Abstract
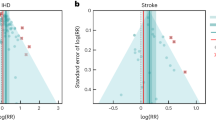
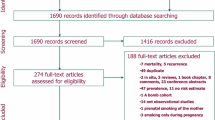
Epidemiological evidence suggests that passive smoke exposure is related to the development of diabetes. However, data on this issue are controversial. We conducted a meta-analysis to provide a quantitative assessment of the association between passive smoking and the risk of diabetes. We searched the Medline and Embase databases up to October 2013 to identify prospective cohort studies related to passive smoke exposure and incident diabetes. Summary effect estimates with 95 % confidence intervals (CI) were derived using a fixed or random effects model, depending on the heterogeneity of the included studies. Six prospective studies that span three continents involving 154,406 participants (ages 18–74) with 7,116 new diabetes cases were included in the meta-analysis. On the basis of the Newcastle Ottawa Scale system, five studies were identified as relatively high-quality. In our primary analysis, compared to never smokers without passive smoke exposure, never smokers reporting passive smoke exposure was associated with increased risk of diabetes (pooled relative risk 1.21, 95 % CI 1.07–1.38). Such association persisted in the dose–response analysis. No indications of significant heterogeneity and publication bias were detected. Estimates of total effects were generally consistent in the sensitivity and subgroup analyses. Findings of the present meta-analysis suggest that passive smoke exposure is independently associated with the risk of diabetes. The conclusion may have a far-reaching significance for public health in countries of high smoking intensity and high incident diabetes.



Similar content being viewed by others
References
E. Schönherr, Beitrag zur statistik und klinik der lungentumoren. Zeitschrift für Krebsforschung 27, 436–450 (1928)
M. Öberg, M.S. Jaakkola, A. Woodward, A. Peruga, A. Prüss-Ustün, A worldwide burden of disease from exposure to second-hand smoke: a retrospective analysis of data from 192 countries. Lancet 377, 139–146 (2011)
C. Willi, P. Bodenmann, W.A. Ghali, P.D. Faris, J. Cornuz, Active smoking and the risk of type 2 diabetes: a systematic review and meta-analysis. JAMA 298, 2654–2664 (2007)
M. Lajous, L. Tondeur, G. Fagherazzi, B. de Lauzon-Guillain, M.C. Boutron-Ruaualt, F. Clavel-Chapelon, Childhood and adult secondhand smoke and type 2 diabetes in women. Diabetes Care 36(9), 2720–2725 (2013)
T.K. Houston, S.D. Person, M.J. Pletcher, K. Liu, C. Iribarren, C.I. Kiefe, Active and passive smoking and development of glucose intolerance among young adults in a prospective cohort: CARDIA study. BMJ 332, 1064–1069 (2006)
A.S. Hosler, S.G. Nayak, A.M. Radigan, Stressful events, smoking exposure and other maternal risk factors associated with gestational diabetes mellitus. Paediatr. Perinat. Epidemiol. 25, 566–574 (2011)
K. Mattsson, K. Kallen, M.P. Longnecker, A. Rignell-Hydbom, L. Rylander, Maternal smoking during pregnancy and daughters’ risk of gestational diabetes and obesity. Diabetologia 56, 1689–1695 (2013)
D.F. Stroup, J.A. Berlin, S.C. Morton et al., Meta-analysis of observational studies in epidemiology: a proposal for reporting. Meta-analysis Of Observational Studies in Epidemiology (MOOSE) group. JAMA 283, 2008–2012 (2000)
G.A. Wells, B. Shea, D. O’Connell, J. Peterson, V. Welch, M. Losos, P. Tugwell. The Newcastle–Ottawa Scale (NOS) for assessing the quality of non-randomised studies in meta-analyses (2004). http://www.ohri.ca/programs/clinical_epidemiology/oxford.htm. Accessed 29 Apr 2004
J.P. Higgins, S.G. Thompson, Quantifying heterogeneity in a meta-analysis. Stat. Med. 21, 1539–1558 (2002)
J.P. Higgins, S.G. Thompson, J.J. Deeks, D.G. Altman, Measuring inconsistency in meta-analyses. BMJ 327, 557–560 (2003)
