Abstract
Purpose
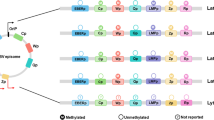
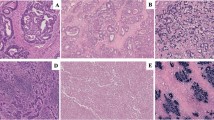
Hodgkin lymphoma (HL) is characterized by the presence of Hodgkin and Reed-Sternberg cells. Epstein-Barr virus (EBV) infection is thought to play an important role in the development of HL. Although epigenetic alterations, such as aberrant DNA methylation, are known to contribute to the pathogenesis of various malignancies, little is known about such alterations in HL and their putative relationships with EBV infection.
Methods
We investigated promoter methylation patterns of seven tumor-associated genes in 53 primary HL cases using methylation-specific PCR (MS-PCR). Concomitantly, the EBV infection status was assessed using PCR, in situ hybridization and immunohistochemistry.
Results
The gene promoter hypermethylation frequencies observed were 77.3 % for P16, 58.5 % for RASSF1A, 50.9 % for CDH1, 45.3 % for DAPK, 43.4 % for GSTP1, 37.7 % for SHP1 and 24.3 % for MGMT. SHP1 gene promoter hypermethylation was more frequently observed in patients at extreme ages (i.e., ≤ 15 and >54 years) than in adult patients (p = 0.006) and in patients with B symptoms (p = 0.03). Interestingly, most of the analyzed gene promoters were more frequently hypermethylated in EBV-negative than in EBV-positive cases, in particular the DAPK gene promoter (58 % versus 27 %, p = 0.04). Furthermore, hypermethylation of multiple gene promoters (≥ 3) was encountered more frequently in females than in males (86 % versus 57 %, p = 0.04), whereas EBV-positive cases were more common among males than females (55 % versus 30 %, p = 0.02).
Conclusions
Our results indicate that epigenetic changes frequently occur in both EBV-positive and EBV-negative HL. The rates of these changes were found to vary according to clinico-pathological parameters. These observations probably reflect the multitude of factors involved in HL development and the complexity of their interactions with genetic and/or hormonal factors.




Similar content being viewed by others
References
H. Kanzler, R. Kuppers, M.L. Hansmann, K. Rajewsky, Hodgkin and reed-Sternberg cells in Hodgkin’s disease represent the outgrowth of a dominant tumor clone derived from (crippled) germinal center B cells. J. Exp. Med. 184, 1495–1505 (1996)
T. Marafioti, M. Hummel, H.D. Foss, H. Laumen, P. Korbjuhn, I. Anagnostopoulos, H. Lammert, G. Demel, J. Theil, T. Wirth, H. Stein, Hodgkin and reed–Sternberg cells represent an expansion of a single clone originating from a germinal center B-cell with functional immunoglobulin gene rearrangements but defective immunoglobulin transcription. Blood 95, 1443–1450 (2000)
R. Kuppers, identifying the precursors of Hodgkin and Reed-Sternberg cells in Hodgkin’s disease: role of the germinal center in B-cell lymphomagenesis. J. Acquir. Immune. Defic. Syndr. 21, 74–79 (1999)
E.S. Jaffe, N.L. Harris, H. Stein, J.W. Vardiman, (eds) World Health Organization Classification of Tumours.Pathologyand Genetics of Tumours of the Haematopoietic and Lymphoid Tissues. (IARC Press, Lyon, 2001) pp 237–251
P.A. McKinney, F.E. Alexander, T.J. Rickett, J. Williams, R.A. Cartwright, A specialist leukaemia/lymphoma registry in the UK. Part 1: incidence and geographical distribution of Hodgkin’s disease. Leukaemia research fund data collection study group. Br. J. Cancer 60, 942–947 (1989)
