Abstract
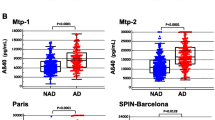
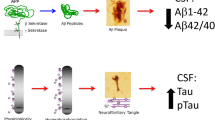
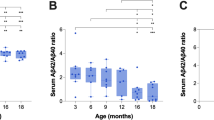
Experimental data suggest that the cerebrospinal fluid (CSF) dynamic is involved in the clearance of beta-amyloid, a key event in the pathogenesis of Alzheimer’s disease (AD). At this regard no evidence still exists in vivo. In this study we explored the relationships between CSF pressure and AD pathology, as measured with CSF core biomarkers. We enrolled 16 patients with probable AD and 21 controls, collecting demographics, clinical data, CSF opening pressure and CSF levels of beta-amyloid-42 fragment (Aβ42), total-tau (t-tau), phosphorylated-tau-181 (p-tau), albumin and albumin ratio. Differences between the groups were calculated with non-parametric tests, while correlations among all parameters were separately calculated with Spearman’s test in each group. The groups significantly differed in biomarkers’ concentration with lower Aβ42, and higher t-tau and p-tau in AD patients. Moreover, CSF pressure was significantly lower in AD group (11.0 ± 2.8 vs. 13.3 ± 3.0 mmHg, p < 0.05) and directly correlated with Aβ42 levels (R = 0.512; p < 0.05), but not with other biomarkers or parameters. No significant correlations emerged for biomarkers in control group. AD patients exhibit low CSF pressure whose values are directly and selectively related to CSF Aβ42 levels. This interesting correlation may confirm in vivo the association between CSF dynamic and beta-amyloid metabolism occurring in AD.


Similar content being viewed by others
References
Bell RD, Zlokovic BV (2009) Neurovascular mechanisms and blood–brain barrier disorder in Alzheimer’s disease. Acta Neuropathol 118(1):103–113
Blennow K et al (2010) Cerebrospinal fluid and plasma biomarkers in Alzheimer disease. Nat Publ Group 6(3):131–144
Blennow K et al (2016) Cerebrospinal fluid biomarkers in Alzheimer’s and Parkinson’s diseases—from pathophysiology to clinical practice. Mov Disord 31(6):836–847
Brinker T et al (2014) A new look at cerebrospinal fluid circulation. Fluids Barriers CNS 11(1):10
Dorr A et al (2012) Amyloid-β-dependent compromise of microvascular structure and function in a model of Alzheimer’s disease. Brain 135(Pt 10):3039–3050
Dubois B et al (2007) Research criteria for the diagnosis of Alzheimer’s disease: revising the NINCDS-ADRDA criteria. Lancet Neurol 6(8):734–746
Friedman DI, Liu GT, Digre KB (2013) Revised diagnostic criteria for the pseudotumor cerebri syndrome in adults and children. Neurology 81(13):1159–1165
Iadecola C (2003) Cerebrovascular effects of amyloid-beta peptides: mechanisms and implications for Alzheimer’s dementia. Cell Mol Neurobiol 23(4–5):681–689
Iliff JJ et al (2012) A paravascular pathway facilitates CSF flow through the brain parenchyma and the clearance of interstitial solutes, including amyloid. Sci Transl Med 4(147):147ra111
Jessen NA et al (2015) The glymphatic system: a beginner’s guide. Neurochem Res 40(12):2583–2599
Karran E, Mercken M, De Strooper B (2011) The amyloid cascade hypothesis for Alzheimer’s disease: an appraisal for the development of therapeutics. Nat Rev Drug Discov 10(9):698–712
Li H, Wolfe MS, Selkoe DJ (2009) Toward structural elucidation of the γ-secretase complex. Structure 17(3):326–334
Li H et al (2014) Vascular and parenchymal amyloid pathology in an Alzheimer disease knock-in mouse model: interplay with cerebral blood flow. Mol Neurodegener 9(1):28
