TF, Souza GK, Simoes MA, Pabis FC, Noronha L (2012) Immunohistochemical expression of cell differentiation and growth in neonate cardiomyocytes. Arq Bras Cardiol 99:797–801
Ye L, Qiu L, Zhang H, Chen H, Jiang C, Hong H, Liu J (2016) Cardiomyocytes in young infants with congenital heart disease: a three-month window of proliferation. Sci Rep 6:23188
Schmid G, Pfitzer P (1985) Mitoses and binucleated cells in perinatal human hearts. Virchows Arch B Cell Pathol Incl Mol Pathol 48:59–67
Botting KJ, Wang KC, Padhee M, McMillen IC, Summers-Pearce B, Rattanatray L, Cutri N, Posterino GS, Brooks DA, Morrison JL (2012) Early origins of heart disease: low birth weight and determinants of cardiomyocyte endowment. Clin Exp Pharmacol Physiol 39:814–823
Eisenstein R, Wied GL (1970) Myocardial DNA and protein in maturing and hypertrophied human hearts. Proc Soc Exp Biol Med 133:176–179
Brodsky V, Sarkisov DS, Arefyeva AM, Panova NW, Gvasava IG (1994) Polyploidy in cardiac myocytes of normal and hypertrophic human hearts; range of values. Virchows Arch 424:429–435
Herget GW, Neuburger M, Plagwitz R, Adler CP (1997) DNA content, ploidy level and number of nuclei in the human heart after myocardial infarction. Cardiovasc Res 36:45–51
Iruretagoyena JI, Davis W, Bird C, Olsen J, Radue R, Teo Broman A, Kendziorski C, Splinter BonDurant S, Golos T, Bird I, Shah D (2014) Metabolic gene profile in early human fetal heart development. Mol Hum Reprod 20:690–700
Nakano H, Minami I, Braas D, Pappoe H, Wu X, Sagadevan A, Vergnes L, Fu K, Morselli M, Dunham C, Ding X, Stieg AZ, Gimzewski JK, Pellegrini M, Clark PM, Reue K, Lusis AJ, Ribalet B, Kurdistani SK, Christofk H, Nakatsuji N, Nakano A (2017) Glucose inhibits cardiac muscle maturation through nucleotide biosynthesis. Elife 6:e29330
Anderson PA, Malouf NN, Oakeley AE, Pagani ED, Allen PD (1991) Troponin T isoform expression in humans. A comparison among normal and failing adult heart, fetal heart, and adult and fetal skeletal muscle. Circ Res 69:1226–1233
Swynghedauw B (1986) Developmental and functional adaptation of contractile proteins in cardiac and skeletal muscles. Physiol Rev 66:710–771
Wilkinson JM, Grand RJ (1978) Comparison of amino acid sequence of troponin I from different striated muscles. Nature 271:31–35
Sasse S, Brand NJ, Kyprianou P, Dhoot GK, Wade R, Arai M, Periasamy M, Yacoub MH, Barton PJ (1993) Troponin I gene expression during human cardiac development and in end-stage heart failure. Circ Res 72:932–938
Reiser PJ, Portman MA, Ning XH, Schomisch Moravec C (2001) Human cardiac myosin heavy chain isoforms in fetal and failing adult atria and ventricles. Am J Physiol Heart Circ Physiol 280:H1814–1820
Ritter O, Luther HP, Haase H, Baltas LG, Baumann G, Schulte HD, Morano I (1999) Expression of atrial myosin light chains but not alpha-myosin heavy chains is correlated in vivo with increased ventricular function in patients with hypertrophic obstructive cardiomyopathy. J Mol Med (Berl) 77:677–685
Miyata S, Minobe W, Bristow MR, Leinwand LA (2000) Myosin heavy chain isoform expression in the failing and nonfailing human heart. Circ Res 86:386–390
Ledda-Columbano GM, Molotzu F, Pibiri M, Cossu C, Perra A, Columbano A (2006) Thyroid hormone induces cyclin D1 nuclear translocation and DNA synthesis in adult rat cardiomyocytes. FASEB J 20:87–94
Olivieri A, Stazi MA, Mastroiacovo P, Fazzini C, Medda E, Spagnolo A, De Angelis S, Grandolfo ME, Taruscio D, Cordeddu V, Sorcini M, Study Group for Congenital H (2002) A population-based study on the frequency of additional congenital malformations in infants with congenital hypothyroidism: data from the Italian Registry for Congenital Hypothyroidism (1991–1998). J Clin Endocrinol Metab 87:557–562
Chowdhury D, Ojamaa K, Parnell VA, McMahon C, Sison CP, Klein I (2001) A prospective randomized clinical study of thyroid hormone treatment after operations for complex congenital heart disease. J Thorac Cardiovasc Surg 122:1023–1025
Lockhart M, Wirrig E, Phelps A, Wessels A (2011) Extracellular matrix and heart development. Birth Defects Res A Clin Mol Teratol 91:535–550
McMahon CJ, Nihill MR, Denfield S (2003) Neoaortic root dilation associated with left coronary artery stenosis following arterial switch procedure. Pediatr Cardiol 24:43–46
Farooqi KM, Sutton N, Weinstein S, Menegus M, Spindola-Franco H, Pass RH (2012) Neonatal myocardial infarction: case report and review of the literature. Congenit Heart Dis 7:E97–102
Nakagama Y, Inuzuka R, Ichimura K, Hinata M, Takehara H, Takeda N, Kakiuchi S, Shiraga K, Asakai H, Shindo T, Hirata Y, Saitoh M, Oka A (2018) Accelerated cardiomyocyte proliferation in the heart of a neonate with LEOPARD syndrome-associated fatal cardiomyopathy. Circ Heart Fail 11:e004660
Tsang V, Yacoub M, Sridharan S, Burch M, Radley-Smith R, Khaghani A, Savoldo B, Amrolia PJ (2009) Late donor cardiectomy after paediatric heterotopic cardiac transplantation. Lancet 374:387–392
Fratz S, Hager A, Schreiber C, Schwaiger M, Hess J, Stern HC (2011) Long-term myocardial scarring after operation for anomalous left coronary artery from the pulmonary artery. Ann Thorac Surg 92:1761–1765
Wesselhoeft H, Fawcett JS, Johnson AL (1968) Anomalous origin of the left coronary artery from the pulmonary trunk. Its clinical spectrum, pathology, and pathophysiology, based on a review of 140 cases with seven further cases. Circulation 38:403–425
Porrello ER, Olson EN (2014) A neonatal blueprint for cardiac regeneration. Stem Cell Res 13:556–570
Godwin JW, Debuque R, Salimova E, Rosenthal NA (2017) Heart regeneration in the salamander relies on macrophage-mediated control of fibroblast activation and the extracellular landscape. NPJ Regen Med 2(1):22
Gray GA, Toor IS, Castellan R, Crisan M, Meloni M (2018) Resident cells of the myocardium: more than spectators in cardiac injury, repair and regeneration. Curr Opin Physiol 1:46–51
Acknowledgements
We thank members of the Yutzey lab for valuable input and discussion.
Funding
This study was funded by NIH R01HL135848, R01HL142217, and Cincinnati Children’s Research Foundation.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflict of interest to declare.
Research Involving Human and Animal Rights
This article does not contain any experiments with human participants or animals performed by any of the authors.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Velayutham, N., Agnew, E.J. & Yutzey, K.E. Postnatal Cardiac Development and Regenerative Potential in Large Mammals. Pediatr Cardiol 40, 1345–1358 (2019). https://doi.org/10.1007/s00246-019-02163-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00246-019-02163-7