Abstract
Summary
Whether infant vitamin D supplementation may have long-term bone benefits is unclear. In this study, breastfed infants who received vitamin dosages greater than 400 IU/day did not have higher bone mineralization at 3 years. This study provides important data to inform pediatric public health recommendations for vitamin D.
Introduction
North American health agencies recommend breastfed infants should be supplemented with 400 IU of vitamin D/day to support bone health. Few studies examined the long-term benefits of early life vitamin D supplementation on bone mineralization. The objective of this study was to determine if a dose-response relationship exists between infant vitamin D supplementation, vitamin D status, and bone outcomes at 3 years of age.
Methods
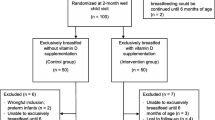
This was a double-blind randomized trial of 132, 1-month-old healthy, breastfed infants from Montréal, Canada, between 2007 and 2010. In this longitudinal analysis, 87 infants (66 %) returned for follow-up at 3 years of age, between 2010 and 2013. At 1 month of age, participants were randomly assigned to receive oral cholecalciferol (vitamin D3) supplements of 400, 800, 1200, or 1600 IU/day until 12 months of age. Lumbar spine vertebrae 1–4 (LS) bone mineral density (BMD), LS and whole body bone mineral content (BMC), and mineral accretion were measured by dual-energy x-ray absorptiometry at 3 years.
Results
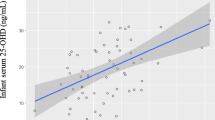
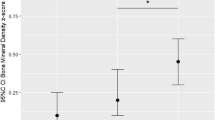
At follow-up, the treatment groups were similar in terms of diet, sun exposure, and demographics. There were no significant differences among the groups in LS or whole body BMC, BMD, or accretion. Although, 25(OH)D concentrations were not different among the groups, higher doses (1200 and 1600 IU/day) achieved higher 25(OH)D area under the curve from 1 to 36 months vs. 400 IU/day.
Conclusions
This is the first longitudinal follow-up of an infant vitamin D dose-response study which examines bone mineralization at 3 years of age. Dosages higher than 400 IU/day do not appear to provide additional benefits to the bone at follow-up. Larger studies with more ethnically diverse groups are needed to confirm these results.

Similar content being viewed by others
References
Institute of Medicine (2011) Dietary reference intakes for calcium and vitamin D. National Academy Press, Washington, DC
Leidig-Bruckner G, Roth HJ, Bruckner T et al (2011) Are commonly recommended dosages for vitamin D supplementation too low? Vitamin D status and effects of supplementation on serum 25-hydroxyvitamin D levels—an observational study during clinical practice conditions. Osteoporos Int 22:231–240. doi:10.1007/s00198-010-1214-5
Wagner CL, Greer FR, American Academy of Pediatrics Section on Breastfeeding, American Academy of Pediatrics Committee on Nutrition (2008) Prevention of rickets and vitamin D deficiency in infants, children, and adolescents. Pediatrics 122:1142–1152. doi:10.1542/peds.2008-1862
Godel JC, Canadian Paediatric Society, First Nations, Inuit and Métis Health Committe (2007) Vitamin D supplementation: recommendations for Canadian mothers and infants. Paediatr Child Health 12:583–598
Gallo S, Comeau K, Vanstone C et al (2013) Effect of different dosages of oral vitamin D supplementation on vitamin D status in healthy, breastfed infants: a randomized trial. JAMA J Am Med Assoc 309:1785–1792. doi:10.1001/jama.2013.3404
Holmlund-Suila E, Viljakainen H, Hytinantti T et al (2012) High-dose vitamin D intervention in infants—effects on vitamin d status, calcium homeostasis, and bone strength. J Clin Endocrinol Metab 97:4139–4147. doi:10.1210/jc.2012-1575
Ziegler EE, Nelson SE, Jeter JM (2014) Vitamin D supplementation of breastfed infants: a randomized dose-response trial. Pediatr Res. doi:10.1038/pr.2014.76
Gallo S, Vanstone CA, Weiler HA (2012) Normative data for bone mass in healthy term infants from birth to 1 year of age. J Osteoporos 2012:672403. doi:10.1155/2012/672403
Cooper C, Javaid MK, Taylor P et al (2002) The fetal origins of osteoporotic fracture. Calcif Tissue Int 70:391–394. doi:10.1007/s00223-001-0044-z
Holroyd C, Harvey N, Dennison E, Cooper C (2012) Epigenetic influences in the developmental origins of osteoporosis. Osteoporos Int 23:401–410. doi:10.1007/s00198-011-1671-5
Mahon P, Harvey N, Crozier S et al (2010) Low maternal vitamin D status and fetal bone development: cohort study. J Bone Miner Res Off J Am Soc Bone Miner Res 25:14–19. doi:10.1359/jbmr.090701