S.L. Glasser, W.G. Swartz, Time trends in Hodgkin’s disease incidence. Role Diagn. Accuracy. Cancer. 66, 2196–2204 (1990)
S.L. Glaser, R.J. Lin, S.L. Stewart, R.F. Ambinder, R.F. Jarrett, P. Brousset, G. Pallesen, M.L. Gulley, G. Khan, J. O'Grady, M. Hummel, M.V. Preciado, H. Knecht, J.K. Chan, A. Claviez, Epstein-Barr virus-associated Hodgkin's disease: epidemiologic characteristics in international data. Int. J. Cancer 70, 375–382 (1997)
P.G. Murray, L.S. Young, M. Rowe, J. Crocker, Immunohistochemical demonstration of the Epstein-Barr virus-encoded latent membrane protein in paraffin sections of Hodgkin's disease. J. Pathol. 166, 1–5 (1992)
P. Brousset, D. Schlaifer, F. Meggetto, E. Bachmann, S. Rothenberger, J. Pris, G. Delsol, H. Knecht, Persistence of the same viral strain in early and late relapses of Epstein-Barr virus-associated Hodgkin’s disease. Blood 84, 2447–2451 (1994)
E. Yiannakopoulou, Targeting epigenetic mechanisms and microRNAs by aspirin and other non steroidal anti-inflammatory agents–implications for cancer treatment and chemoprevention. Cell. Oncol. 37, 167–178 (2014)
J.S. de Groot, X. Pan, J. Meeldijk, E. van der Wall, P.J. van Diest, C.B. Moelans, Validation of DNA promoter hypermethylation biomarkers in breast cancer–a short report. Cell. Oncol. 37, 297–303 (2014)
R. Singal, G.D. Ginder, DNA methylation. Blood 93, 4059–4070 (1999)
S.B. Baylin, Tying it all together: epigenetics, genetics, cell cycle, and cancer. Science 277, 1948–1949 (1997)
S.B. Baylin, J.G. Herman, DNA hypermethylation in tumorigenesis: epigenetics joins genetics. Trends Genet. 16, 168–174 (2000)
J.G. Herman, S.B. Baylin, Gene silencing in cancer in association with promoter hypermethylation. N. Engl. J. Med. 349, 2042–2054 (2003)
M. Esteller, Relevance of DNA methylation in the management of cancer. Lancet Oncol. 4, 351–358 (2003)
A. Rawat G. AGopisetty, R. Thangarajan, E4BP4 is a repressor of epigenetically regulated SOSTDC1 expression in breast cancer cells. Cell. Oncol. 37, 409–419 (2014)
A. Yousuf, M.Y. Bhat, A.A. Pandith, D. Afroze, N.P. Khan, K. Alam, P. Shah, M.A. Shah, S. Mudassar, MGMT gene silencing by promoter hypermethylation in gastric cancer in a high incidence area. Cell. Oncol. 37, 245–252 (2014)
F.A. Duijkers, R.X. de Menezes, I.J. Goossens-Beumer, D.J. Stumpel, P. Admiraal, R. Pieters, J.P. Meijerink, M.M. van Noesel, Epigenetic drug combination induces genome-wide demethylation and altered gene expression in neuro-ectodermal tumor-derived cell lines. Cell. Oncol. 36, 351–362 (2013)
O. Ammerpohl, A. Haake, S. Pellissery, M. Giefing, J. Richter, B. Balint, M. Kulis, J. Le, M. Bibikova, H.G. Drexler, M. Seifert, R. Shaknovic, B. Korn, R. Küppers, J.I. Martín-Subero, R, array based DNA methylation analysis in classical Hodgkin lymphoma reveals new insights into the mechanisms underlying silencing of B cell-specific genes. Leukemia 26, 185–188 (2012)
A. Ushmorov, O. Ritz, M. Hummel, F. Leithäuser, P. Möller, H. Stein, T. Wirth, Epigenetic silencing of the immunoglobulin heavy chain gene in classical Hodgkin lymphoma -derived cell lines contributes to the loss ofimmunoglobulin expression. Blood 104, 3326–3334 (2004)
