Abstract
Rationale
Attentional biases and executive control deficits may play a role in smoking cessation failure.
Objectives
The object of this study was to determine whether smokers' pre-quit reaction times on a computerized modified Simon task (which assesses attentional biases and executive control deficits) predict abstinence following a quit attempt.
Methods
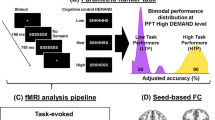
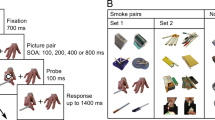
Participants (N = 365) in a larger smoking cessation clinical trial completed the modified Simon task twice (while 10-h nicotine-deprived vs. not deprived). In the task, two photographs (i.e., two digital slides) were displayed—one always neutral, the other positive, negative, smoking-relevant, or neutral. A probe (<<< or >>>) then appeared to the left or right of center, and participants indicated the arrow's direction (left or right) which was either congruent or incongruent with the arrow's location on the screen. The incongruency effect, a measure of executive control, was calculated by subtracting the reaction time to congruent probes from the reaction time to incongruent probes.
Results
Greater impairment in executive control (i.e., greater probe incongruency effects) after viewing positive and smoking slides relative to negative slides predicted an inability to establish initial cessation and to maintain abstinence up to 8 weeks post-quit.
Conclusions
These effects may be because smokers who avoid/escape from processing negative affect are more likely to fail in a cessation attempt. Differences in relatively automatic responses to affective cues distinguish smokers who are successful and unsuccessful in their smoking cessation attempts, but effects were modest in size.



Similar content being viewed by others
Notes
Trials involving two neutral slides were included as filler trials and were not analyzed.
The mean arousal and valence ratings for the smoking slides were computed for a set of 36 smoking slides developed by Shi (1998). The current study used a subset of 24 of those 36 smoking slides. Ratings for the individual slides were not accessible.
We also calculated the following attentional bias scores (by subtracting slide–probe match from slide–probe mismatch reaction times) for negative (M = 2 ms, SD = 67.6), positive (M = −3 ms, SD = 59.6), and smoking slides (M = 5 ms, SD = 68.2). These findings suggest there was not a meaningful effect of slide–probe match (i.e., sticky attention) for any of the slide types. Although the findings seemingly conflict with findings from the visual probe task discussed earlier, the current study used the modified Simon task which may explain the different findings.
As mentioned earlier, we selected short-term outcomes because we believed long-term outcomes would be less sensitive to baseline information processing biases and more sensitive to fortuitous events. When longer-term outcomes were examined (i.e., 6-month abstinence), task performance did not predict cessation outcome.
These findings were fairly robust when simple contrasts instead of planned Helmert contrasts were used for the Slide Type factor (i.e., when we first tested that the omnibus F-test was significant and then followed-up with simple contrasts for negative versus positive slides and for smoking versus negative slides). For three of the four cessation outcomes, the omnibus F-test showed that the Slide Type × Probe Congruency × Cessation Outcome Measure interaction was significant. (For the cessation outcome abstinence at 8 weeks post-quit, this interaction was not significant, although the effect was in the right direction, p = 0.09). We then followed up the three significant omnibus F-tests with simple contrasts. For the first simple contrasts (negative versus positive slides), the Slide Type (negative versus positive slides) × Probe Congruency × Cessation Outcome Measure interaction was significant for the three cessation outcomes. For the second simple contrasts (smoking versus negative slides), we found only a Slide Type (smoking versus negative slides) × Probe Congruency × Abstinence interaction at 1 week post-quit (p = 0.01).