Martorana A et al (2015) Cerebrospinal fluid Aβ42 levels: when physiological become pathological state. CNS Neurosci Ther 21(12):921–925
Preston SD et al (2003) Capillary and arterial cerebral amyloid angiopathy in Alzheimer’s disease: defining the perivascular route for the elimination of amyloid beta from the human brain. Neuropathol Appl Neurobiol 29(2):106–117
Sagare AP, Bell RD, Zlokovic BV (2013) Neurovascular defects and faulty amyloid-β vascular clearance in Alzheimer’s disease. J Alzheimer’s Dis 33(Suppl 1):S87–S100
Scheltens P, Blennow K, Breteler MM, de Strooper B, Frisoni GB, Salloway S, Van der Flier WM (2016) Alzheimer’s disease. Lancet 388(10043):505–517
Schirinzi T et al (2015) A clinical and biochemical analysis in the differential diagnosis of idiopathic normal pressure hydrocephalus. Front Neurol 6:86
Silverberg GD et al (2001) The cerebrospinal fluid production rate is reduced in dementia of the Alzheimer’s type. Neurology 57(10):1763–1766
Silverberg GD et al (2003) Alzheimer’s disease, normal-pressure hydrocephalus, and senescent changes in CSF circulatory physiology: a hypothesis. Lancet Neurol 2(8):506–511
Silverberg G et al (2006) Elevated cerebrospinal fluid pressure in patients with Alzheimer’s disease. Cerebrospinal Fluid Res 3(1):7
Simon MJ, Iliff JJ (2016) Regulation of cerebrospinal fluid (CSF) flow in neurodegenerative, neurovascular and neuroinflammatory disease. Biochim Biophys Acta 1862(3):442–451
Sun X et al (2006) Hypoxia facilitates Alzheimer’s disease pathogenesis by up-regulating BACE1 gene expression. Proc Natl Acad Sci 103(49):18727–18732
Tapiola T et al (2009) Cerebrospinal fluid {beta}-amyloid 42 and tau proteins as biomarkers of Alzheimer-type pathologic changes in the brain. Arch Neurol 66(3):382–389
Tarasoff-Conway JM et al (2015) Clearance systems in the brain-implications for Alzheimer disease. Nat Rev Neurol 11(8):457–470
Thomas T et al (1996) β-Amyloid-mediated vasoactivity and vascular endothelial damage. Nature 380(6570):168–171
Toombs J et al (2017) Effect of spinal manometers on cerebrospinal fluid amyloid-β concentration. J Alzheimer’s Dis 56(3):885–891
van Waalwijk van Doorn LJC et al (2017) Improved cerebrospinal fluid-based discrimination between Alzheimer’s disease patients and controls after correction for ventricular volumes. J Alzheimer’s Dis 56(2):543–555
Wallin AK et al (2010) CSF biomarkers predict a more malignant outcome in Alzheimer disease. Neurology 74(19):1531–1537
Whiteley W et al (2006) CSF opening pressure: reference interval and the effect of body mass index. Neurology 67(9):1690–1691
Wostyn P, Audenaert K, De Deyn PP (2009) More advanced Alzheimer’s disease may be associated with a decrease in cerebrospinal fluid pressure. Cerebrospinal Fluid Res 6:14
Zhang C, Saunders AJ (2007) Therapeutic targeting of the alpha-secretase pathway to treat Alzheimer’s disease. Discov Med 7(39):113–117
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
No funding has been received for this study.
Conflict of interest
All authors declare no conflicts of interests.
Rights and permissions
About this article
Cite this article
Schirinzi, T., Di Lazzaro, G., Sancesario, G.M. et al. Levels of amyloid-beta-42 and CSF pressure are directly related in patients with Alzheimer’s disease. J Neural Transm 124, 1621–1625 (2017). https://doi.org/10.1007/s00702-017-1786-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00702-017-1786-8