A. Ushmorov, F. Leithäuser, O. Sakk, Epigenetic processes play a major role in B-cell-specific gene silencing in classical Hodgkin lymphoma. Blood 107, 2493–2500 (2006)
J.G. Herman, J.R. Graff, S. Myohanen, B.D. Nelkin, S.B. Baylin, Methylation-specific PCR: a novel PCR assay for methylation status of CpG islands. Proc. Natl. Acad. Sci. U. S. A. 93, 9821–9826 (1996)
K. Amara, M. Trimeche, S. Ziadi, Presence of simian virus 40 DNA sequences in diffuse large B-cell lymphomas in Tunisia correlates with aberrant promoter hypermethylation of multiple tumor suppressor genes. Int. J. Cancer 121, 2693–2702 (2007)
R. Singal, L. Fredinand, I.M. Reis, J.J. Schlesselman, Methylation of multiple gene in prostate cancer and the relation with clinicopathological features and disease. Oncol. Rep. 12, 631–637 (2004)
D. Astuti, A. Agathanggelou, S. Honorio, et al., RASSF1A promoter region CpG island hypermethylation in phaeochromocytomas and neuroblastomatumours. Oncogene 20, 7573–7577 (2001)
M. Esteller, S. Tortola, M. Toyota, et al., Hypermethylation-associated inactivation of p14(ARF) is independent of p16(INK4a) methylation and p53 mutational status. Cancer Res. 60, 129–133 (2000)
R.A. Katzenellenbogen, S.B. Baylin, J.G. Herman, Hypermethylation of the DAP-kinase CpG island is a common alternation in B-cell malignancies. Blood 93, 4347–4353 (1999)
M. Esteller, P.G. Corn, J.M. Urena, E. Gabrielson, S.B. Baylin, J.G. Herman, Inactivation of glutathione S-transferase P1 gene by promoter hypermethylation in human neoplasia. Cancer Res. 58, 4515–4518 (1998)
T. Oka, M. Ouchida, M. Koyama, et al., Gene silencing of the tyrosine phosphatase SHP1 gene by aberrant methylation in leukemias/lymphomas. Cancer Res. 62, 6390–6394 (2002)
P.G. Corn, R.H. Heath, F. Fogt, A.A. Forastiere, J.G. Herman, T. Wu, Frequent hypermethylationof the 50 CpG island of E-cadherin in esophageal adenocarcinomas. Clin. Cancer Res. 7, 2765–2769 (2001)
M. Esteller, S.R. Hamilton, P.C. Burger, S.B. Baylin, J.G. Herman, Inactivation of the DNA repair gene O6-methylguanine-DNA methyltransferase by promoter hypermethylation is a common event in primary human neoplasia. Cancer Res. 59, 793–797 (1999)
M.R. Gopal, B.J. Thomson, J. Fox, R.S. Tedder, R.W. Honess, Detection by pcr of HHV-6 and EBV DNA in blood and oropharynx of healthy adults and hiv-seropositives. Lancet 335, 1598–1599 (1990)
M.G. Goll, T.H. Bestor, Eukaryotic cytosine methyltransferases. Annu. Rev. Biochem. 74, 481–514 (2005)
M. Esteller, Epigenetics in cancer. N. Engl. J. Med. 358, 1148–1159 (2008)
R.F. Jarrett, J. MacKenzie, Epstein-Barr Virus and other candidate viruses in the pathogenesis of Hodgkin’s disease. Semin. Hematol. 36, 260–269 (1999)
A.A. Armstrong, F.E. Alexander, R. Cartwright, et al., Epstein-Barr virus and Hodgkin's disease: further evidence for the three disease hypothesis. Leukemia 12, 1272–1276 (1998)
K.R. Kim, T. Yoshizaki, H. Miyamori, et al., Transformation of madin-darby canine kidney (MDCK) epithelial cells by Epstein-Barr virus latent membrane protein 1 (LMP1) induces expression of Ets1 and invasive growth. Oncogene 19, 1764–1771 (2000)
W.E. Miller, G. Mosialos, E. Kieff, N. Raab-Traub, Epstein-Barr virus LMP1 induction of the epidermal growth factor receptor is mediated through a TRAF signaling pathway distinct from NF-kappa B activation. J. Virol. 71, 586–594 (1997)
