Abstract
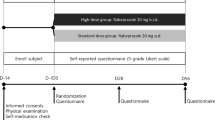
This study aimed to determine whether dysphagia associated with gastroesophageal reflux disease was effectively treated with rabeprazole, a proton pump inhibitor. Sixty-eight outpatients with gastroesophageal reflux-associated dysphagia were enrolled in this study. Endoscopic esophagitis was confirmed in 52 of 68 subjects. The proton pump inhibitor rabeprazole was administered at 20 mg daily for 8 weeks. Rabeprazole was administered for a further 6 months to 16 subjects whose dysphagia was improved (10 mg/day) and 5 of these underwent 24-hr esophageal pH monitoring before and after treatment. Dysphagia was completely resolved in 40 of 68 subjects, which were categorized in Group I. Dysphagia improved partially in 20 subjects and was unchanged in 8 subjects. These 28 subjects were categorized into Group II. Comparison was made between Group I and Group II and multivariate analysis demonstrated that the only factor that correlated with the effect of rabeprazole on dysphagia was “improvement in heartburn symptoms.” There were no relapses of symptoms during the 6-month follow-up period, and pH monitoring showed sustained suppression of acid secretion.The results indicate that rabeprazole is effective in the treatment of dysphagia associated with gastroesophageal reflux disease. We were, however, unable to elicit any factors that could predict the therapeutic effect of rabeprazole before commencing treatment.
Similar content being viewed by others
References
De Vault KR, Castell DO: The practice parameters committee of the American College of gastroenterology. Updated guidelines for the diagnosis and treatment of gastroesophageal reflux disease. Am J Gastroenterol 14:34–42, 1994
Armstrong D, Bennett JR, Blum AL, Dent J, DeDombal FT, Galmiche JP, Lundell L, Margulies M, Richter JE, Spechler SJ, Tytgat GN, Wallin L: The endoscopic assessment of esophagitis: a progress report on observer agreement. Gastroenterology 111:85–92, 1996
Lundell LR, Dent J, Bennett JR, Blum AL, Armstrong D, Galmiche JP, Johnson F, Hongo M, Richter JE, Spechler SJ, Tytgat GN, Wallin L: Endoscopic assessment of esophagitis: clinical and functional correlates and further validation of the Los Angeles Classification. Gut 45:172–180, 1999
Nguyen NQ, Holloway RH: Gastroesophageal reflux disease. Curr Opin Gastroenterol 19:373–378, 2003
Okamoto K, Iwakiri R, Mori M, Hara M, Oda K, Danjo A, Ootani A, Sakata H, Fujimoto K: Clinical symptoms in endoscopic esophagitis: evaluation in 8031 adult subjects. Dig Dis Sci 48:2237–2241, 2003
Tauber S, Gross M, Issing W: Association of laryngopharyngeal symptoms with gastroesophageal reflux disease. Laryngoscope 112:879–886, 2002
Woo P, Noodzij P, Ross J: Association of esophageal reflux and globus symptoms: comparison of laryngoscopy and 24-hour pH manometry. Otolaryngol Head Neck Surg 115:502–507, 1996
Shaker R, Milbrath M, Ren J, Toohill R, Hogan WJ, Li Q, Hofmann CL: Esophagopharyngeal distribution of refluxed gastric acid in patients with reflux laryngitis. Gastroenterology 109:1575–1582, 1995
Amin MR, Postma GN, Johnson P, Digges N, Koufman JA: Proton pump inhibitor resistance in the treatment of laryngopharyngeal reflux. Otolaryngol Head Neck Surg 125:374–378, 2001
Maton PN, Burton ME: Antacids revisited: a review of their clinical pharmacology and recommended therapeutic use. Drugs 57:855–870, 1999
Tytgat GN: Treatment of mild and severe cases of GERD. Aliment Pharmacol Ther 16 (Suppl 4):73–78, 2002
Pantoflickova D, Dorta G, Ravic M, Jornod P, Blum AL: Acid inhibition on the first day of dosing:comparison of four proton pump inhibitors. Aliment Pharmacol Ther 17:1507–1514, 2003
Saitoh T, Fukushima Y, Otsuka H, Hirakawa J, Mori H, Asano T, Ishikawa T, Katsube T, Ogawa K, Ohkawa S: Effect of rabeprazole, lansoprazole and omeprazole on intragastric p in CYP2C19 extensive metabolizers. Aliment Pharmacol Ther 16:1811–1817, 2002
Robinson M, Fitzgerald S, Hegedus R, Murthy A, Jokubaitis L: Onset of symptom relief with rabeprazole: a community-based, open-label assessment of patients with erosive oesophagitis. Aliment Pharmacol Ther 16:445–454, 2002