References
Ayduk O, Mendoza-Denton R, Mischel W, Downey G, Peake PK, Rodriguez M (2000) Regulating the interpersonal self: strategic self-regulation for coping with rejection sensitivity. J Pers Soc Psychol 79:776–792
Baker TB, Piper ME, McCarthy DE, Majeskie MR, Fiore MC (2004) Addiction motivation reformulated: an affective processing model of negative reinforcement. Psychol Rev 111:33–51
Berridge KC (2007) The debate over dopamine's role in reward: the case for incentive salience. Psychopharmacol (Berl) 191:391–431
Bolt DM, Piper ME, McCarthy DE, Japuntich SJ, Fiore MC, Smith SS, Baker TB (2009) The Wisconsin predicting patients' relapse questionnaire. Nicotine Tob Res 11:481–492
Bradley B, Field M, Mogg K, De Houwer J (2004) Attentional and evaluative biases for smoking cues in nicotine dependence: component processes of biases in visual orienting. Behav Pharmacol 15:29–36
Brown RA, Lejuez CW, Kahler CW, Strong DR, Zvolensky MJ (2005) Distress tolerance and early smoking lapse. Clin Psychol Rev 25:713–733
Brown RA, Palm KM, Strong DR, Lejuez CW, Kahler CW, Zvolensky MJ, Hayes SC, Wilson KG, Gifford EV (2008) Distress tolerance treatment for early-lapse smokers: rationale, program description, and preliminary findings. Behav Modif 32:302–332
Cohen J (1992) A power primer. Psychol Bull 112:155–159
Cohen J, Cohen P, West SG, Aiken LS (2003) Applied multiple regression/correlation analysis in the behavioral sciences (3rd ed). Lawrence Erlbaum Associates, Lawrence Erlbaum Associates, Hillsdale, NJ
Cox WM, Fadardi JS, Pothos EM (2006) The addiction-Stroop test: theoretical considerations and procedural recommendations. Psychol Bull 132:443–476
Curtin JJ, McCarthy DE, Piper ME, Baker TB (2006) Implicit and explicit drug motivational processes: a model of boundary conditions. In: Weirs RW, Stacy AW (eds) Handbook of implicit cognition and addiction. Sage, Thousand Oaks, pp 233–250
Davis JM, Fleming MF, Bonus KA, Baker TB (2007) A pilot study on mindfulness based stress reduction for smokers. BMC Complement Altern Med 7:2
Dawkins L, Powell JH, West R, Powell J, Pickering A (2007) A double-blind placebo-controlled experimental study of nicotine: II—effects on response inhibition and executive functioning. Psychopharmacol (Berl) 190:457–467
Elliott R, Rubinsztein JS, Sahakian BJ, Dolan RJ (2002) The neural basis of mood-congruent processing biases in depression. Arch Gen Psychiatry 59:597–604
Erickson K, Drevets WC, Clark L, Cannon DM, Bain EE, Zarate CA Jr, Charney DS, Sahakian BJ (2005) Mood-congruent bias in affective go/no-go performance of unmedicated patients with major depressive disorder. Am J Psychiatry 162:2171–2173
Field M, Mogg K, Bradley BP (2004) Eye movements to smoking-related cues: effects of nicotine deprivation. Psychopharmacol (Berl) 173:116–123
Fiore MC, Jaen CR, Baker TB, Bailey WC, Benowitz N, Curry SJ, Dorfman SF, Froelicher ES, Goldstein MG, Healton CG, Henderson PN, Heyman RB, Koh HK, Kottke TE, Lando HA, Mecklenburg RE, Mermelstein RJ, Mullen PD, Orleans CT, Robinson L, Stitzer M, Tommasello AC, Villejo L, Wewers ME (2008) Treating tobacco use and dependence: 2008 update. Rockville, MD: US Department of Health and Human Services, US Public Health Service, US Department of Health and Human Services, US Public Health Service
Forster KI, Forster JC (2003) DMDX: a windows display program with millisecond accuracy. Behav Res Meth Instrum Comput 35:116–124
Fozard JL, Vercryssen M, Reynolds SL, Hancock PA, Quilter RE (1994) Age differences and changes in reaction time: the Baltimore Longitudinal Study of Aging. J Gerontol 49:179–189
