Abstract
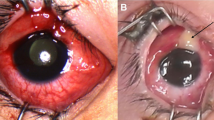
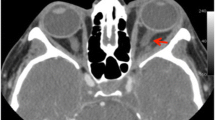
A case of orbital cellulitis caused by mucormycosis developed in a patient subsequent to cataract extraction and during systemic steroid treatment for postoperative complications. Fatal mucormycosis is a rare disease usually beginning with a subcutaneous inflammatory lesion. As the subsequent development of orbital cellulitis is very rare, little has been published on this subject. In cases of subcutaneous mucormycosis, the diagnosis can easily be made by means of histologic examination of the lesion. However, early diagnosis is difficult in cases with orbital involvement, because the most common cause of orbital cellulitis is bacterial. Thus, orbital cellulitis caused by mucormycosis is often wrongly treated with antibacterial agents only, as histologic examination is neither easy nor part of any routine investigation. Therefore, a combined treatment using antibiotics and antifungal agents in immunusuppressed patients with this disease is advocated.
Similar content being viewed by others
References
Agger W, Maki D (1978) Mucormycosis: a complication of critical care. Arch Intern Med 138:927
Ainsworth G, Sparrow F, Sussman A (1973) The fungi. Academic Press, New York
Bauer H, Wallace G, Sheldon W (1957) The effects of cortisone and chemical inflammation on experimental mucormycosis. Yale J Biol Med 29:389–395
Bruck H, Nash G, Foley F, Pruitt B Jr (1971) Opportunistic fungal infection of the burn wound with Phycomycetes andAspergillus: a clinical-pathogenic review. Arch Surg 102:476–482
Deal W, Johnson J (1969) Gastric phycomycosis: report of a case and review of the literature. Gastroenterology 57:579–586
DeSouza R, MacKinnon S, Spagnola S, Fossieck B Jr (1972) Treatment of localized pulmonary phycomycosis. South Med J 72:609–612
Haim S, Better O, Lichtig C, Erlik D, Barzilai A (1979) Rhinocerebral mucormycosis following kidney transplantation. Isr J Med Sci 6:646–649
Meyer R, Armstrong D (1973) Mucormycosis — changing status. Crit Rev Clin Lab Sci 4:421–451
Meyer R, Rosen P, Armstrong D (1972) Phycomycosis complicating leukemia and lymphoma. Ann Intern Med 77:871–879
Pillsburg H, Fischer N (1977) Rhinocerebral mucormycosis. Arch Otolaryngol 103:600–604
Rabin E, Lundberg G, Mitchell E (1961) Mucormycosis in severely burned patients: report of two cases with extensive destruction of the face and nasal cavity. N Engl J Med 264: 1286–1289
Stevens K, Newell R, Bergstrom L (1972) Mucormycosis in a patient receiving azahtioprine. Arch Otolaryngol 96:250–251
Stinson E, Bieber C, Griepp R, Clark D, Shumway N, Remington J (1971) Infectious complications after cardiac transplantation in man. Ann Intern Med 74:22–36
Straatsma B, Zimmerman L, Gass J (1962) Phycomycosis: a clinicopathologic study of fifty-one cases. Lab Invest 11:963–985
Taylor C, Alexander R, Green W, Kramer H Jr (1969) Mucormycosis (phycomycosis) involving the maxilla: report of a case with survival. Oral Surg 27:806–822
Watson K, Neame P (1960) In vitro activity of amphotericin B on strains of Mucoraceae pathogenic to man. J Lab Clin Med 56:251–257
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Kotzamanoglou, K., Tzanakakis, G., Michalopoulos, E. et al. Orbital cellulitis due to mucormycosis. Graefe's Arch Clin Exp Ophthalmol 226, 539–541 (1988). https://doi.org/10.1007/BF02169201
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF02169201