Holtmann G, Bytzer P, Metz M, Loeffler V, Blum AL: A randomized, double-blind, comparative study of standard-dose rabeprazole and high-dose omeprazole in gastro-oesophageal reflux disease. Aliment Pharmacol Ther 16:479–485, 2002
Adachi K, Hashimoto T, Hamamoto N, Hirakawa K, Niigaki M, Miyake T, Taniura H, Ono M, Kaji T, Suetsugu H, Yagi J, Komazawa Y, Mihara T, Katsube T, Fujishiro H, Shizuku T, Hattori S, Yamamoto S, Kinoshita Y: Symptom relief in patients with reflux esophagitis: Comparative study of omeprazole, lansoprazole, and rabeprazole. J Gastroenterol Hepatol 18:1392–1398, 2003
Ishizaki T, Horai Y: Cytochrome P450 and the metabolism of proton pump inhibitors—emphasis on rabeprazole. Aliment Pharmacol Ther 13 (Suppl 3):27–36, 1999
Adachi K, Katsube T, Kawamura A, Takashima T, Yuki M, Amano K, Ishihara S, Fukuda R, Watanabe M, Kinoshita Y: CYP2C19 genotype status and intragastric pH during dosing with lansoprazole or rabeprazole. Aliment Pharmacol Ther 14:1259–1266, 2000
Shirai N, Furuta T, Moriyama Y, Okochi H, Kobayashi K, Takashima M, Xiao F, Kosuge K, Nakawawa K, Hanai H, Chiba K, Ohashi K, Ishizaki T: Effects of CYP2C19 genotypic differences in the metabolism of omeprazole and rabeprazole on intragastric pH. Aliment Pharmacol Ther 15:1929–1937, 2001
Lachman L, Howden CW: Twenty-four-hour intragastric pH: Tolerance within 5 days of continuous ranitidine administration. Am J Gastroenterol 95:57–61, 2000
Fackler WK, Ours TM, Vaezi MF, Richter JE: Long-term effect of H2RA therapy on nocturnal gastric acid breakthrough. Gastroenterology 122:625–632, 2002
Adachi K, Komazawa Y, Fujishiro H, Mihara T, Ono M, Yuki M, Kawamura A, Karim RMA, Amano Y, Kinishita Y: Nocturnal gastric acid breakthrough during the administration of rabeprazole and ranitidine in Helicobacter pylori-negative subjects: effects of different regimens. J Gastroenterol 38:830–835, 2003
Thjodleifsson B, Rindi G, Fiocca R, Humphries TJ, Morcutti A, Miller N, Bardhan KD: A randomized, double-blind trial of the efficacy and safety of 10 or 20 mg rabeprazole compared with 20 mg omeprazole in the maintenance of gastro-oesophageal reflux disease over 5 years. Aliment Pharmacol Ther 17:343–351, 2003
Fass R, Fennerty MB, Johnson C, Camargo L, Samplimer RE: Correlation of ambulatory 24-hour esophageal pH monitoring results with symptom improvement in patients with noncardiac chest pain due to gastroesophageal reflux disease. J Clin Gastroenterol 28:36–39, 1999
Talley NJ, Fullerton S, Junghard O, Wiklund I: Quality of life in patients with endoscopy-negative heartburn: reliability and sensitivity of disease-specific instruments. Am J Gastroenterol 96:1998–2004, 2001
Young MA, Rose S, Reynolds JC: Gastrointestinal manifestations of scleroderma: Rheum Dis Clin North Am 22:797–823, 1996
Postma GN, Tomek MS, Belafsky PC, Koufman JA: Esophageal motor function in laryngopharyngeal reflux is superior to that in classic gastroesophageal reflux disease. Ann Otol Rhinol Laryngol 110:1114–1116, 2001
Yoshida N, Yoshikawa T, Tanaka Y, Fujita N, Kassai K, Naito Y, Kondo M: A new mechanism for anti-inflammatory actions of proton pump inhibitors—inhibitory effects on neutrophil–endothelial cell interactions. Aliment Pharmacol Ther 14 (Suppl 1):74–81, 2000
Hamaguchi M, Fujiwara Y, Takashima T, Hayakawa T, Sasaki E, Shiba M, Watanabe T, Tominaga K, Oshitani N, Matsumoto T, Higuchi K, Arawawa T: Increased expression of cytokines and adhesion molecules in rat chronic esophagitis. Digestion 68:189–197, 2003
Fujiwara Y, Higuchi K, Hamaguchi M, Takashima T, Watanabe T, Tominaga K, Oshitani N, Matsumoto T, Arakawa T: Increased expression of transforming growth factor-alpha and epidermal growth factor receptors in rat chronic reflux esophagitis. J Gastroenterol Hepatol 19:521–527, 2004
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Oda, K., Iwakiri, R., Hara, M. et al. Dysphagia Associated with Gastroesophageal Reflux Disease Is Improved by Proton Pump Inhibitor. Dig Dis Sci 50, 1921–1926 (2005). https://doi.org/10.1007/s10620-005-2962-5
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/s10620-005-2962-5