Franken IH (2003) Drug craving and addiction: integrating psychological and neuropsychopharmacological approaches. Prog Neuropsychopharmacol Biol Psychiatry 27:563–579
Gifford EV, Kohlenberg BS, Hayes SC, Antonuccio DO, Piasecki MM, Rasmussen-Hall ML, Palm KM (2004) Acceptance-based treatment for smoking cessation. Behav Ther 35:689–705
Gloria R, Angelos L, Schaefer HS, Davis JM, Majeskie M, Richmond BS, Curtin JJ, Davidson RJ, Baker TB (2009) An fMRI investigation of the impact of withdrawal on regional brain activity during nicotine anticipation. Psychophysiology 46:681–693
Heatherton TF, Kozlowski LT, Frecker RC, Fagerstrom KO (1991) The Fagerstrom test for nicotine dependence: a revision of the Fagerstrom tolerance questionnaire. Br J Addict 86:1119–1127
Kashdan TB, Barrios V, Forsyth JP, Steger MF (2006) Experiential avoidance as a generalized psychological vulnerability: comparisons with coping and emotion regulation strategies. Behav Res Ther 44:1301–1320
Kenford SL, Smith SS, Wetter DW, Jorenby DE, Fiore MC, Baker TB (2002) Predicting relapse back to smoking: contrasting affective and physical models of dependence. J Consult Clin Psychol 70:216–227
Lang PJ, Bradley MM, Cuthbert BN (1999) International affective picture system (IAPS): Instruction manual and affective ratings. Technical Report A-4. Center for Research in Psychophysiology, University of Florida, Center for Research in Psychophysiology, Gainesville, FL: University of Florida
Leventhal AM, Waters AJ, Breitmeyer BG, Miller EK, Tapia E, Li Y (2008) Subliminal processing of smoking-related and affective stimuli in tobacco addiction. Exp Clin Psychopharmacol 16:301–312
Littel M, Franken IH (2007) The effects of prolonged abstinence on the processing of smoking cues: an ERP study among smokers, ex-smokers and never-smokers. J Psychopharmacol 21:873–882
Lu C-H, Proctor RW (1995) The influence of irrelevant location information on performance: a review of the Simon and spatial Stroop effects. Psychon Bull Rev 2:174–207
MacPherson L, Tull MT, Matusiewicz AK, Rodman S, Strong DR, Kahler CW, Hopko DR, Zvolensky MJ, Brown RA, Lejuez CW (2010) Randomized controlled trial of behavioral activation smoking cessation treatment for smokers with elevated depressive symptoms. J Consult Clin Psychol 78:55–61
McCarthy DE, Gloria R, Curtin JJ (2009) Attention bias in nicotine withdrawal and under stress. Psychol Addict Behav 23:77–90
Munafo M, Mogg K, Roberts S, Bradley BP, Murphy M (2003) Selective processing of smoking-related cues in current smokers, ex-smokers and never-smokers on the modified Stroop task. J Psychopharmacol 17:310–316
Olson SL, Schilling EM, Bates JE (1999) Measurement of impulsivity: construct coherence, longitudinal stability, and relationship with externalizing problems in middle childhood and adolescence. J Abnorm Child Psychol 27:151–165
Piper ME, Federmen EB, McCarthy DE, Bolt DM, Smith SS, Fiore MC, Baker TB (2008) Using mediational models to explore the nature of tobacco motivation and tobacco treatment effects. J Abnorm Psychol 117:94–105
Piper ME, Smith SS, Schlam TR, Fiore MC, Jorenby DE, Fraser D, Baker TB (2009) A randomized placebo-controlled clinical trial of five smoking cessation pharmacotherapies. Arch Gen Psychiatry 66:1253–1262
Shi F-Y (1998) Smoking motivation, nicotine withdrawal and the startle probe response. Dissertation, University of Wisconsin-Madison, Madison, WI
Shiffman S, Scharf DM, Shadel WG, Gwaltney CJ, Dang Q, Paton SM, Clark DB (2006) Analyzing milestones in smoking cessation: illustration in a nicotine patch trial in adult smokers. J Consult Clin Psychol 74:276–285
Shoda Y, Mischel W, Peake PK (1990) Predicting adolescent cognitive and self-regulatory competencies from preschool delay of gratification: identifying diagnostic conditions. Dev Psychol 26:978–986
