Summary
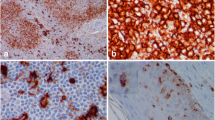
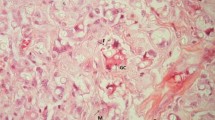
Immunocompetent antigen-presenting Langerhans cells were investigated in skin biopsies of 20 short-term Type 1 (insulin-dependent) diabetic patients and compared with 17 matched normal control subjects. Langerhans cells in epidermal sheet preparations were visualized with a monoclonal anti-HLA DR antibody using indirect immunofluorescence. A significant decrease of Langerhans cells/mm2 body surface area was found in 10 patients immediately at the onset of diabetes compared to 10 patients with 6 months duration of diabetes and to normal control subjects (401±30 vs 559±43 vs 611±33, p<0.01 and p<0.002). There was no significant difference in the number of Langerhans cells between patients with 6 months duration of diabetes and control subjects. Examination of the most likely precursor of Langerhans cells, the blood monocytes, indicated an increase of monocyte counts in Type 1 diabetic patients after 6 months duration (344±37 cells/μl vs 191±31 in control subjects, p<0.05) and an inverse correlation between the number of Langerhans cells in skin with the number of monocytes in peripheral blood (at onset: r=−0.73, p<0.01, after 6 months of diabetes: r=−0.61, p<0.05). In addition, a positive correlation between Langerhans cells and daily insulin dose was noted in patients after 6 months of diabetes (r=0.76, p<0.01). The data suggest a loss of Langerhans cells in skin at the onset of Type 1 diabetes and that functional alterations of these and perhaps also other antigenpresenting cells may be involved in the pathogenesis of Type 1 diabetes.
Article PDF
Similar content being viewed by others
References
Ziegler AG, Standl E, Lander T, Nerl C, Rieber EP, Mehnert H (1987) Cell mediated autoimmunity at the onset of insulin-dependent diabetes mellitus (IDDM). Klin Wochenschr 65: 546–550
Stingl G, Romani N, Wolff K (1987) Langerhans cells: a distinctive member of bone marrow-derived dendritic cells. Adv Dermatol 2: 269–282
Sontheimer RD, Bergstresser PR (1982) Epidermal Langerhans cell involvement in cutaneous lupus erythematosus. J Invest Dermatol 79: 237–243
Andrews BS, Frion GJ, Barr RJ, Minck GR, Bergman M, Sandborg C, Ross PA (1986) Loss of epidermal Langerhans cells and endothelial cell HLA-DR antigens in the skin in progressive systemic sclerosis. J Rheumatol 13: 341–348
Aberer W, Schuler G, Stingl G, Hönigsmann H, Wolff K (1981) Ultraviolet light depletes surface markers of Langerhans cells. J Invest Dermatol 76: 202–210
Belsito DV, Flotte TY, Lim HW, Baer RL, Thorbecke GT, Gigli I (1982), Effect of glucocorticosteroids on epidermal Langerhans cells. J Exp Med 155: 291–302
Juhlin L, Shelly WB (1977) New staining techniques for the Langerhans cells. Acta Derm Venereol (Stockh) 57: 289–295
Nordlund JJ, Ackles A (1981) A method for quantifying Langerhans cells in epidermal sheets of human and murine skin. Tissue Antigens 17: 217–222
Silberberg-Sinakin I, Thorbecke GJ, Baer RL, Rosenthal SA, Berezowsky V (1976) Antigen bearing Langerhans cells in skin, dermal lymphatics and in lymph nodes. Cell Immunol 25: 137–151
Shah SC, Malone JI, Simpson NE (1988) A comparison of high dose insulin therapy and steroid — immuran therapy in new onset insulin-dependent diabetics. Diabetes 37 [Suppl.1]: 203 A
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Ziegler, A.G., Standl, E. Loss of Ia-positive epidermal Langerhans cells at the onset of Type 1 (insulin-dependent) diabetes mellitus. Diabetologia 31, 632–635 (1988). https://doi.org/10.1007/BF00264773
Received:
Issue Date:
DOI: https://doi.org/10.1007/BF00264773