Weiler H, Fitzpatrick-Wong S, Veitch R et al (2005) Vitamin D deficiency and whole-body and femur bone mass relative to weight in healthy newborns. CMAJ 172:757–761. doi:10.1503/cmaj.1040508
Viljakainen HT, Saarnio E, Hytinantti T et al (2010) Maternal vitamin D status determines bone variables in the newborn. J Clin Endocrinol Metab 95:1749–1757. doi:10.1210/jc.2009-1391
Javaid MK, Crozier SR, Harvey NC et al (2006) Maternal vitamin D status during pregnancy and childhood bone mass at age 9 years: a longitudinal study. Lancet 367:36–43. doi:10.1016/S0140-6736(06)67922-1
Greer FR, Searcy JE, Levin RS et al (1982) Bone mineral content and serum 25-hydroxyvitamin D concentrations in breast-fed infants with and without supplemental vitamin D: one-year follow-up. J Pediatr 100:919–922
Roberts CC, Chan GM, Folland D et al (1981) Adequate bone mineralization in breast-fed infants. J Pediatr 99:192–196
Zamora SA, Rizzoli R, Belli DC et al (1999) Vitamin D supplementation during infancy is associated with higher bone mineral mass in prepubertal girls. J Clin Endocrinol Metab 84:4541–4544. doi:10.1210/jcem.84.12.6183
Cheng S, Tylavsky F, Kröger H et al (2003) Association of low 25-hydroxyvitamin D concentrations with elevated parathyroid hormone concentrations and low cortical bone density in early pubertal and prepubertal Finnish girls. Am J Clin Nutr 78:485–492
Hazell TJ, Pham TT, Jean-Philippe S et al (2014) Vitamin D status is associated with bone mineral density and bone mineral content in preschool-aged children. J Clin Densitom Off J Int Soc Clin Densitom. doi:10.1016/j.jocd.2014.04.121
Cooper C, Cawley M, Bhalla A et al (1995) Childhood growth, physical activity, and peak bone mass in women. J Bone Miner Res Off J Am Soc Bone Miner Res 10:940–947. doi:10.1002/jbmr.5650100615
De Onis M, Onyango AW, Borghi E et al (2007) Development of a WHO growth reference for school-aged children and adolescents. Bull World Health Organ 85:660–667
Gallo S, Comeau K, Agellon S et al (2014) Methodological issues in assessing plasma 25-hydroxyvitamin D concentration in newborn infants. Bone 61:186–190. doi:10.1016/j.bone.2014.01.012
Singh RJ (2010) Quantitation of 25-OH-vitamin D (25OHD) using liquid tandem mass spectrometry (LC-MS-MS). Methods Mol Biol 603:509–517. doi:10.1007/978-1-60761-459-3_50
Thomas JB, Duewer DL, Mugenya IO et al (2012) Preparation and value assignment of standard reference material 968e fat-soluble vitamins, carotenoids, and cholesterol in human serum. Anal Bioanal Chem 402:749–762. doi:10.1007/s00216-011-5447-8
Holick MF, Binkley NC, Bischoff-Ferrari HA et al (2011) Evaluation, treatment, and prevention of vitamin D deficiency: an Endocrine Society clinical practice guideline. J Clin Endocrinol Metab 96:1911–1930. doi:10.1210/jc.2011-0385
El Hayek J, Pham TT, Finch S et al (2014) Validity and reproducibility of a short food frequency questionnaire in assessing calcium and vitamin D intake in Canadian preschoolers. EC Nutr 1(1):9–18
Food and Drug Regulations. CRC, c 870 (last amended on 2014 Aug. 21). http://laws-lois.justice.gc.ca/eng/regulations/C.R.C.,_c._870/. Accessed 25 Sep 2014
El Hayek J, Pham TT, Finch S et al (2013) Vitamin D status in Montréal preschoolers is satisfactory despite low vitamin D intake. J Nutr 143:154–160. doi:10.3945/jn.112.169144
Barger-Lux MJ, Heaney RP (2002) Effects of above average summer sun exposure on serum 25-hydroxyvitamin D and calcium absorption. J Clin Endocrinol Metab 87:4952–4956. doi:10.1210/jc.2002-020636
Webb AR, Kline L, Holick MF (1988) Influence of season and latitude on the cutaneous synthesis of vitamin D3: exposure to winter sunlight in Boston and Edmonton will not promote vitamin D3 synthesis in human skin. J Clin Endocrinol Metab 67:373–378. doi:10.1210/jcem-67-2-373
Del Bino S, Sok J, Bessac E, Bernerd F (2006) Relationship between skin response to ultraviolet exposure and skin color type. Pigment Cell Res 19:606–614. doi:10.1111/j.1600-0749.2006.00338.x
Kalkwarf HJ, Abrams SA, DiMeglio LA et al (2014) Bone densitometry in infants and young children: the 2013 ISCD Pediatric Official Positions. J Clin Densitom 17:243–257. doi:10.1016/j.jocd.2014.01.002
Kelly T, Specker B, Binkley T, et al. (2006) Pediatric BMD reference database for US white children. BONE, p Suppl1:S30