Simon JR, Rudell AP (1967) Auditory S–R compatibility: the effect of an irrelevant cue on information processing. J Appl Psychol 51:300–304
Thush C, Wiers RW, Ames SL, Grenard JL, Sussmann S, Stacy AW (2008) Interactions between implicit and explicit cognition and working memory capacity in the prediction of alcohol use in at-risk adolescents. Drug Alcohol Depend 94:116–124
Tiffany ST (1990) A cognitive model of drug urges and drug-use behavior: role of automatic and nonautomatic processes. Psychol Rev 97:147–168
Waters AJ, Shiffman S, Bradley BP, Mogg K (2003a) Attentional shifts to smoking cues in smokers. Addiction 98:1409–1417
Waters AJ, Shiffman S, Sayette MA, Paty JA, Gwaltney CJ, Balabanis MH (2003b) Attentional bias predicts outcome in smoking cessation. Health Psychol 22:378–387
Welsch SK, Smith SS, Wetter DW, Jorenby DE, Fiore MC, Baker TB (1999) Development and validation of the Wisconsin Smoking Withdrawal Scale. Exp Clin Psychopharmacol 7:354–361
Wiers RW, Houben K, Smulders FTY, Conrod PJ, Jones BT (2006) To drink or not to drink: the role of automatic and controlled cognitive processes in the etiology of alcohol-related problems. In: Wiers RW, Stacy AW (eds) Handbook of implicit cognition and addiction. Sage, Thousand Oaks, pp 339–361
Williams JMG, Mathews A, MacLeod C (1996) The emotional Stroop task and psychopathology. Psychol Bull 120:3–24
Acknowledgments
Tanya R. Schlam, Sandra J. Japuntich, Megan E. Piper, Rebecca Gloria, and John J. Curtin have no potential conflicts of interest to disclose. Timothy B. Baker has served as an investigator on research projects sponsored by pharmaceutical companies including Pfizer, Glaxo Wellcome, Sanofi, and Nabi.
This research was conducted at the University of Wisconsin-Madison and was supported by grant #P50 DA019706 from NIH/NIDA; by grant #M01 RR03186 from the General Clinical Research Centers Program of the National Center for Research Resources, NIH; by grant 1UL1RR025011 from the Clinical and Translational Science Award (CTSA) program of the National Center for Research Resources, NIH; and by grant #1K05CA139871 from NIH. Medication was provided to participants at no cost under a research agreement with GlaxoSmithKline (GSK); no part of this manuscript was written or edited by anyone employed by GSK. The authors are solely responsible for the analyses, content, and writing of this article. The authors have full control of all primary data, and they agree to allow the journal to review the data if requested.
We declare that this research complies with the current laws of the USA. All participants gave written informed consent, and the study was approved by the University of Wisconsin Health Sciences Institutional Review Board.
We would like to thank the staff at the Center for Tobacco Research and Intervention in the University of Wisconsin School of Medicine and Public Health for their help with this research. We are particularly grateful to Linda Kurowski, Christine Ripley, and Wendy Theobald for their assistance.
Author information
Authors and Affiliations
Corresponding author
Additional information
S. J. Japuntich is now at the Tobacco Research and Treatment Center and Mongan Institute for Health Policy, Massachusetts General Hospital, Harvard Medical School.
Rights and permissions
About this article
Cite this article
Schlam, T.R., Japuntich, S.J., Piper, M.E. et al. Cognitive conflict following appetitive versus negative cues and smoking cessation failure. Psychopharmacology 214, 603–616 (2011). https://doi.org/10.1007/s00213-010-2063-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00213-010-2063-9