Abstract
Objective
Right ventricular function (RVF) is a strong predictor of adverse cardiac events; however, the reference standard for RVF assessment, MRI, is limited in some patients for whom accurate evaluation of RVF is essential, like those with COPD or non-MR compatible metal implants. We conducted this meta-analysis to evaluate whether CT was as accurate as MRI for the assessment of RVF.
Method
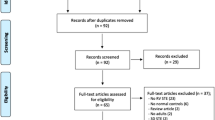
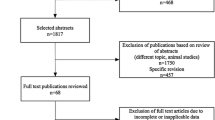
We conducted a meta-analysis of studies retrieved from PubMed, Embase, and Cochrane Central searches to evaluate the differences and correlations between the following RVF parameters as measured by CT and MRI: end diastole volume (EDV), end systole volume (ESV), right ventricular ejection fraction (RVEF), and stroke volume (SV).
Results
Sixteen studies that used disk summation (637 subjects) and three studies that used three-dimensional reconstruction were included. For the 16 studies, the pooled standard mean differences (95% confidence interval) were 1.04 (− 2.59, 4.67) for EDV, 1.22 (1.50, 3.95) for ESV, − 0.65 (− 2.60, 1.29) for RVEF, and − 0.37 (− 3.64, 2.90) for SV. The overall correlation coefficient (r) values were 0.98 for EDV, 0.95 for ESV, 0.98 for RVEF, and 0.97 for SV. The mean difference between the two methods was not statistically significant (overall effect Z test, p > 0.1).
Conclusion
CT can assess RVF with accuracy comparable to that of MRI. Thus, CT is a valid alternative to MRI.
Key Points
• CT could help clinicians to assess RVF as accurately as MRI can, with satisfactory repeatability.






Similar content being viewed by others
Change history
25 March 2020
The original version of this article, published on 27 May 2019, unfortunately contained mistakes.
Abbreviations
- CI:
-
Confidence interval
- CT:
-
Computed tomography
- EDV:
-
End diastole volume
- ESV:
-
End systole volume
- LOA:
-
Limit of agreement
- MD:
-
Mean difference
- MR:
-
Magnetic resonance
- MRI:
-
Magnetic resonance imaging
- QUADAS:
-
The Quality Assessment of Diagnostic Studies
- RV:
-
Right ventricular
- RVEF:
-
Right ventricular ejection fraction
- RVF:
-
Right ventricular function
- SD:
-
Standard deviation
- SV:
-
Stroke volume
- TR:
-
Temporary resolution
References
Haddad F, Doyle R, Murphy DJ, Hunt SA (2008) Right ventricular function in cardiovascular disease, part II: pathophysiology, clinical importance, and management of right ventricular failure. Circulation 117:1717–1731
Zornoff LA, Skali H, Pfeffer MA et al (2002) Right ventricular dysfunction and risk of heart failure and mortality after myocardial infarction. J Am Coll Cardiol 39:1450–1455
Dini FL, Conti U, Fontanive P et al (2007) Right ventricular dysfunction is a major predictor of outcome in patients with moderate to severe mitral regurgitation and left ventricular dysfunction. Am Heart J 154:172–179
Juillière Y, Barbier G, Feldmann L, Grentzinger A, Danchin N, Cherrier F (1997) Additional predictive value of both left and right ventricular ejection fractions on long-term survival in idiopathic dilated cardiomyopathy. Eur Heart J 18:276–280
de Groote P, Millaire A, Foucher-Hossein C et al (1998) Right ventricular ejection fraction is an independent predictor of survival in patients with moderate heart failure. J Am Coll Cardiol 32:948–954
Borer JS, Hochreiter CA, Supino PG, Herrold EM, Krieger KH, Isom OW (2002) Importance of right ventricular performance measurement in selecting asymptomatic patients with mitral regurgitation for valve surgery. Adv Cardiol 39:144–152
Patscheider H, Lorbeer R, Auweter S et al (2018) Subclinical changes in MRI determined right ventricular volumes and function in subjects with prediabetes and diabetes. Eur Radiol 28:3105–3113
Meune C, Khanna D, Aboulhosn J et al (2016) A right ventricular diastolic impairment is common in systemic sclerosis and is associated with other target-organ damage. Semin Arthritis Rheum 45:439–445
Hoffmann R, Barletta G, von Bardeleben S et al (2014) Analysis of left ventricular volumes and function: a multicenter comparison of cardiac magnetic resonance imaging, cine ventriculography, and unenhanced and contrast-enhanced two-dimensional and three-dimensional echocardiography. J Am Soc Echocardiogr 27:292–301