Institute of Medicine (2005) Dietary reference intakes for energy, carbohydrate, fiber, fat, fatty acids, cholesterol, protein, and amino acids (macronutrients). National Academy Press, Washington, DC
Winzenberg T, Powell S, Shaw KA, Jones G (2011) Effects of vitamin D supplementation on bone density in healthy children: systematic review and meta-analysis. BMJ 342:c7254
Ma J, Siminoski K, Alos N et al (2015) The choice of normative pediatric reference database changes spine bone mineral density Z-scores but not the relationship between bone mineral density and prevalent vertebral fractures. J Clin Endocrinol Metab 100:1018–1027. doi:10.1210/jc.2014-3096
Leonard MB, Propert KJ, Zemel BS et al (1999) Discrepancies in pediatric bone mineral density reference data: potential for misdiagnosis of osteopenia. J Pediatr 135:182–188
Noon E, Singh S, Cuzick J et al (2010) Significant differences in UK and US female bone density reference ranges. Osteoporos Int 21:1871–1880. doi:10.1007/s00198-009-1153-1
Singh RJ, Taylor RL, Reddy GS, Grebe SKG (2006) C-3 epimers can account for a significant proportion of total circulating 25-hydroxyvitamin D in infants, complicating accurate measurement and interpretation of vitamin D status. J Clin Endocrinol Metab 91:3055–3061. doi:10.1210/jc.2006-0710
Kamao M, Tatematsu S, Hatakeyama S et al (2004) C-3 epimerization of vitamin D3 metabolites and further metabolism of C-3 epimers: 25-hydroxyvitamin D3 is metabolized to 3-epi-25-hydroxyvitamin D3 and subsequently metabolized through C-1alpha or C-24 hydroxylation. J Biol Chem 279:15897–15907. doi:10.1074/jbc.M311473200
Zemel B, Bass S, Binkley T et al (2008) Peripheral quantitative computed tomography in children and adolescents: the 2007 ISCD Pediatric Official Positions. J Clin Densitom 11:59–74. doi:10.1016/j.jocd.2007.12.006
Wu T-C, Huang I-F, Chen Y-C et al (2011) Differences in serum biochemistry between breast-fed and formula-fed infants. J Chin Med Assoc 74:511–515. doi:10.1016/j.jcma.2011.09.007
Seibel M (2005) Biochemical markers of bone turnover part I: biochemistry and variability. Clin Biochem Rev 26:97–122
Acknowledgments
The authors would like to thank Dr. Ali Khamessan, PhD Europharm International Canada Inc., for the design of the study product. We thank McGill University graduate student Sade Hayes RD, MSc for the help with study measurements and analysis of the dietary data. Finally, we would like to thank all the families who agreed to participate in the original and current follow-up study and the Mary Emily Clinical Nutrition Research Unit of the School of Dietetics and Human Nutrition.
Research funding was provided by the Canadian Institutes of Health Research and Nutricia Research Foundation, Europharm International Canada Inc. provided in-kind support of supplements. The sponsors were not involved in the design, conduct of the study, collection, management, analysis, and interpretation of the data; or in the preparation, review, or approval of the manuscript. Dr. Hope A. Weiler, RD PhD is a Canada Research Chair with infrastructure funding from the Canadian Foundation for Innovation. Drs. Sina Gallo and Hope Weiler had full access to all the data in the study and take responsibility for the integrity of the data and the accuracy of the data analysis.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
McGill University and George Mason University institutional review boards provided ethical approval for the study.
Conflicts of interest
Sina Gallo, Tom Hazell, Catherine A. Vanstone, Sherry Agellon, Glenville Jones, Mary L’Abbé, and Celia Rodd declare that they have no conflict of interest. Hope Weiler is a Canada Research Chair with infrastructure funding from the Canadian Foundation for Innovation.
Sources of support
Canadian Institutes of Health Research and the Nutricia Research Foundation for research funding, and Europharm International Canada Inc. for the in-kind support of supplements.
Additional information
Trial registration clinical trials.gov Identifier NCT00381914
Electronic supplementary material
Below is the link to the electronic supplementary material.
ESM 1
(DOC 83 kb)
Rights and permissions
About this article
Cite this article
Gallo, S., Hazell, T., Vanstone, C.A. et al. Vitamin D supplementation in breastfed infants from Montréal, Canada: 25-hydroxyvitamin D and bone health effects from a follow-up study at 3 years of age. Osteoporos Int 27, 2459–2466 (2016). https://doi.org/10.1007/s00198-016-3549-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00198-016-3549-z