R. DerSimonian, N. Laird, Meta-analysis in clinical trials. Control. Clin. Trials 7, 177–188 (1986)
B. Woolf, On estimating the relation between blood group and disease. Ann. Hum. Genet. 19, 251–253 (1955)
M. Egger, G. Davey Smith, M. Schneider, C. Minder, Bias in meta-analysis detected by a simple, graphical test. BMJ 315, 629–634 (1997)
C.B. Begg, M. Mazumdar, Operating characteristics of a rank correlation test for publication bias. Biometrics 50, 1088–1101 (1994)
K.P. Ko, H. Min, Y. Ahn et al., A prospective study investigating the association between environmental tobacco smoke exposure and the incidence of type 2 diabetes in never smokers. Ann. Epidemiol. 21, 42–47 (2011)
M. Lajous, L. Tondeur, G. Fagherazzi, B. de Lauzon-Guillain, M.C. Boutron-Ruaualt, F. Clavel-Chapelon, Childhood and adult secondhand smoke and type 2 diabetes in women. Diabetes Care 36, 2720–2725 (2013)
L. Zhang, G.C. Curhan, F.B. Hu, E.B. Rimm, J.P. Forman, Association between passive and active smoking and incident type 2 diabetes in women. Diabetes Care 34, 892–897 (2011)
Y. Hayashino, S. Fukuhara, T. Okamura et al., A prospective study of passive smoking and risk of diabetes in a cohort of workers: the High-Risk and Population Strategy for Occupational Health Promotion (HIPOP-OHP) study. Diabetes Care 31, 732–734 (2008)
B. Kowall, W. Rathmann, K. Strassburger et al., Association of passive and active smoking with incident type 2 diabetes mellitus in the elderly population: the KORA S4/F4 cohort study. Eur. J. Epidemiol. 25, 393–402 (2010)
The health consequences of smoking—50 years of progress: a report of the Surgeon General 2014. http://www.surgeongeneral.gov/library/reports/50-years-of-progress/index.html. Accessed 24 Dec 2013
A.B. Hill, The environment and disease: association or causation? Proc. R. Soc. Med. 58, 295–300 (1965)
M. Sorensen, Z.J. Andersen, R.B. Nordsborg et al., Long-term exposure to road traffic noise and incident diabetes: a cohort study. Environ. Health Perspect. 121, 217–222 (2013)
M.R. Law, J.K. Morris, N.J. Wald, Environmental tobacco smoke exposure and ischaemic heart disease: an evaluation of the evidence. BMJ 315, 973–980 (1997)
M. Weitzman, S. Cook, P. Auinger et al., Tobacco smoke exposure is associated with the metabolic syndrome in adolescents. Circulation 112, 862–869 (2005)
D.F. Yankelevitz, C.I. Henschke, R. Yip et al., Second-hand tobacco smoke in never smokers is a significant risk factor for coronary artery calcification. JACC Cardiovasc. Imaging 6, 651–657 (2013)
L.E. Wagenknecht, G.L. Burke, L.L. Perkins, N.J. Haley, G.D. Friedman, Misclassification of smoking status in the CARDIA study: a comparison of self-report with serum cotinine levels. Am. J. Public Health 82, 33–36 (1992)
P. Vineis, L. Airoldi, F. Veglia et al., Environmental tobacco smoke and risk of respiratory cancer and chronic obstructive pulmonary disease in former smokers and never smokers in the EPIC prospective study. BMJ 330, 277 (2005)
M.D. Eisner, P.P. Katz, E.H. Yelin, S.K. Hammond, P.D. Blanc, Measurement of environmental tobacco smoke exposure among adults with asthma. Environ. Health Perspect. 109, 809–814 (2001)
Acknowledgment
This work was supported by Grants from the National Natural Science Foundation of China (81270916, 81000317 and 81170766). The funders were not involved in study design, data collection, data analysis, manuscript preparation and/or publication decisions.
Conflict of interest
All of the authors have no relevant conflict of interests.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Sun, K., Liu, D., Wang, C. et al. Passive smoke exposure and risk of diabetes: a meta-analysis of prospective studies. Endocrine 47, 421–427 (2014). https://doi.org/10.1007/s12020-014-0194-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12020-014-0194-1