C.L. Tsai, H.P. Li, Y.J. Lu, et al., Activation of DNA methyltransferase1 by EBV LMP1 involves c-Jun NH(2)-terminal kinase signaling. Cancer Res. 66, 11668–11676 (2006)
F. Ksiaa, S. Ziadi, K. Amara, S. Korbi, M. Trimeche, Biological significance of promoter hypermethylation of tumor-related genes in patients with gastric carcinoma. Clin. Chim. Acta 404, 128–133 (2009)
M. Saito, J. Nishikawa, T. Okada, et al., Role of DNA methylation in the development of Epstein–Barr virus-associated gastric carcinoma. J. Med. Virol. 85, 121–127 (2013)
M.J. García, B. Martínez-Delgado, A. Cebrian, A. Martínez, J. Benítez, C. Rivas, Different incidence and pattern of p15INK4b and p16INK4a promoter region hypermethylation in Hodgkin's and CD30-positive non-Hodgkin's lymphomas. Am J Pathol. 161, 1007–1013 (2002)
K. Amara, M. Trimeche, S. Ziadi, A. Laatiri, M. Hachana, S. Korbi, Prognostic significance of aberrant promoter hypermethylation of CpG islands in patients with diffuse large B-cell lymphomas. Ann. Oncol. 19, 1774–&è86 (2008)
S. Challouf, S. Ziadi, R. Zaghdoudi, F. Ksiaa, R. Ben Gacem, M. Trimeche, Patterns of aberrant DNA hypermethylation in nasopharyngeal carcinoma in Tunisian patients. Clin. Chim. Acta 413, 795–802 (2012)
P.G. Murray, G.H. Qiu, L. Fu, et al., Frequentepigeneticinactivationof the RASSF1Atumor suppressor gene inHodgkin's lymphoma. Oncogene 23, 1326–1331 (2004)
C. Wu, M. Sun, L. Liu, G.W. Zhou, The function of the protein tyrosine phosphatase SHP-1 in cancer. Gene 13, 1–12 (2003)
S. Takeuchi, M. Matsushita, M. Zimmermann, et al., Clinical significance of aberrant DNA methylation in childhood acute lymphoblastic leukemia. Leuk. Res. 35, 1345–1349 (2011)
R.F. Jarrett, Viruses and Hodgkin's lymphoma. Ann. Oncol. 1, 23–29 (2002)
A.A. Armstrong, L. Shield, A. Gallagher, R.F. Jarrett, Lack of involvement of known oncogenic DNA viruses in Epstein-Barr virus-negative Hodgkin's disease. Br. J. Cancer 77, 1045–1047 (1998)
P. Brousset, V. de Araujo, R.D. Gascoyne, Immunohistochemical investigation of SV40largeTantigen in Hodgkin and non-Hodgkin's lymphoma. Int. J. Cancer 112, 533–535 (2004)
J. Hernández-Losa, C.G. Fedele, F. Pozo, A. Tenorio, V. Fernández, J. Castellví, C. Parada, S.A. Ramón y Cajal, Lack of association of polyomavirus and herpesvirus types 6 and 7in human lymphomas. Cancer. 103, 293–298 (2005)
A. Gallagher, J. Perry, L. Shield, J. Freeland, J. MacKenzie, R.F. Jarrett, Viruses and Hodgkin’s disease: no evidence of novel herpesviruses in non-EBV-associated lesions. Int. J. Cancer 101, 259–264 (2002)
O. Cohen, A. Kimchi, DAP-kinase:from functional gene cloning to establishment of its role in apoptosis and cancer. Cell Death Differ. 8, 6–15 (2001)
Acknowledgments
This work was supported by the ‘Ministère de l’Enseignement Supérieur, de la Recherche Scientifique et de la Technologie’ and the ‘Ministère de la Sante’ of Tunisia.
The authors thank Intissar Klibi-Toumi, Samir Jaafar, and Houda Sghaier for their technical assistance.
Conflict of interest
The authors declare no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Dhiab, M.B., Ziadi, S., Mestiri, S. et al. DNA methylation patterns in EBV-positive and EBV-negative Hodgkin lymphomas. Cell Oncol. 38, 453–462 (2015). https://doi.org/10.1007/s13402-015-0242-8
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13402-015-0242-8