Moon JC, Lorenz CH, Francis JM, Smith GC, Pennell DJ (2002) Breath-hold FLASH and FISP cardiovascular MR imaging: left ventricular volume differences and reproducibility. Radiology 223:789–797
Barkhausen J, Ruehm SG, Goyen M, Buck T, Laub G, Debatin JF (2001) MR evaluation of ventricular function: true fast imaging with steady-state precession versus fast low-angle shot cine MR imaging: feasibility study. Radiology 219:264–269
Miller JD, Nazarian S, Halperin HR (2016) Implantable electronic cardiac devices and compatibility with magnetic resonance imaging. J Am Coll Cardiol 68:1590–1598
Barkhausen J, Ruehm SG, Goyen M, Buck T, Laub G, Debatin JF (2016) Bias associated with left ventricular quantification by multimodality imaging: a systematic review and meta-analysis. Open Heart 3:e388
Pickett CA, Cheezum MK, Kassop D, Villines TC, Hulten EA (2015) Accuracy of cardiac CT, radionucleotide and invasive ventriculography, two- and three-dimensional echocardiography, and SPECT for left and right ventricular ejection fraction compared with cardiac MRI: a meta-analysis. Eur Heart J Cardiovasc Imaging 16:848–852
Moher D, Liberati A, Tetzlaff J, Altman DG, PRISMA Group (2009) Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. BMJ 339:b2535
Bland JM, Altman DG (1986) Statistical methods for assessing agreement between two methods of clinical measurement. Lancet 1:307–310
Whiting P, Rutjes AW, Reitsma JB, Bossuyt PM, Kleijnen J (2003) The development of QUADAS: a tool for the quality assessment of studies of diagnostic accuracy included in systematic reviews. BMC Med Res Methodol 3:25
Fisher RA (1915) Frequency distribution of the values of the correlation coefficients in samples from an indefinitely large population. Biometrika 10:507–521
Guo YK, Gao HL, Zhang XC, Wang QL, Yang ZG, Ma ES (2010) Accuracy and reproducibility of assessing right ventricular function with 64-section multi-detector row CT: comparison with magnetic resonance imaging. Int J Cardiol 139:254–262
Jensen CJ, Wolf A, Eberle HC et al (2011) Accuracy and variability of right ventricular volumes and mass assessed by dual-source computed tomography: influence of slice orientation in comparison to magnetic resonance imaging. Eur Radiol 21:2492–2502
Plumhans C, Mühlenbruch G, Rapaee A et al (2008) Assessment of global right ventricular function on 64-MDCT compared with MRI. AJR Am J Roentgenol 190:1358–1361
Koch K, Oellig F, Oberholzer K et al (2005) Assessment of right ventricular function by 16-detector-row CT: comparison with magnetic resonance imaging. Eur Radiol 15:312–318
Zhang XC, Yang ZG, Guo YK et al (2012) Assessment of right ventricular function for patients with rheumatic mitral stenosis by 64-slice multi-detector row computed tomography: comparison with magnetic resonance imaging. Chin Med J (Engl) 125:1469–1474
Huang X, Pu X, Dou R et al (2012) Assessment of right ventricular function with 320-slice volume cardiac CT: comparison with cardiac magnetic resonance imaging. Int J Cardiovasc Imaging 28:87–92
Fuchs A, Kühl JT, Lønborg J et al (2012) Automated assessment of heart chamber volumes and function in patients with previous myocardial infarction using multidetector computed tomography. J Cardiovasc Comput Tomogr 6:325–334
Schroeder J, Peterschroeder A, Vaske B et al (2009) Cardiac volumetry in patients with heart failure and reduced ejection fraction: a comparative study correlating multi-slice computed tomography and magnetic resonance tomography. Reasons for intermodal disagreement. Clin Res Cardiol 98:739–747
Elgeti T, Lembcke A, Enzweiler CN, Breitwieser C, Hamm B, Kivelitz DE (2004) Comparison of electron beam computed tomography with magnetic resonance imaging in assessment of right ventricular volumes and function. J Comput Assist Tomogr 28:679–685
Gao Y, Du X, Liang L, Cao L, Yang Q, Li K (2012) Evaluation of right ventricular function by 64-row CT in patients with chronic obstructive pulmonary disease and cor pulmonale. Eur J Radiol 81:345–353
Müller M, Teige F, Schnapauff D, Hamm B, Dewey M (2009) Evaluation of right ventricular function with multidetector computed tomography: comparison with magnetic resonance imaging and analysis of inter- and intraobserver variability. Eur Radiol 19:278–289
Wang L, Zhang Y, Yan C et al (2013) Evaluation of right ventricular volume and ejection fraction by gated 18F-FDG PET in patients with pulmonary hypertension: comparison with cardiac MRI and CT. J Nucl Cardiol 20:242–252
