Abstract
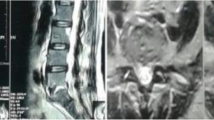
Lumbar disc infection, either after surgical discectomy or caused by haematogenous spread from other infection sources, is a severe complication. Specific antibiotic treatment has to be started as soon as possible to obtain satisfactory results in conservative treatment or operative fusion. The aim of this study was to analyse 16 cases of lumbar disc infection, treated with percutaneous lumbar discectomy (PLD) to obtain adequate amounts of tissue for histological examination and microbial culture. Between 1990 and 1994, 26 patients with vertebral osteomyelitis were treated. Sixteen patients, with an average age of 41.4 years (range 14–59 years), underwent a diagnostic PLD. Eight of them showed only moderate changes on computed tomograms (CT scans) and magnetic resonance (MR) images in the initial stages of the disease. The other eight showed more or less extensive osteolytic lesions of one or both vertebral bodies adjacent to the involved disc. The histology results showed non-specific discitis in nine patients and tuberculosis in one. In two patients an open biopsy had been performed, which showed non-specific discitis. Microbiological analysis revealed specific infection in 45% of the patients. These patients received a specific antibiotic treatment after antibiogram for an average of 33 days. Only three patients were treated surgically, with evacuation of the disc space and interbody fusion; the whole group received a spondylitis brace. All patients obtained satisfactory clinical results at the last follow-up regarding pain, mobility and spontaneous fusion of the involved disc space. In conclusion, PLD is a very helpful minimally invasive procedure in conservative treatment of lumbar discitis.
Similar content being viewed by others
References
Bircher MD, Tasker T, Crawshaw C, Mulholland RC (1988) Discitis following lumbar surgery. Spine 13:98–102
Collert S (1977) Osteomyelitis of the spine. Acta Orthop Scand 40:283–290
Digby JM, Kersley BJ (1979) Pyogenic nontuberculous spinal infection. J Bone Joint Surg Br 61:47
Dufek P, von Salis Soglio G, Bozdech Z (1987) Die unspezifische bakterielle Spondylitis - eine Analyse von 32 Fällen. Z Orthop Ihre Grenzgeb 125:255–261
Friedrich M, Kramer J (1990) Neue Aspekte in der Diagnostik der Spondylodiszitis. Z Orthop Ihre Grenzgeb 128:503–506
Hodgson AR, Stock FE (1960) Anterior spine fusion for the treatment of tuberculosis of the spine. J Bone Joint Surg Am 42:295
Krödel A, Stürz H (1989) Differenzierte operative und konservative Therapie der Spondylitis und Spondylodiszitis. Z Orthop Ihre Grenzgeb 127:587–596
Meurer A, Eysel P, Heine J (1995) Ergebnisse der operatives Behandlung der Spondylitis tuberculosa. Z Orthop Ihre Grenzgeb 133:227–335
Otten R, Ludwig C, Rütt J (1992) Die spezifische und unspezifische Spondylitis — eigene Nachuntersuchungsergebnisse. Orthop Praxis 28: 113–115
Peters KM, Schwanitz B, Zilkens KW (1992) Spondylodiszitis - eine häufig spät gestellte Diagnose. Orthop Praxis 28:108–112
Postacchini F, Cinotti G (1993) Postoperative lumbar discitis. Eur Spine J 1:226–230
Thibodeau AA (1968) Closed space infection following removal of lumbar intervertebral disc. J Bone Joint Surg Am 50:400–410
Valls J, Ottolenghi CE, Schajowicz F (1984) Aspiration biopsy in diagnosis of lesions of vertebral bodies. JAMA 136:375–382
Yu WY, Siu C, Wing PC, Schweigel JF, Jetha N (1991) Percutaneous suction aspiration for osteomyelitis. Spine 16:198–202
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Haaker, R.G., Senkal, M., Kielich, T. et al. Percutaneous lumbar discectomy in the treatment of lumbar discitis. Eur Spine J 6, 98–101 (1997). https://doi.org/10.1007/BF01358740
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF01358740