Maffei E, Messalli G, Martini C et al (2012) Left and right ventricle assessment with cardiac CT: validation study vs cardiac MR. Eur Radiol 22:1041–1049
Raman SV, Shah M, McCarthy B, Garcia A, Ferketich AK (2006) Multi–detector row cardiac computed tomography accurately quantifies right and left ventricular size and function compared with cardiac magnetic resonance. Am Heart J 151:736–744
Sugeng L, Mor-Avi V, Weinert L et al (2010) Multimodality comparison of quantitative volumetric analysis of the right ventricle. JACC Cardiovasc Imaging 3:10–18
Lembcke A, Dohmen PM, Dewey M et al (2005) Multislice computed tomography for preoperative evaluation of right ventricular volumes and function: comparison with magnetic resonance imaging. Ann Thorac Surg 79:1344–1351
Takx RA, Moscariello A, Schoepf UJ et al (2012) Quantification of left and right ventricular function and myocardial mass: comparison of low-radiation dose 2nd generation dual-source CT and cardiac MRI. Eur J Radiol 81:e598–e604
Yamasaki Y, Nagao M, Yamamura K et al (2014) Quantitative assessment of right ventricular function and pulmonary regurgitation in surgically repaired tetralogy of Fallot using 256-slice CT: comparison with 3-tesla MRI. Eur Radiol 24:3289–3299
Guo YK, Yang ZG, Shao H, Deng W, Ning G, Dong ZH (2013) Right ventricular dysfunction and dilatation in patients with mitral regurgitation: analysis using ECG-gated multidetector row computed tomography. Int J Cardiol 167:1585–1590
Jennifer L, Lezotte DC, Weitzenkamp DA, Allen LA, Salcedo EE (2012) Performance of 3-dimensional echocardiography in measuring left ventricular volumes and ejection fraction: a systematic review and meta-analysis. J Am Coll Cardiol 59:1799–1808
Peng P, Lekadir K, Gooya A, Shao L, Petersen SE, Frangi AF (2016) A review of heart chamber segmentation for structural and functional analysis using cardiac magnetic resonance imaging. MAGMA 29:155–195
Yang WJ, Chen KM, Liu B et al (2013) Contrast media volume optimization in high-pitch dual- source CT coronary angiography: feasibility study. Int J Cardiovasc Imaging 29:245–252
Burghard P, Plank F, Beyer C et al (2018) Evaluation of right ventricular function by coronary computed tomography angiography using a novel automated 3D right ventricle volume segmentation approach: a validation study. Eur Radiol 28:5129–5136
Gutberlet M, Schwinge K, Freyhardt P et al (2005) Influence of high magnetic field strengths and parallel acquisition strategies on image quality in cardiac 2D CINE magnetic resonance imaging: comparison of 1.5 T vs. 3.0 T. Eur Radiol 15:1586–1597
Santoro F, Ieva R, Di Biase M, Brunetti ND (2015) Long live β-blockers in Takotsubo outflow obstruction! Rather with a short half-life. Can J Cardiol 31:1074–1077
Oda S, Katahira K, Utsunomiya D et al (2015) Improved image quality at 256-slice coronary CT angiography in patients with a high heart rate and coronary artery disease: comparison with 64-slice CT imaging. Acta Radiol 56:1308–1314
Funding
This work was supported by the National Natural Science Foundation of China (81471722, 81771887, 81471721, 81771897) and Program for Young Scholars and Innovative Research Team in Sichuan Province of China (2017TD0005).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Guarantor
The scientific guarantor of this publication is Ying-kun Guo.
Conflict of interest
The authors report no conflicts of interest.
Statistics and biometry
No complex statistical methods were necessary for this paper.
Informed consent
Written informed consent was not required for this study because it is a meta-analysis.
Ethical approval
Institutional Review Board approval was not required because of the meta-analysis study design.
Study subjects or cohorts overlap
Study subjects and cohorts have been reported previously as detailed in the methods and results as well as reference.
Methodology
• Performed at one institution
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
ESM 1
(DOCX 22.5 kb)
Rights and permissions
About this article
Cite this article
Fu, H., Wang, X., Diao, K. et al. CT compared to MRI for functional evaluation of the right ventricle: a systematic review and meta-analysis. Eur Radiol 29, 6816–6828 (2019). https://doi.org/10.1007/s00330-019-06228-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00330-019-06228-2